Patients
- Prospective study of 11 patients with PBL proven histologically,
enrolled in our University Hospital center from January 2009 to December 2011.
- All the patients were immunocompetent.
The mean age was 53 years.
In other publications,
PBL usually occurred in the sixth decade [5].
- They had a variety of symptoms including :
Signs of increased intracranial pressure (n=8),
focal neurological deficits (n=5),
and signs of Coma (n=3).
Imaging analysis (our study)
MRI study of the brain was performed in all the patients either immediately or after a cranial CT scan (n=8).
MRI evaluation was done on a 1,5T,
including conventional sequences,
diffusion-weighted sequences,
MR spectroscopy (MRS) and MR perfusion.
_ Location :
- Most lesions are supratentorial (n=9),
- periventricular locations (n=5),
- both fronto-parietal lobes were observed in 2 cases,
- and leptomeningeal involvement was found in one patient.
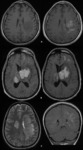
_ Characteristic of MRI findings :
- Predominance of lesions with intense enhancement,
- DWI: Restricted diffusion with low ADC values,
- MRS: elevated lipid and lactate peaks and decreased in the NAA peak.
- No necrosis lesion was detected.
Histological confirmation was obtained using stereotactic biopsy.
These findings will be widely compared to proven literature data:
General Features [1,6]
Best diagnostic clue: Enhancing lesion within basal ganglia,
and periventricular white matter.
_ Location:
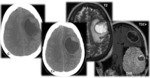
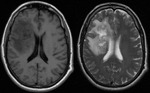
- 90% supra tentorial : Frontal and parietal lobes most common (Figure 1),
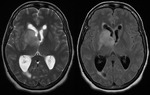
- Deep gray nuclei commonly affected (Figure 2),
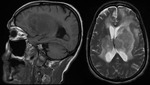
- Lesions cluster around ventricles (Figure 3),
GM-WM junction,
- Often involve,
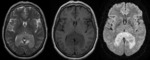
cross corpus callosum (Figures 4,
5),
- Frequently abut,
extend along ependymal surfaces (Figure 5),
- Infratentorial,
sellar,
pineal region uncommon,
- May involve leptomeninges or dura,
more commonly in secondary lymphoma (Figure 6).
_ Morphology
- Multiple lesions (Figure 7) or solitary mass (Figure 8),
- May be circumscribed (Figure 8) or infiltrative (Figure 5).
Most lesions are supratentorial,
and involve central hemispheric or periventricular white matter.
Proximity to the sub arachnoid / subependymal space is a common finding and may provide a diagnostic clue (Figure 9).
The sites of involvement include: frontal lobe (20- 43 %) (Figure 9),
basal ganglia (13- 20%): (Figures 2,
3),
corpus callosum (10%) (Figure 4),
posterior fossa (13%) and the spinal cord,
in only 1%–2% of patients [6].
Primary dural lymphoma is a rare subtype of PCNSL that differs biologically from other PCNSLs because it arises from the dura mater [7].
PCNSL May rarely involve leptomeninges,
retina,
vitreous humour and optic nerve.
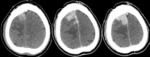
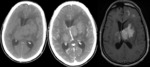
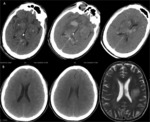
CT Findings(Figures 7,
10):
• Non-Enhanced CT:
A round or oval iso-/ hyper dense lesion.
A negative CT examination does not exclude CNS lymphoma and there is a reported 13-38% false-negative rate (Figure 10 B)
• Contrast-Enhanced CT:
Common: moderate-to-marked contrast enhancement [6]
Uncommon: heterogeneous or absent contrast enhancement.
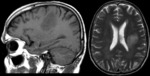
MR Findings
1.
T1 :
Hypo- or iso intense lesions (Figures 1,
2).
2.
T2:
- Hyper or iso-intense (Figures 1,
2).
- Mild surrounding edema is typical (Figure 11).
3.
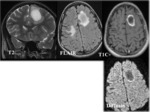
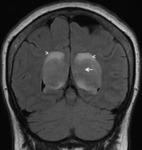
FLAIR (Figure 12):
- Homogeneous,
isointense/hypointense to cortex.
May be hyperintense.
- Mild surrounding edema is typical.
4.
DWI (Figures 4):
- Because PBLs are highly cellular tumors,
water diffusion is often restricted,
making them appear hyperintense on DWI
- and hypointense on ADC maps [8].
5.
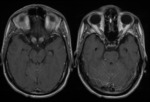
T1 C+ (Figure 13):
- Common: moderate to marked contrast enhancement.
- Uncommon: heterogeneous or absent contrast enhancement.
- The pattern of enhancement could be categorized as solid,
irregular,
linear (Figure 9),
punctate,
patchy and rim (ring)-like [9].
6.
T2*GRE (Figure 14):
- Hemorrhage or internal calcification within the tumor is quite a rare finding [9].
- May see blood products or calcium as areas of "blooming" (immunocompromised)
7.
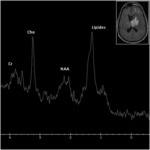
Magnetic resonance spectroscopy (Figures 15,
16):
- MRS provides information on metabolic change in vivo.
