TRANSABDOMINAL ULTRASONOGRAPHY
Background
Transabdominal Ultrasonography (US) represents the first choice modality for evaluating gallbladder diseases.
The accuracy of US in diagnosing GA,
and in particular in differentiating GA from gallbladder cancer,
has progressively increased during the years (from 66.0% in year 2001 to 92.7% in year 2013),
mainly as a consequence of technical improvements of US scanners: i.e.
high frequency transducers,
harmonics,
compounding techniques and speckle reduction imaging.
US findings
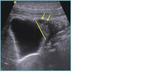
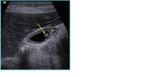
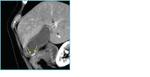
- Focal or diffuse gallbladder wall thickening (Fig 2, line)can be easily highlighted at US and represents the direct consequence of epithelial hyperplasia and muscular layer hypertrophy.
It is always present in GA,
but it is not pathognomonic for it.
A cleavage plane with the liver must be always present.
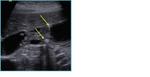
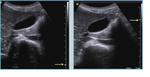
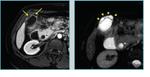
- Small anechoic cystic spaces (Fig 2-3, arrows)within the thickened gallbladder wall represent clear-bile filled RAS and must be accurately searched because they are pathognomonic for gallbladder adenomyomatosis; indeed,
if cystic RAS are visualized, the diagnosis of GA is sure.
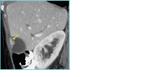
- Intramural echogenic spots (Fig 4, arrows) without or withacoustic shadowing,
are the consequence of cholesterine crystals- or dystrophic calcifications-filled RAS,
respectively.
Their presence is virtually pathognomonic for gallbladder adenomyomatosis.
- Reverberation artifacts (Fig 5, arrowheads) are the consequence of the coexistence of different acoustic impedance media,
i.e.
clear bile and cholesterine crystals,
within RAS.
They appear as hyperechoic “comet-tail” artifacts that project deeply to Rokitansky-Aschoff sinuses,
but RAS theirselves may be sometimes not directly recognizable at the origin of reverberation artifacts.
Their presence is strongly associated with gallbladder adenomyomatosis.
- Twinkling artifacts on color-Doppler sonography (Fig 6)are due to the interaction of the ultrasound beam with an acoustic interface composed by randomly disposed strongly reflecting media (i.e.
cholesterine crystals or calcifications) which generate a rough interface.
Twinkling artifacts appear as rapidly alternating red and blue color-Doppler signals,
“comet-tail” shaped,
deeply to RAS.
The presence of twinkling artifacts is strongly associated with gallbladder adenomyomatosis.
Tips & tricks
- Focus adjustment (Fig 7). A precise focal depth adjustment (arrow) is crucial in order to correctly investigate every portion of gallbladder wall for the presence of gallbladder adenomyomatosis.
In particular,
it is often necessary to bring the focal point to very superficial positions (b) in order to highlighting fundal type GA.
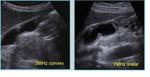
- High frequency US (Fig 8). Gallbladder adenomyomatosis often involves gallbladder fundus,
a region that may be unsatisfactory investigated by means of the 4-5MHz convex abdominal probes (a); every suspect finding in this area must be further investigated by means of high frequency (7-9MHz) linear probes (b) in order to better characterize it.
- Harmonic imaging. The utilization of harmonic imaging significantly increases the accuracy of US in depicting gallbladder wall morphology and in recognizing Rokitansky-Aschoff sinuses,
compared to non-harmonic imaging.
- Hepatic window. Sometimes fundal adenomyomatosis might be poorly delimitable by means of the classical sub-costal approach,
particularly in obese patients; hepatic parenchyma inclusion between the probe and the gallbladder fundus,
that can be usually achieved by means of an trans-costal approach,
significantly increases image quality in these cases.
Pitfalls & limitations
- Cholesterine polyps (Fig 9) are sometimes counfounded with GA,
whereas they represent a completely different entity.
Polyos (arrow) and adenomyomatosis (star) may coexist in some patients.
- US is an extremely operator-dependent imaging modality and the ability in depicting GA varies according to the operator’s experience.
Moreover,
sonographic examination may be limited by obesity and bowel gas interposition.
- Contrast material administration (CEUS) does not increase US accuracy in depicting gallbladder adenomyomatosis and its use is not justified.
Indications
US is the imaging modality of choice in the suspicion of gallbladder adenomyomatosis.
If a confident diagnosis of GA cannot be reached at US,
MR must be considered the second level imaging modality of choice.
MAGNETIC RESONANCE
Background
Magnetic Resonance (MR) has become nowadays widely available and,
thanks to its multiplanarity and to its high tissue contrast resolution,
it is becoming an increasingly requested imaging modality for hepato-biliary pathology.
On the other hand,
MR remains a time- and resource-consuming imaging modality and,
therefore,
the indications for its performance must be accurately evaluated.
MR is the imaging technique that offers the highest accuracy in diagnosing GA,
in particular in differentiating GA from gallbladder carcinoma (accuracy 93.0%).
At MR,
the diagnosis of gallbladder adenomyomatosis is essentially based on T2-weighted images; contrast material administration is not indicated.
MRI findings
- Focal or diffuse gallbladder wall thickening is clearly recognizable both on T1- and on T2-weighted MR images.
