IMAGING TECHNIQUES
Radiography
Once the hemodynamic stability of the patient is assured,
a portable chest radiograph is usually obtained in the emergency room as the initial imaging evaluation.
Upright frontal and lateral chest radiographs are optimal to evaluate chest injuries.
However,
in the polytrauma setting,
supine radiographs are usually performed owing to the need for patient immobilization.
The initial chest radiograph provides information regarding immediately life-threatening conditions,
such as tension pneumothorax or potentially life-threatening conditions,
including hemothorax and pneumothorax.
Other lesions,
such as diaphragm rupture,
flail chest,
pulmonary contusion,
pneumopericardium,
and pneumo- and hemomediastinum,
are often diagnosed or suggested by initial plain radiography.
Furthermore,
chest radiography can quickly provide essential information about tube and line malpositioning.
Computed tomography
After chest radiograph,
a decision must be taken as to whether further imaging techniques are to be performed.
Several reports have shown that the sensitivity of MDCT is much higher than that of radiograph in the detection of thoracic injuries after trauma 2,3: this fact has increased the use of this modality as an additional or substitute screening study for chest trauma victims,
changing the imaging approach to patients sustaining blunt or penetrating thoracic injury.
MDCT offers better spatial and temporal resolution,
a marked increase in scanning speed and it allows high-quality multiplanar reformations that are extremely valuable for diagnosis of severe traumatic injuries of the chest.
In particular,
sagittal and coronal reformations improve the assessment of the aorta,
the tracheobronchial tree and the thoracic skeleton.
The utility of CT studies is most advantageous for direct diagnosis of major vascular,
airway and diaphragm injuries,
pericardial effusion,
the course of penetrating trauma,
and subtle pneumothorax or pleural effusion.
The extent of lung parenchymal and chest wall injuries is also more accurately assessed with CT than radiographs.
Therefore it is rare today for major trauma patients not to undergo CT of one or more body parts.
In addition to this,
CT has been credited with changing management in up to 20% of chest trauma patients with abnormal initial radiographs 2,4.
For instance,
CT is more accurate than radiography for the evaluation of pulmonary contusions,
thereby allowing early prediction of respiratory compromise.
1It is also valuable in the diagnosis of fractures of the thoracic spine,
especially at the cervicothoracic junction,
which is difficult to evaluate with conventional radiography.
Previous statements support MDCT as the gold standard of imaging in patients with severe chest trauma.
Ultrasound
Bedside ultrasonography of the lower chest may be combined with the focused assessment with sonography for trauma (FAST) examination of the abdomen.
Patients with chest trauma may benefit from echocardiography in the emergency department.
Thansthoracic and transesophageal echocardiography can be used to obtain clinical information at the bedside for many emergent conditions,
including the immediate detection of hemopericardium and acute aortic injury 5.
More recent works have demonstrated that US can be used to detect hemothoraces 6 and pneumothoraces 7 with accuracy.
Therefore,
physicians caring for trauma patients should be familiar with these techniques.
SPECTRUM OF IMAGING FINDINGS
Chest wall injuries
Chest trauma may result in significant soft tissues and skeletal injuries.
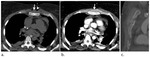
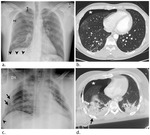
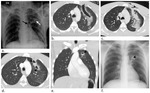
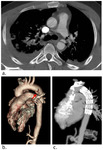
Chest wall hematoma (Fig.
1a-b) may be of arterial or venous origin.
High-pressure arterial hemorrhage leads to hematomas that tend to enlarge rapidly,
causing mass effect with displacement of adjacent organs.
Hematomas due to venous bleeding are usually low-pressure and self-limited.
Extrapleural hematomas (EPH) are commonly associated with rib fractures that injure the intercostal,
internal mammary or subclavian arteries.
Extravasated blood collects between the parietal pleura and the endothoracic fascia. EPH appear as focal lobulated areas of increased density,
which may indent the parietal pleura focally,
creating a convex margin toward the lung.
EPH will not change configuration with changes in the position of the patient,
as will pleural space fluid collections.
In a few cases the localization of a hematoma to either the pleural or the extrapleural space is uncertain: in these cases the medial displacement of the fat layer that is just external to the parietal pleura deep to the endothoracic fascia and inner intercostals muscles aids in localization of hematoma to the extrapleural space 8.
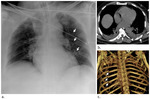
Rib fractures (Fig.
2) are the most common skeletal injuries in blunt chest trauma,
and occur in approximately 50% of patients9.
Fractures of the first three ribs indicate significant energy transfer and may be associated with injury to the brachial plexus and subclavian vessels.
