1.
Acute Hyperammonaemic Encephalopathy
Hyperammonaemic encephalopathy can occur in acute fulminant hepatic failure or in patient with chronic liver disease.
Patients present with progressive drowsiness,
seizures,
and coma due to toxic effects of ammonia on the brain parenchyma with elevated serum ammonia levels (normal levels 9-30umol/l).
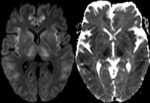
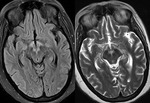
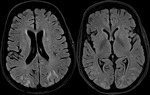
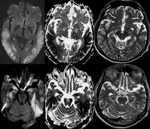
MRI shows diffusion restriction in symmetrical pattern involving insular and cingulate gyri (Fig.
1).
These cortical changes appear to be early imaging findings and potentially reversible if aggressive treatment is instituted.
Involvement of brain regions other than the insular or cingulate gyrus is more variable with bilateral symmetrical diffusion restriction seen in temporo-occipital cortex,
caudate head,
lentiform nucleus,
thalami,
midbrain (sparing cerebral peduncles) and dorsal pons.
In an appropriate clinical setting and correlation with serum ammonia levels it can be differentiated with posterior reversible encephalopathy syndrome,
seizure activity,
hepatic encephalopathy,
and diffuse hypoxic-ischemic injury.
Key Points
- Diffusion restriction in symmetrical pattern involving insular and cingulate gyri should alert the radiologist to the possibility of hyperammonemic encephalopathy.
- Involvement of other regions is more variable with bilateral symmetrical diffusion restriction seen in temporo-occipital cortex,
caudate,
lentiform nucleus,
thalami,
midbrain (sparing cerebral peduncles) and dorsal pons.
- Cortical changes appear to be early imaging findings and potentially reversible if aggressive treatment is instituted.
2.
Osmotic or Central Pontine Myelinolysis (Central pontine and extrapontine myelinolyisis)
Central pontine myelinolysis can be seen in patients with chronic alcoholics,
malnourished patients,
cirrhotic liver disease,
organ transplants,
severe burns,
addison’s disease,
and electrolyte disturbances.
Rapid correction of prolonged hyponatremia is the most important risk factor for the development of CPM.
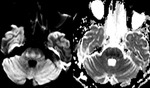
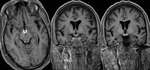
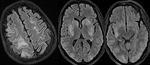
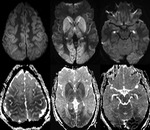
The classic imaging appearance is focal symmetric,
"trident or mexican hat shaped" high signal in the basal pons on T2-weighted/FLAIR sequences and corresponding diffusion restriction with sparing of the tegmentum and corticospinal tracts (Fig.
2).
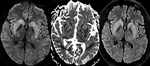
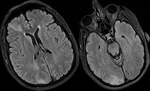
Associated symmetric signal abnormality may also be present in the extrapontine locations including the basal ganglia,
midbrain,
thalami and cerebellum (Fig.
3).
DWI and apparent diffusion coefficient (ADC) values are very useful in distinguishing conditions which may be confused with osmotic demyelination syndrome like encephalomyelitis and multiple sclerosis.
Key Points
- Rapid correction of prolonged hyponatremia is the most important risk factor for the development of CPM.
- The classic imaging appearance in central pontine myelinolyisis is focal symmetric,"trident or mexican hat shaped high signal" in the basal pons on T2/FLAIR sequences with corresponding diffusion restriction and sparing of the tegmentum and corticospinal tracts.
3. Metronidazole Induced Encephalopathy
Metronidazole induced encephalopathy (MIE) is a rare toxic encephalopathy caused by the antibiotic drug metronidazole.
Metronidazole can produce neurologic symptoms at doses exceeding 2 g/d.
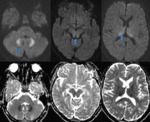
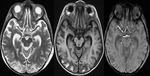
On MRI the dentate nuclei in the cerebellum are most commonly involved,
followed by the tectum,
red nucleus,
periaqueductal gray matter,
dorsal pons (the vestibular nucleus,
abducens nucleus,
and superior olivary nucleus),
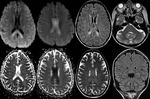
splenium of corpus callosum and dorsal medulla (Fig.