It demonstrates an exaggerated lipid peak in a solid mass with high Choline /Creatine ratios.
- Elevation of lipid peak is typically a signature of cell death; however,
a lipid-dominated spectrum is found in PCNSL that is not macroscopically necrotic and due to macrophage content [10,
11].
8.
MR perfusion [12,
13]:
- PBLs demonstrate low cerebral blood volume (CBV) [Figure 17] and a characteristic intensity time curve,
which is related to a massive leakage of contrast media into the interstitial space (Figures 18 and 19 from [14,
15]).
Furthermore,
maximum relative CBV (rCBV) measured in tumor tissue,
calculated as a ratio to contralateral normal-appearing WM,
is typically lower in lymphomas than in other brain tumors.
This characteristic finding can help to differentiate glioblastomas and metastases from lymphomas.
In one study,
rCBV of PBLs was 1.72,
while that of high-grade gliomas was 4.86.
In another study,
primary and secondary CNSLs showed relatively low values for the maximum rCBV ratio.
- MR perfusion should be measured before steroid administration at it induces a reduction in blood tumour barrier permeability and regional cerebral blood volume.
BRAIN BIOPSY
Stereotactic brain biopsy is the most appropriate method for the diagnosis of PBL.
However,
open brain biopsy may be necessary in those patients who have lesions located in areas of the brain that are difficult to access (eg,
brainstem).
If possible,
the procedure should be performed before corticosteroids have been administered.
In summary,
a stereotactic-guided biopsy for multiple or deep-seated lymphomas is a safe operative procedure with minimal morbidity and no mortality.
DIFFERENTIAL DIAGNOSIS
1.
Glioblastoma multiforme (Figure 20):
- "Butterfly glioma" involving corpus callosum,
- Hemorrhage common,
- Enhancement typically heterogeneous,
- Necrosis with ring enhancement in 95%,
- PBLs lesions often have more restricted diffusion and lower ADC values than high-grade gliomas.
2.
Demyelination: Demyelinating pseudotumor(Figure 21):
- Younger patients,
- May involve corpus callosum,
- Often incomplete,
"horseshoe-shaped" enhancement open towards cortex.
3.
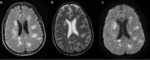
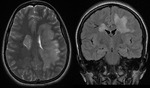
Acute disseminated encephalomyelitis (Figure 22):
- Acute disseminated encephalomyelitis (ADEM) is an acute,
monophasic inflammatory demyelinating disease affecting the CNS,
which usually follows an infection or vaccination.
The disease is characterised by multifocal WM lesions on neuroimaging.
- CT Scan is generally normal at onset and usually becomes abnormal 5–14 days later.
The typical computed tomographic appearance is that of low attenuation,
multifocal lesions in the subcortical WM.
- Demyelinating lesions of ADEM are better visualised by MRI,
which usually exhibit no mass effect and can be seen scattered throughout the white matter of the posterior fossa and cerebral hemispheres.
Involvement of the cerebellum and brainstem is more common in children.
- Characteristic lesions seen on MRI appear as patchy areas of increased signal intensity on conventional T2-weighted images and on FLAIR sequence.
Few MRI lesions may enhance after gadolinium administration.
Extensive perifocal oedema may be seen.
4.
Secondary CNS Lymphoma (Figure 23):
- Typical location: Leptomeninges +++
- Superficial cerebral lesion; communicating hydrocephalus.
- Leptomeningeal,
subependymal,
dural,
or cranial nerve contrast enhancement.

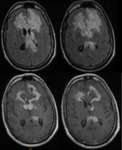
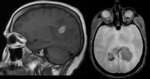

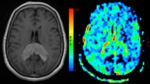
![Fig. 18: multimodal MRI of a large deep right frontal periventricular lesion, showing a strong homogeneous enhancement with peripheral oedema. MRI perfusion indicates increasing of the intensity of the signal above the baseline attesting the high blood-brain barrier permeability with no significant neoangiogenesis [14]. References: 14. Houillier C, Gonzalez-Aguilar A, Hoang-Xuan K. Lymphome cérébral primitif chez un sujetimmunocompétent. Pratique Neurologique – FMC 2012;3:40 –44](https://epos.myesr.org/posterimage/esr/ecr2013/115125/media/510236?maxheight=150&maxwidth=150)
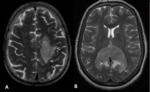
![Fig. 19: Multimodality cerebral MRI of a middle-aged man with a PCNS lymphoma. T1 WI with contrast showing a homogeneous enhancing of two lesions in contact with the ventricles. MRI perfusion of the major lesion shows a weak increase of relative cerebral blood volume, which indicates no significant localized neoangiogenesis (no red area in the lesion). The first pass of the bolus agent curve indicates high blood-brain barrier permeability [15]. References: Ricard D, Idbaih A, Ducray F, Lahutte M, Hoang-Xuan K, Delattre J.Y. Primary brain tumours in adults. Lancet 2012; 379: 1984–96](https://epos.myesr.org/posterimage/esr/ecr2013/115125/media/510237?maxheight=150&maxwidth=150)