A careful evaluation for upper abdominal organ injuries is indicated in case of fractures of the eighth to eleventh ribs because liver injury is probable on the right side,
while splenic injury may occur on the opposite side.
Although isolated rib fractures may not be of clinical significance,
the presence of multiple fractures may result in respiratory compromise.
Double fractures in three or more neighboring ribs or the combination of adjacent ribs and sternal or costochondral fractures can produce a flail chest,
a condition characterized by a paradoxical movement of a part of the chest wall during respiration.
The paradoxic motion of the fractured segment alters normal pulmonary dynamics and promotes atelectasis,
stasis of secretion and pneumonia; it may require early intubation for ventilatory support.
Flail chest is commonly associated with massive pulmonary contusions.
Furthermore,
fractures of any rib can be associated with pneumothorax,
hemothorax or extrapleural hematomas.
Fractured ribs accompanied by lacerations of intercostals arteries (Fig.
6) can cause major intra- and extrapleural hemorrhage,
often requiring angiographic localization and embolization.
Fractures of the sternum,
sternoclavicular dislocation and fracture of the scapula are indicators of high-impact blunt chest trauma.
Together with rib fractures,
they account for the skeletal injuries that can be part of the “seat belt” syndrome seen in drivers after a motor vehicle collision.
Sternal fracture (Fig.
1c) typically occurs at the body or manubrium.
Frontal chest radiograph misses all sternal fractures unless associated with significant transverse displacement.
Lateral view will detect sternal fractures with high sensitivity,
but it is hardly ever obtained in the acute trauma setting.
Therefore the diagnosis is made more often on CT.
It is important to consider that a fracture that is oriented in the axial plane may be missed on axial CT images: a coronal and sagittal multiplanar reconstruction (MPR) is needed to detect this fracture.
Varying amounts of anterior mediastinal hemorrhage (Fig.
1a-b) are associated almost always with a sternal fracture.
MDCT with isotropic MPR helps to detect and evaluate the extent of concomitant retrosternal hematoma or other associated injuries,
such as cardiac contusion.
Most sternoclavicular dislocations are anterior and have a benign course,
but they are a marker for high-energy trauma: the majority of patients have other chest injuries,
such as pneumothorax,
hemothorax,
rib fractures or pulmonary contusions.
The posterior dislocation is of greater concern due to its frequent association with mediastinal injuries (damage to adjacent vessels,
superior mediastinal nerves,
trachea or esophagus).
MDCT with MPR reconstructions allow a better visualization of the displaced clavicle and critical neurovascular and airway structures,
but an additional evaluation with transcatheter angiography or endoscopy may be required in case of posterior dislocation.
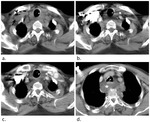
Also scapular fracture (Fig.
3b-c) indicates high-force trauma,
because the scapula is protected by the large muscle masses of the posterior thorax.
Scapular fracture is frequently associated with pulmonary contusions,
rib fractures,
clavicle fractures (Fig.
3) and arterial injuries (axillary,
brachial or subclavian).
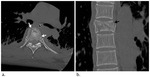
Fractures of the thoracic spine (Fig.
4) may be easily overlooked when interpreting the frontal chest radiograph in acute blunt trauma because the films are often underexposed and are compromised by patient motion,
overlying support lines and tubes,
and poor positioning.
On chest radiography,
an abrupt change in alignment in the thoracic spine indicates spinal injury.
Above the T10 level,
most spinal injuries produce a basic pattern of an anterior fracture-dislocation of two contiguous vertebrae,
often with neurologic impairment 10.
An important imaging finding of subtle thoracic spinal fractures is widening of paraspinal lines,
indicative of a hematoma.
Upper thoracic spine injuries are often poorly demonstrated on frontal chest radiographs.
CT scan is superior in fracture detection and characterization.
Multiplanar reformations in the sagittal and coronal planes (Fig.
4b) are obtained routinely in the presence of a fracture to aid in fracture characterization and stability.
Magnetic resonance imaging is superior to CT scan in the evaluation of spinal cord injury and posttraumatic disk herniation 10.
Pleural space injuries
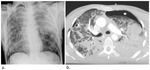
Pneumothorax (Fig.
5) occurs in 30% to 40% of patients after blunt chest trauma.
The most common cause is a rib fracture that lacerates the lung,
but it also may be caused by rupture of a pre-existing bleb at the time of impact.
The diagnosis of pneumothorax is usually easy on upright chest radiographs (Fig.
5a),
with demonstration of the visceral pleural line outlined by radiolucent free pleural air and absent vascular markings in the periphery or apex of the chest.
