Survival
Median survival was 105 weeks,
with 1 year,
2 year and 3-year survival 95.5%,
89.9% and 77.7% respectively.
Patients who had a total number of tumour lesions ≥ 3 ablated were found to have a mean survival of 150 weeks,
compared to 195 weeks in those with a total number of lesions ≤ 2.
This almost reached statistical significance (p=0.091) (figures 1 and 2).
The following variables were not statistically significant (table 1): mean maximum tumour size; initial number of tumours ablated; whether the lesions were unilateral or bilateral; total number of RFA procedures performed; the presence of metastases at additional sites; pre-RFA chemotherapy; site of primary tumour.
Tumour Recurrence
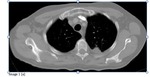
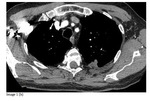
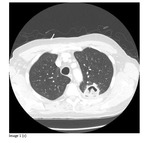
17% of the lesions developed evidence of recurrence,
with mean and median time to recurrence 32 and 30 (range 7 - 65) weeks respectively (Images 1a-c)
40% of recurrences occurred when the lesions were abutting segmental pulmonary arteries or larger vessels,
including the thoracic aorta and superior vena cava.
Two of the patients who developed recurrence had suboptimal ablation.
The first experienced an episode of bradycardia requiring atropine and had the procedure aborted; the second received inadequate analgesia and sedation so was unable to tolerate the ablation.
53% of the recurring lesions underwent repeat radiofrequency ablation.
Only one demonstrated recurrence after second RFA,
with a time to recurrence of 66 weeks.
Thus,
the secondary (after repeat ablations) effectiveness rate was 90.7% (78 of 86 lesions without tumour progression at the end of follow-up).
Complications
The significant complication rate was 12%.
Pneumothorax requiring insertion of a percutaneous chest drain occurred in a total of 6 ablation treatments.
There were 3 cases of pleural effusion requiring drainage,
while one patient developed a post-procedure pneumonia.
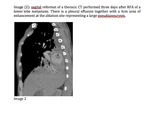
One patient who underwent right lower lobe RFA developed a large false aneurysm in a right lower lobe artery (Image 2).
This was treated by coil embolisation.
A further patient developed significant chest wall pain,
probably due to intercostal nerve damage.
The thirty-day mortality rate following RFA was 0%.