This poster is published under an
open license. Please read the
disclaimer for further details.
Type:
Educational Exhibit
Keywords:
Cancer, Ablation procedures, CT, Lung
Authors:
N. Bashar, S. L. Smith; Ipswich/UK
DOI:
10.1594/ecr2014/C-0624
Findings and procedure details
Tip 1: Staffing
- Dedicated team of nurses and radiographers familiar with the procedure.
- Prospective data base of patients.
Tip 2: Careful patient selection
- True oligometastatic disease (<3 lesions per organ fare better than those with more lesions).
- Lesions less than 4 cm in diameter have a better outcome.
- Period of at leat 12 months between primary diagnosis and presentation of metastases.
- PET prior to RFA is very useful to exclude more widespread disease.
Tip 3: Use Conscious sedation whenever possible
- RFA is generally very well tolerated.
- Deep sedation with an opiate and midazolam is preferred.
- Use of Bispectral Index monitoring is useful.
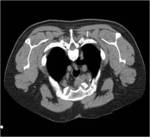
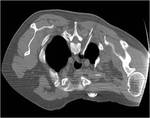
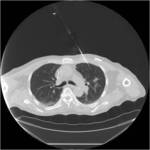
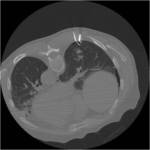
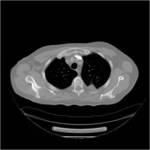
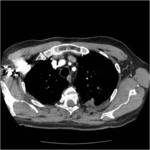
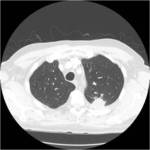
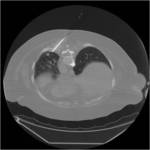
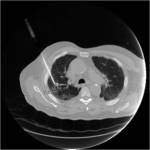
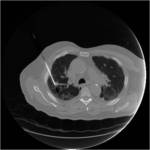
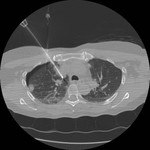
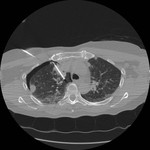
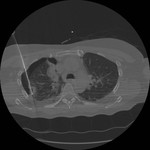
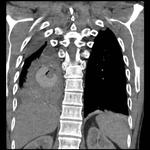
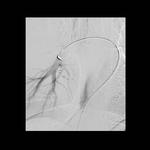
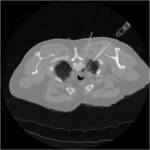
Tip 4: Equipment (figures 1-8)
- We favour the Boston LeVeen RFA needle.
This is an impedance controlled deployable array,
introduced using a coaxial needle.
Its advantages are that it is lightweight,
its coaxial introducer makes insertion under CT control easy and there is no need for any circulating cooling liquid. The expanding tines also act as a useful ‘grappling hook’ which allow for a stable position in the lung even in the context of an enlarging pneumothorax.
- There can be considerable beam hardening artefact from the coaxial needle and we have found removing the central stillet before image acquisition is very useful.
- Needle placement can be a little counter-intuitive.
As the tines project forward by about 8 mm the tip of the introducer needs to be positioned sufficiently proximal to the lesion to ensure good contact/penetration.
- The needle length must be sufficient to reach the lesion,
but not so long that once inserted,
the patient will not clear the CT gantry.
- The operator has a choice of ablation zone size.
We generally use at least 3 cm in the lung to ensure an adequate margin.
Care should be taken with sub pleural lesions or lesions close to bronchi.
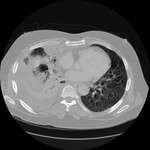
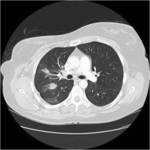
Tip 5: Difficult lesions and practical tips (Figures 9-13)
- Subpleural lesions-use of an iatrogenic pneumothorax or dextrose buffer important to prevent chest wall trauma (figure 12).
- Lesions close to major vascular structures are likely to recur due to the 'heat sink' effect.
Aggressive treatment or manipulations to move them away from vessels are important.
- Care should be taken where lesions are close to major mediastinal strucures.
Deployable times may not be appropriate if there is a risk of damge and a single electrode needle may be more appropriate.
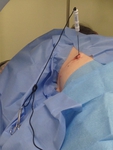
- Patient positioning is very important to allow safe access to the lesions.
Care should be taken to select a short route that preferably avoids the fissues.
Obliuing the patient or moving their arms often improves accessability (figures 2 and 3).
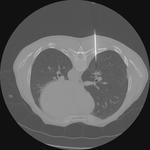
Tip 6: follow up (figures 14-18)
- A scan at one month is useful to asses complications.
- Serial CT at 3 monthly intervals thereafter.
- Local recurrence can be subtle and early detection is the aim to allow aggressive re-ablation (figures 9,10 and 11).
- Any increase in ablation zone size after three months,
or chnage in contour should be considered suspicious.
Tip 7: Complications (figures 19-22)
- Common complications include pneumothorax and pulmonary haemorrhage.
These are usually of no significance.
- Major complications occur in <3%.
these include abscess,
major haemorrhage,
air embolism and vascular injury.