Unfortunately,
most chest radiographs in polytrauma patients are obtained with the patient in the supine position (Fig.
5c).
In this position pneumothorax tends to accumulate in the antero-inferior aspect of the pleural space producing hyperlucency of the affected hemithorax,
an unduly sharp heart or mediastinal border,
a deep and abnormally lucent costophrenic sulcus (the “deep sulcus sign”) and the “double diaphragm” sign that is seen when air outlines the dome and the anterior insertion of the diaphragm.
Several studies have documented much higher sensitivity of CT for pneumothorax as compared to supine chest radiographs 11.
Patients who are symptomatic or who demonstrate a significant pneumothorax are considered for chest tube placement.
However,
it is important to consider that a small,
asymptomatic pneumothorax can enlarge and become hemodynamically significant if the patient is placed on mechanical ventilation: a prophylactic insertion of a chest tube may be considered in these cases.
Tension pneumothorax (Fig.
5c-d) is a life-threatening condition that is frequently clinically diagnosed before imaging.
The increase in intrathoracic pressure is usually secondary to one-way movement of air from the lung,
airway,
or mediastinum into the pleural space.
This can cause collapse of the ipsilateral lung and compression of the vena cava,
which prevents adequate diastolic filling of the heart.
Radiographic signs of a tension pneumothorax include shift of the mediastinum to the contralateral side,
abnormal lucency of the hemithorax with a collapsed lung in the hilar region,
depression of the ipsilateral hemidiaphragm,
and widening of the intercostal spaces.
Tension pneumothorax requires immediate notification to the clinical service for urgent placement of a chest tube.
If this condition persists despite correct chest tube placement,
there should be concern for a major airway injury.
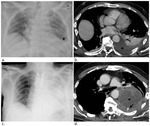
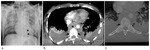
Hemothorax (Fig.
6) is defined as a collection of blood in the pleural space,
usually due to lacerations of the lung parenchyma,
pleura or any of the intrathoracic vessels.
On supine radiography liquid blood will layer posteriorly producing uniform increased density over the hemithorax with preserved visibility of pulmonary vascular markings.
A hemothorax also may compress the lateral lung parenchyma,
which is seen on the supine radiography as a rim of density surrounding the lateral aspect and apex of the lung.
In the erect view the liquid blood will create a meniscus with increased density confined to the lower hemithorax (Fig.
6a).
A large hemothorax can opacify the hemithorax completely (Fig.
6c) and the mediastinum can shift contralaterally (generally this occur in case of arterial bleeding).
Ultrasound is more sensitive than and just as specific as chest radiography for the detection of hemithorax,
although a CT scan is more sensitive for detecting hemothoraces of smaller volumes.
In addition,
the Hounsfield unit (HU) measurement of fluid in the pleural space can be used to identify the origin of the fluid.
Hemothorax measures 35 to 70 HU,
depending on the amount of clot present.
Blood can be seen in the pleural space at different degrees of coagulation,
giving rise to a layered appearance,
called the “hematocrit sign”.
MDCT has also the ability to demonstrate active extravasation into the pleural space from a vascular injury (Fig.
6d),
thereby localizing the bleeding source: in this case a surgical or arteriographic intervention is needed.
A hemothorax of venous origin typically is self-limiting and usually does not increase in size; in case of arterial bleeding there is a progression of size on radiography or CT.
Other possible types of pleural effusion are simple serous effusion (resulting from decreased resorption of fluid by the pleura),
chylous effusion (resulting from disruption of the major thoracic lymphatic channels) and bilo-pleural fistulas (in case of simultaneous injury to the liver and right diaphragm).
Pulmonary trauma
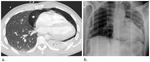
Pulmonary contusions (Fig.
7) are the most common lung injury in blunt chest trauma 12.
Pulmonary contusions result from direct impact to the chest wall,
they often reflect the shape of the impacting object and tend to be located adjacent to bony structures.
Injury to the walls of the alveoli and pulmonary vessels allows blood to leak into the alveolar and interstitial spaces.
The radiologic findings may be absent on the initial chest radiograph,
but they usually become evident over the first 6 hours after the injury.
Chest CT scan is more sensitive then conventional chest radiography in identifying pulmonary contusion and may help predict the need for mechanical ventilation,
which is necessary with greater than 28% of lung involvement but generally not indicated if less than 18% of the lung is involved with contusions 4.
The CT appearance of pulmonary contusions depends on the severity of parenchymal injury.
