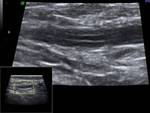
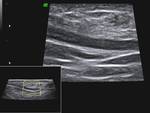
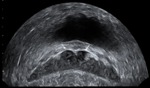
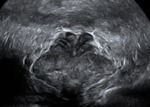
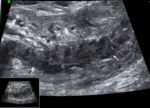
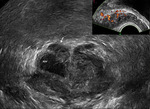
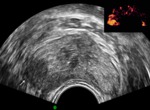
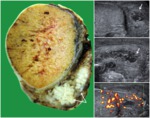
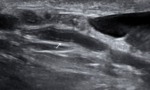
In the control group VD identified as incompressible,
hypoechoic and layered tubular anatomical structure,
which occupies a marginal position in the spermatic cord,
having a clear external contours and regular sizes.
Outer diameter and internal structure of the VD does not depend on the age,
body mass index,
sizes the testicles and prostate.
Visualization were available all the anatomical parts of the VD,
except in the pelvic region.
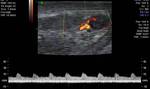
Density intraductal blood flow at Power Doppler was 0 (0 - 1) signals to cross-sectional area of VD.
Blood flow in the artery VD characterized as a low speed and high-resistance (Fig 1 - 5).
AND was diagnosed in 54 (63%) of 86 patients with acute scrotum.
The age distribution of patients had a bimodal character (Fig.
6).
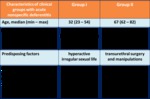
The 1rst subgroup (n = 42) comprised patients young and middle-age,
in the 2nd subgroup (n = 12) consisted of patients of elderly and senile age.
In the 1st subgroup the AND mainly developed at sexually transmitted infections (trichomoniasis,
chlamydiasis and other),
in the 2nd subgroup the AND often occurred after various transurethral surgery and manipulations on prostate and bladder at gram-negative infection (E.
coli,
Proteus mirabilis and other).
In both subgroups development AND preceded inflammatory diseases of the urogenital organs: acute urethritis – in 8 (15%) patients,
acute prostatitis – in 13 (24%),
acute seminal vesiculitis – in 18 (33%) or a combination of these diseases – in 15 (28%) (Fig 7 - 8).
Clinical laboratory signs of the AND were non-specific and they simulated acute epididymitis.
They included acute pain in the scrotum – in 54 (100%) patients,
swelling and hyperemia scrotum – in 28 (52%),
asymmetric increase scrotum – in 14 (26%),
general signs of inflammation (fever,
leukocytosis,
increase ESR) - in 51 (94%).
Palpation the VD was non-informative test because of the expressed pain and swelling of the scrotum in 52 (96%) patients.
When clinical and laboratory evaluation of patients the AND was detected only in 6 (12%).
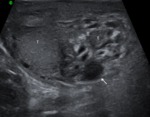
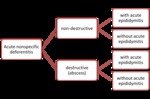
According to high-resolution ultrasound the AND characterized by:
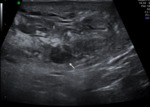
a) indistinct external outlines the VD in 54 (100%) patients;
b) thickening the VD over 5 mm – in 52 (96%);
c) poor differentiation of the layers VD - in 54 (100%);
d) heterogeneous structure the VD – in 42 (78%);
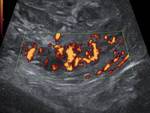
e) intraductal and periductal hyoervascularization – in 54 (100%).
Blood flow in the artery of the VD was high-speed and low-resistance.
Vascular density the VD was 5,6 (3 - 8) (Fig.
9 - 13).
The AND usually combined with the acute epididymitis in 40 (74%) patients,
less often the AND preceded the acute epididymitis – in 8 (15%).
Very rarely it has developed in isolation as an independent disease - in 6 (11%) patients (Fig.
14).
As a rule,
the AND limited to defeat by epididymal part of the VD.
In 2 (4%) cases was noted involvement in the inflammatory process of the terminal and of the inguinal parts the VD.
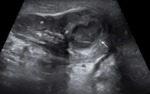
Destructive form of the AND was observed in 8 (15%) patients.
In these patients,
ultrasound were found small abscesses the VD dimensions of 3,2 (2,6 - 5,3) mm in diameter.
Abscesses of the VD combined with destructive changes of the epididymis and testis in all cases and treated surgically.
In 2 (25%) patients with destructive forms of the AND the abscesses VD identified previously by ultrasonography,
however,
in during the operation they were not found,
the operation was limited to only by epididymectomy.
In the postoperative period,
the status of the patients are not improved.
The ultrasonography confirmed the presence of the abscess VD with the spread of the inflammatory process on the testicle.
It was rescheduled forced and advanced surgical intervention: orchiectomy (Fig.
15 - 17).
The clinical and ultrasound differencial criteria the AND are presented in figures 18 -19.
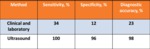
The sensitivity,
the specificity and the diagnostic accuracy of high-resolution ultrasound at the AND were 100%,
96% and 98%,
respectively (Fig.
20).