4).
Lesions are often bilateral and symmetric in distribution showing increased signal intensity on T2/FLAIR images,
do not show contrast enhancement and are reversible after discontinuation of the drug.
Diffusion restriction can be seen depending on the severity of edema (cytotoxic or vasogenic).
The most important differential diagnosis includes acute wernicke's encephalopathy where the involvement is predominantly of the diencephalon and midbrain.
Acute nonalcoholic wernicke's encephalopathy can present with bilateral symmetric lesions at the dentate nuclei,
vestibular nuclei and the tegmentum mimicking MIE.
Although MR imaging findings of bilateral involvement of the dentate nuclei are a very characteristic feature of MIE the differential diagnosis of bilaterally symmetrical T2 hyperintense dentate nuclei includes
- Methyl bromide intoxication,
maple syrup urine disease and enteroviral encephalomyelitis.
Key points
- Metronidazole can produce neurologic symptoms at doses exceeding 2 g/d.
- Brain lesions typically located at the cerebellar dentate nucleus,
midbrain,
dorsal pons,
medulla,
and splenium of the corpus callosum.
- Toxicity can be suspected in the presence of the characteristic MRI distribution of lesions with involvement of the cerebellar dentate nuclei in most cases and confirmed when the history of metronidazole intake is available with reversal of symptoms and MRI findings after cessation of drug intake.
4. Wernicke’s Encephalopathy
Wernicke ’s encephalopathy is associated with chronic alcohol abuse,
gastroplasty for obesity,
anorexia nervosa,
voluntary food starvation,
chronic uremia,
and parenteral therapy.
The hallmark of the disease is represented by a clinical triad of altered consciousness,
ocular dysfunction,
and ataxia.
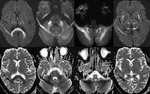
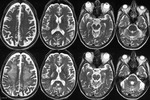
MRI shows symmetric T2 hyperintensity in the mamillary bodies,
medial thalami,
tectal plate and periaqueductal area with contrast enhancement in the same regions most commonly the mamillary bodies (Fig.5,6).
The changes in the mamillary bodies are more often seen in alcoholic patients.
Diffusion restriction can be seen in the involved regions suggestive of cytotoxic edema.
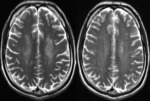
Atypical MRI findings are more common in non-alcoholic patients represented by symmetric signal alterations of the cerebellar vermis,
dentate nuclei,
cranial nerve nuclei,
red nuclei,
caudate nuclei,
splenium,
and cerebral cortex (Fig.
7).
The differential diagnosis in this scenario includes metronidazole-induced encephalopathy.
The conversion of metronidazole to a thiamine analog and its vitamin B1 antagonism acting via metabolic pathways similar to those operating in wernicke's encephalopathy has been described.
Therefore,
the differential diagnosis between WE and metronidazole-induced encephalopathy may be difficult in malnourished patients treated with metronidazole.
Key Points
- Wernicke ’s encephalopathy is commonly associated with chronic alcohol abuse.
- Clinical triad of altered consciousness,
ocular dysfunction,
and ataxia.
- MRI shows symmetric T2 hyperintensity in the mamillary bodies,
medial thalami,
tectal plate and periaqueductal area with contrast enhancement most commonly of the mamillary bodies.
- Atypical MRI findings inculdes symmetric signal alterations of the cerebellar vermis,
dentate nuclei,
cranial nerve nuclei,
red nuclei,
caudate nuclei,
splenium,
and cerebral cortex.
The differential diagnosis in this scenario includes metronidazole-induced encephalopathy.
5. Postpartum Hypernatremic Encephalopathy
Neurological manifestations due to hypernatremia during postpartum period producing encephalopathy and osmotic demyelination is rare.
Diffusion restriction with T2/FLAIR hyperintensity involving the corpus callosum especially the splenium is seen in most of the patients with symmetrical hyperintensities also seen in cerebellar peduncles,
cerebellar white matter,
thalami, internal capsules and corona radiata (Fig.