The “ground glass” pattern is seen when interstitial or partial alveolar compromise occurs,
resulting in a peripheral,
multifocal,
nonsegmental,
nonlobar and ill-defined regions of opacification that readily cross pleural fissures.
When injury to the alveoli is severe the air spaces are completely filled with blood resulting in a widespread areas of consolidation.
Air bronchograms are usually absent as a result of blood filling the airways.
The peripheral opacities typically exhibit a thin zone of surrounding subpleural lucency that is presumed to represent a rim of relatively hypovascular lung tissue that was compressed at the moment of the injury and,
therefore,
relatively spared of alveolar hemorrhage and edema.
Uncomplicated pulmonary contusions begin to resolve on the chest radiograph after 48 to 72 hours,
but complete resolution of severe contusion may take up to 14 days.
Persistence of airspace disease beyond this period suggests the development of pneumonia,
aspiration or adult respiratory distress syndrome (ARDS).
Miller and colleagues found that contusion volume is an independent predictor for the subsequent development of ARDS: patients who had greater than 20% contusion developed ARDS 82% of the time,
compared with only 22% of patients who had less than 20% contusion 13.
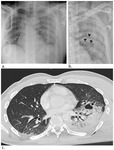
Pulmonary lacerations (Fig.
8 – Fig.
9) are tears in the lung parenchyma leading to alveolar rupture. They can be caused by penetrating injury,
lung perforation from rib fractures and shearing forces caused by inertial deceleration.
If the lacerations are subpleural in location,
they may be associated with a pneumothorax.
When lacerations occur deeper within the lung parenchyma (Figure 8),
they are ovoid or round in shape because of the elastic recoil of the lung tissue,
and have a thin 2- to 3-mm pseudomembrane of adjacent compressed lung parenchyma.
Because contused areas surround pulmonary lacerations,
they are frequently not identified on the initial chest radiograph.
They usually become more apparent over the next 48 to 72 hours as the contusion resolves.
A chest CT is significantly more sensitive to detect and evaluate their extension than a conventional chest radiograph 4.
The laceration may be lucent and filled with air (pneumatocele),
completely opacified as a result of blood accumulation within the cavity (hematoma) or demonstrate an air-fluid level that is due to variable amounts of blood within the lumen.
Often there are numerous small lacerations within areas of contused,
consolidated lung producing a “Swiss cheese” appearance.
Pulmonary lacerations usually resolve slowly over a period of 4 to 5 weeks.
During this time,
a laceration that is filled with clot may be misinterpreted as a lung nodule.
Potential complications of pulmonary lacerations include infection that leads to pulmonary abscess,
enlargement of the laceration,
hemorrhage or formation of a bronchopleural fistula.
A bronchopleural fistula may develop in case of large lacerations involving the pleural surface; this should be suspected if there is failure of pneumothorax resolution following chest tube placement.
Diaphragmatic tears
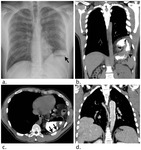
Tears of the diaphragm (Fig.
10) after blunt trauma are uncommon.
Diaphragmatic tears can be caused by both abdominal and thoracic blunt trauma.
Blunt trauma to the abdomen increases the trans-diaphragmatic pressure gradient between the abdominal compartment and the thorax.
The pressure stress results in shearing of the diaphragm.
Traction and compression of the chest wall can lead to avulsion of the diaphragmatic attachments.
Moreover,
fractured ribs secondary to blunt thoracic trauma can tear the adjacent diaphragm.
Left-sided rupture is more frequent then right-sided,
most likely related to the protective effect of the liver.
The detection of this injury with plain chest radiography alone is limited.
Injury to the left hemidiaphragm is more commonly diagnosed radiographically (Fig.
10a) since herniation of abdominal contents is more likely to occur than on the right side where it is blocked by the liver.
Radiographic signs of left diaphragmatic rupture include herniation of abdominal viscera (typically the stomach) above the hemidiaphragm,
air-fluid levels at the left lung base (due to the presence of the herniated viscera) and poorly defined of apparently elevated diaphragm.
An anomalous position of a nasogastric tube tip above the left hemidiaphragm indicates herniation of the stomach,
which may be confirmed with water-soluble contrast administration.
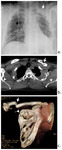
Ruptures of the right hemidiaphragm (Fig.
10d) are strongly suggested after blunt trauma by the elevation of the apparent right hemidiaphragm4 cmor more to the left.
Diaphragmatic rupture is well demonstrated by the use of MDCT with multiplanar reconstructions (Fig.
10b).
MDCT findings suggestive of this kind of lesion include diaphragmatic discontinuity,
herniation of bowel or solid organs into the thorax,
the “dependent visceral sign” and the “ collar or rim” sign.