MR also offers an high accuracy in excluding the presence of extraparietal infiltration,
which is indicative of gallbladder carcinoma.
- Cystic spaces (Fig 10-11, arrows) within the thickened gallbladder wall,
representing RAS,
appear as well delimited T2-hyperintense spots.
On T1-weighted images RAS usually appear hypointense and they show no contrast enhancement.
The recognition of RAS in pathognomonic for gallbladder adenomyomatosis.
- Pearl necklace sign (Fig 11, arrowheads) is considered a typical finding in gallbladder adenomyomatosis and is the consequence of the presence of multiple contiguous bile-filled RAS within the thickened gallbladder wall.
It is best depicted on T2-weighted images and is pathognomonic for GA.
Tips & tricks
- Thin slice thickness. In some cases RAS may be extremely small and,
therefore,
barely recognizable on thick slab axial T2-weighted images.
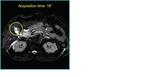
The acquisition of volumetric respiratory-triggered T2-weighted images increases the sensibility of MR in recognizing small RAS and offers the possibility of oblique images reconstruction,
orientated according to gallbladder longer axis.
- Fat saturation. The use of fat-saturated T2-weighted sequences increases the conspicuity of RAS,
compared to unsaturated T2-weighted sequences.
- Diffusion-weighted imaging. The evaluation of apparent diffusion coefficient maps can be useful in differentiating benign from malignant gallbladder wall thickenings. ADC values higher then 2,36 x 10-3 mm2/s are significantly associated with benign lesions.
- "Time is money". A single axial fat-saturated T2-weighted TSE sequence (Fig 12) may be sufficient for diagnosing gallbladder adenomyomatosis.
If RAS are clearly visualized,
no further sequences ae needed.
Pitfalls & limitations
- T1-hyperintensity (Fig 13, arrow) might be found within RAS.
This finding must not interfere with the diagnosis of gallbladder adenomyomatosis because it is simply the consequence of the a concentrated biliary content,
cholesterine crystals or calcifications within RAS.
Indications
MR is the most accurate and reproducible imaging modality for diagnosing GA,
but it is also significantly time- and resource-consuming; therefore MR must be considered the problem solving technique in equivocal cases of GA at US.
COMPUTED TOMOGRAPHY
Background
Computed Tomography (CT) examinations are nowadays extensively performed and the CT finding of a gallbladder wall thickening may represent a diagnostic dilemma; in fact,
CT shows an unsatisfactory accuracy (40-75%) in correctly identifying GA and in differentiating it from early stage gallbladder carcinoma.
A confident diagnosis of GA is possible only if large (at least 3-4 mm) clear bile filled RAS are present.
CT findings
- Thickened gallbladder wall is clearly recognizable at CT,
like at the other above described imaging modalities.
- Well-delimitated hypodense spaces (Fig 14, arrow) representing RAS can be confidently recognized within gallbladder thickening only if they reach at least 3-4 mm in diameter and if they have a clear bile content.
If RAS are clearly identified,
CT diagnosis of gallbladder adenomyomatosis can be made.
- Focal intramural calcifications (Fig 15, arrows) are virtually pathognomonic for gallbladder Adenomyomatosis,
but,
unfortunately,
GA shows intramural calcifications only in a minority of the cases.
Tips & tricks
- Thin slices. Thin slice images (1mm or even less),
although showing more background noise compared to thicker reconstructions warrant an higher accuracy in recognizing RAS.
- Don’t stop at CT! If you are not absolutely confident with your CT diagnosis of gallbladder adenomyomatosis,
don’t hesitate to further investigate the patient by means of a US examination.
Pitfalls & limitations
- Tissue contrast resolution of CT is often insufficient for distinguishing concentrate-bile containing RAS within the thickened gallbladder wall.
I.v.
iodinated contrast material administration increases the signal to noise ratio between gallbladder wall and RAS.
Indications
CT is not indicated in the suspicion of gallbladder adenomyomatosis. At CT,
the incidental finding of a gallbladder wall thickening can be diagnosed as GA only if large RAS are present,
otherwise further US evaluation is indicated.
POSITON EMISSION TOMOGRAPHY
Background
Positron Emission Tomography (PET),
despite to its low spatial resolution,
offers the possibility of obtaining metabolic information from body tissues.
After i.v.
administration of fluorine-18-fluorodeoxiglucose (18F-FDG) high glucose consuming tissues (i.e.
neoplastic and inflammatory ones) can be identified.
PET is not usually performed in the suspicion of GA,
but a lot of patients affected by GA are incidentally evaluated by means of PET for other reasons.
PET findings
- No/low 18F-FDG uptake. GA shows a 18F-FDG uptake lower then the liver.
This finding,
however,
is not exclusive for GA but is common to many benign gallbladder lesions.
Pitfalls & limitations
- Inflammatory reaction. An acute inflammatory reaction sometimes may surround RAS,
generating an increased 18F-FDG uptake that may lead to a neoplasm misdiagnosis.
In such cases a definite diagnosis can be made only on histological specimen after cholecystectomy.
- Spatial resolution. The accuracy of PET in excluding the presence of a gallbladder neoplasm is unsatisfactory in lesions measuring less then 1 cm in their largest diameter.
Indications
PET is not indicatedin the suspicion of gallbladder adenomyomatosis but it may be helpful for excluding gallbladder carcinoma.