This poster is published under an
open license. Please read the
disclaimer for further details.
Keywords:
Abdomen, Liver, Interventional vascular, CT, Digital radiography, Ultrasound, Ablation procedures, Chemoembolisation, Treatment effects, Aneurysms, Cirrhosis, Radiation oncology in Developing Nations
Authors:
A. F. Mourad; Assiut/EG
DOI:
10.1594/ecr2014/C-0792
Results
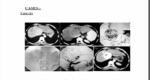
I- Group 1: (TACE):
This group included 20 patients for whom TACE was done.
Twelve patients showed good response (good lipidol uptake with no enhancing residual tumor tissue in triphasic CT).
Eight patients showed poor response (residual enhancing tumor tissue) for whom another procedure was done one month later.
Two out of the 8 patients showed good response.
So,
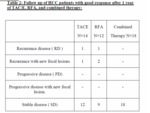
collectively 14/20 patients (70%) showed good response and 6/20 patients (30%) showed poor response (table 1).
AFP in patients who showed good response (14/20) is reduced by 20- 35% in all patients after one month.
Moreover,
at 6 months and one year follow up period,
AFP was near normal range.
However,
it was raised in patients who showed poor response (6/20).
Recurrence at the site of primary lesions was detected in two patients (2/14) who demonstrated good response after the 2nd session of TACE,
and one of them developed new focal lesion.
One of those patients showed re-raising of the AFP but it did not change in the other patient.
While 3/6 patients who demonstrated poor response,
developed new focal lesion and had progression of primary tumor size.
Regarding the other three patients with poor response,
one of them showed stable lesion and the other two showed progression of the tumor only (table 1).
- Survival analysis at one,
six months,
and one year follow up:
All patients were alive up to 6 months,
while 5/20 patients (25 %) died by the end of 1st year.
Those who showed poor response (4 patients),
and another patient who demonstrated good response after the 2nd session but developed local recurrence and new focal lesion.
Therefore,
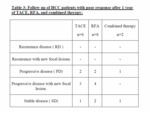
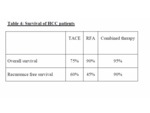
overall survival was 75% (15/20 patients) but the recurrence free survival was 60% (12patients) (table 2).
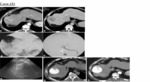
II- Group 2 (RFA):
This group included 20 patients for whom RFA was done.
Nine patients showed good response (complete ablation with no residual enhancing tumor tissue in triphasic CT).
On the other hand,
11 patients demonstrated poor response (residual enhancing tumor tissue),
for them another session was done one month later.
Three out of 11 patients showed good response after the 2nd session.
So,
collectively 12/20 patients (60%) showed good response,
while 8/20 patients remained with poor response (40%).
AFP decreased initially by about 40% in all patients at the 1st follow up (one month),
but near the normal range at 6 months later in those showed good response (12/20 patients).
Three patients among 12 who showed good response after the 2nd session developed local recurrence with re-rising of the AFP at the near end of 1st year and two of them developed new focal lesion in addition.
While 4 patients out of the 8 patients,
who demonstrated poor response,
developed new focal lesion in addition to the progression of the primary tumor.
Regarding the other 4/8 patients,
two of them developed only progression of the tumor while the other two showed stable lesion.
- Survival analysis at one,
six months,
and one year follow up:
All patients were alive up to 6 months,
while 2 patients with poor response died by the end of 1st year.
So the overall survival was 90% (18/20 patients) but the disease free survival was 45% (9/20 patients).
III- Third group (Combined TACE and RFA):
Twenty patients included in this group for whom combined therapy (TACE and RFA) performed.
Seventeen patients showed good response,
while 3 patients showed poor response for whom another session of TACE and RFA have been performed one month later.
One patient among three showed good response.
So,
18/20 patients (90%) demonstrated good response in that group,
while 2/20 patients showed poor response (10%).
AFP decreased by 45 % in all patients at the one month follow up and nearly normal by the end of one year in patients demonstrated good response (18/20 patients).
Neither local recurrence nor new focal lesion had been demonstrated in the 18 patients who developed good response.
On the other hand,
one of the two patients who
demonstrated poor response showed stable disease,
while the other had progressive disease and died.
- Survival analysis at one,
six months,
and one year follow up:
All patients were alive at the end of the 1st year except one patient died (who demonstrated poor response).
So the overall survival was 95% (19/20 patients) while the recurrence free survival is 90% (18/20 patients).
The single patient who survived out of the two who demonstrated poor response showed stable lesion.
Complications were minor in the three groups and included pain,
nausea,
mild hyperthermia and these could be managed conservatively.
However there was one patient in the group of RFA developed minimal peumothorax disappeared spontaneously later on.
Another patient in of combined therapy group and was child pough II,
developed minimal ascites but controlled with diuretics and salt free albumin.