8).
On coronal T2 weighted images symmetrical hyperintensities of the internal capsule,
crus cerebri,
and pons similar to the ‘wine-glass’ pattern of hyperintensities found in amyotrophic lateral sclerosis (ALS),
primary lateral sclerosis,
and leukodystrophies has been described.
The ‘wine glass’ pattern depicts the involvement of corticospinal tract in these different conditions.
Key Points
- Diffusion restriction with T2/FLAIR hyperintensity involving the corpus callosum especially the splenium.
- Symmetrical hyperintensities also be seen in internal capsule,
corona radiata,
cerebellar peduncles and hippocampii.
- ‘Wine-glass’ pattern of hyperintensities in symmetrical pattern involving the internal capsule,
crus cerebri,
and pons involving the corticospinal tracts has been described.
- The differential diagnosis of T2 hyperintense lesions in the splenium of the corpus callosum besides hypernatremia includes Marchiafava-Bignami disease,
acute toxic encephalopaties,
encephalitis (demyelinating,
viral),
osmotic myelinolysis and anti-epileptic drugs.
6. Posterior reversible encephalopathy syndrome
Posterior reversible encephalopathy syndrome (PRES) is most commonly seen in patients with eclampsia,
organ transplantation related to cyclosporine or tacrolimus,
wegener granulomatosis,
systemic lupus erythematosus,
hypertension and postchemotherapy.
Patients typically experience headache,
altered sensorium,
visual disturbances,
severe hypertension and generalized seizures.
The most characteristic imaging pattern in PRES demonstrates vasogenic edema seen as T2/FLAIR hyperintensity without diffusion restriction involving the white matter of the parieto-occipital regions in a relatively symmetric pattern that spares the calcarine and paramedian parts of the occipital lobes (Fig.
9 and 12).
Imaging Patterns in PRES
Three primary variations of the traditional PRES imaging pattern can be seen
Holohemispheric Watershed Pattern
Vasogenic edema in a linear pattern spanning the frontal,
parietal,
and occipital lobes with lesser involvement of the temporal lobes at the junction between the medial hemispheric (anterior cerebral [ACA] and posterior cerebral arteries [PCA]) and lateral hemispheric branches (middle cerebral artery [MCA]) consistent with the watershed or anastomotic border zone(Fig.
10).
Superior Frontal Sulcus Pattern
Distinct involvement of the frontal lobe associated with varying degrees of parietal and occipital abnormality (Fig.
11).
Dominant Parietal-Occipital Pattern
The typical “posterior” pattern invovling the parietal and occipital cortex and white matter with variable involvement of the temporal lobes.
Partial expression of PRES (defined as the absence of signal intensity abnormality in either the parietal lobes bilaterally or the occipital lobes bilaterally) can be seen.
Asymmetric expression of PRES (defined as unilateral absence of signal intensity abnormality in either the parietal or occipital lobe) can be seen.
“Atypical” Lesions in PRES
Involvement of the basal ganglia,
brain stem,
cerebellum,
splenium and deep white matter can be seen less commonly.
This can be confidently recognized as part of the PRES particularly when associated with the hemispheric features.
Key Points
- Three imaging patterns : Typical pattern "Dominant Parietal-Occipital distribution",
Holohemispheric Watershed,
Superior Frontal Sulcus.
- The most characteristic imaging pattern demonstrates vasogenic edema seen as T2/FLAIR hyperintensity without diffusion restriction involving the white matter of the parieto-occipital regions in a relatively symmetric pattern that spares the calcarine and paramedian parts of the occipital lobes
- Partial expression,
asymmetric expression of PRES and “atypical” lesions involving the basal ganglia,
brain stem,
cerebellum,
splenium and deep white matter can be seen.
- Awareness of this variability in patterns is important in proper recognition of PRES.
7.
Hypoglycaemic encephalopathy
Hypoglycaemia is a sudden decrease in serum glucose level less than 50 mg/dl.
The symptoms included altered sensorium or hypoglycemic coma.
On MRI severe hypoglycaemia manifests as bilateral symmetric diffusion restriction involving the temporal,
occipital,
insular cortex,
the hippocampii and the basal ganglia with sparing of the thalami (Fig.
13).
The deep white matter may be involved in milder cases involving the internal capsule,
corona radiata and splenium of corpus callosum.
These findings can be similar to sporadic Creutzfeldt-Jacob disease,
although the clinical setting should exclude the neurodegenerative disorder.
Correlation with the blood glucose levels may be useful to differentiate this potentially reversible condition from hypoxix ischemic encephalopathy (HIE) and acute infarction.
DWI may be useful to predict outcome.
When diffusion restriction is seen in the corpus callosum,
internal capsule or corona radiata which regress on follow up images,
the patient will likely to recover without a neurologic deficit.
Keys points
- Symmetric diffusion restriction involving the temporo-occipital and insular cortex,
the hippocampii and the basal ganglia with sparing of the thalami.
The internal capsule,
corona radiata and splenium may also be involved.es
- Correlation with the blood glucose levels may be useful to differentiate this potentially reversible condition from HIE and acute infarction.
- DWI may be useful to predict outcome.
Diffusion restriction seen in the corpus callosum,
internal capsule or corona radiata which regress on follow up images suggest good prognosis.
8. Hypoxic ischaemic encephalopathy
Hypoxic-ischaemic cerebral injury occurs at any age,
although the aetiology is significantly different: drowning and asphyxiation remain common causes in children while cardiac arrest or cerebrovascular disease with secondary hypoxemia are common in adults.
Diffusion-weighted MR imaging is the earliest imaging modality to become positive.
During the first 24 hours DWI demonstrates increased signal intensity in the basal ganglia,
cerebral cortex in particular,
the perirolandic and occipital cortices.
The thalami,
brainstem,
hippocampi or cerebellar hemispheres may also be involved (Fig.
14).
Diffusion-weighted imaging abnormalities usually pseudonormalize by the end of the 1st week.
In the early subacute period (24 hours–2 weeks) conventional T2-weighted images typically become positive and show hyperintensity of the injured gray matter structures.
The other variant is parasagittal infarction which involves the deep white matter only at border zones of major arterial territories (water shed).
Key Points
- Diffusion-weighted MR imaging is the earliest imaging modality to become positive.
- Diffusion restriction seen in cerebral cortex in particular,
the perirolandic and occipital cortices,
basal ganglia,
hippocampi and cerebellar hemispheres.
Diffusion-weighted imaging abnormalities usually pseudonormalize by the end of the 1st week.
- Parasagittal infarction involving the deep white matter only at border zones of major arterial territories (water shed) can also be seen.
9. Chemotherapy induced leukoencephalopathy
Several cases of chemotherapy related encephalopathy are noted in the literature with some agents being more problematic than others.
Common agents implicated include cisplastin,
methotrexate,
bleomycin and tacrolimus.
Acute and delayed chemotherapy induced white matter abnormalities occur in a variety of clinical settings including treatment for lymphoma,
leukemia,
glioma,
lung cancer and metastatic disease.
Acute disseminated leukoencephalopathy (ADL) has been proposed as a broad clinical-radiological term describing a range of abnormalities from mild reversible clinical symptoms with MRI changes to profound encephalopathy resulting in death.
DWI/ADC abnormalities are seen in subcortical white matter of the cerebral hemispheres,
corpus callosum,
and brainstem.
Persistent imaging abnormalities characterized by FLAIR/T2 hyperintensities on MRI can be seen (Fig.
15 and 16).
Key Points
-
Acute and delayed chemotherapy induced white matter abnormalities occur in a variety of clinical settings including treatment for lymphoma,
leukemia,
glioma,
lung cancer and metastatic disease.
- Common agents include cisplastin,
methotrexate,bleomycin and tacrolimus.
- DWI/ADC abnormalities are seen in subcortical white matter of the cerebral hemispheres,
corpus callosum and brainstem.
Persistent imaging abnormalities characterized by FLAIR/T2 hyperintensities on MRI can be seen.