Under normal conditions,
while the body is supine,
an intact diaphragm supports the abdominal organs.
The “dependent viscera” sign (Fig.
10c) is seen when abdominal organs set against the posterior ribs due to the loss of support from an injured diaphragm.
This sign is present when there is a direct contact between the posterior chest wall and the upper third of the liver (in case of right hemidiaphragmatic rupture) or the stomach or bowel (in case of left hemidiaphragmatic rupture).
The “collar” sign (Fig.
10b) is seen when the herniated stomach or bowel are strangulated at the site of herniation.
On the right side,
the same mechanism can appear as a focal indentation of the liver,
termed the “rim” sign (Fig.
10d),
which may be easily overlooked on axial images.
Detection of this sign requires careful analysis of the sagittal and coronal multiplanar images.
Atelectasis,
particularly of the left lower lobe,
can elevate the apparent hemidiaphragm mimicking diaphragm rupture with herniation.
On the contrary,
false negative radiologic diagnoses are usually due to tears without associated herniation.
Tracheobronchial injuries
Injuries to the trachea and bronchi may occur with blunt or penetrating trauma.
Penetrating injuries most commonly involve the cervical portion of the airway.
In blunt trauma injury occurs as a result of compression of the trachea against the spine,
shearing forces,
or possibly by sudden increased intraluminal pressure against a closed glottis.
The injury typically occurs within2,5 cmof the carina and most commonly in the proximal right mainstem bronchus.
When there is an associated tear in the parietal pleura a pneumothorax (often a tension one) may develop.
The hallmark of the injury is persistent,
progressive,
and severe pneumomediastinum unrelieved by tube thoracostomy,
often associated with increasing subcutaneous emphysema.
MDCT is more sensitive than chest radiography at diagnosing tracheobronchial injury and it can identify the site of airway rupture 14.
Direct CT finding that can suggest a diagnosis of tracheobronchial injury is discontinuity of the tracheal or bronchial wall with air leaking around the airway.
Among the indirect,
more specific signs we can see a collapsed lung resting on the most dependent area away from hilum (“fallen lung” sign),
persistent pneumothorax after tube thoracostomy and herniation or overdistension of an endotracheal cuff in an intubated patient 14.
The endotrachal (ET) tube balloon should not appear wider than2,5 cm in man and2,1 cm in women.
Distension of the ET tube >28 mm implies tracheal rupture.
Among the more prevalent,
but less specific,
indirect findings,
we can see pneumothoraces,
pneumomediatinum,
pneumoretroperitoneum and subcutaneous emphysema.
Most injuries of the trachea are axially oriented and may not be seen on axial CT images; in these cases the use of multiplanar reformations is very useful.
Fiberoptic bronchoscophy remains the gold standard for evaluation of suspected tracheobronchial injuries,
but the procedure is not always possible and may be contraindicated in patients with facial trauma.
The use of MDCT may provide the resolution necessary to adequately diagnose or exclude airway injury.
Esophageal injuries
Esophageal perforation is largely the result of penetrating trauma,
and only rarely the result of blunt trauma (due to its intrinsic flexibility and compliance and its ability to decompress into the mouth and stomach).
Radiologic signs of esophageal perforation include cervical and mediastinal emphysema,
pleural effusion and abnormal mediastinal contour caused by leakage of fluids,
hematoma or mediastinitis.
When the diagnosis of injury to the esophagus is suspected or considered,
both contrast esophagography (with water-soluble contrast) and endoscopy can be used.
Esophageal perforation must be excluded in any case of mediastinal penetrating trauma.
The main contribution of CT is to identify the direction of the missile tract,
although in some cases it may show an esophageal lesion.
Indirect CT signs of esophageal lesion include bubbles of air or fluid accumulation adjacent to the esophagus.
Patients with missile tracts near the esophagus require further studies,
such as endoscopy.
Injuries to the heart and pericardium
Injuries to the heart include cardiac contusion,
laceration and rupture; valve and coronary artery injury; tears of the pericardial sac,
hemopericardium and pneumopericardium.
Among blunt cardiac injuries,
myocardial contusion is by far the most common and it may manifest on echocardiography as areas of impaired wall motion or ventricular hypokinesia.
Fluid in the pericardial sac of an acutely injured patient usually represents blood (hemopericardium).
Unfortunately,
the conventional chest radiograph is of limited use in the diagnosis of hemopericardium since only a small amount of blood can tamponade cardiac motion acutely without changing the cardiac shadow significantly.
Thus,
bedside sonography is very useful to quickly confirm or exclude pericardial fluid after trauma.
At CT fluid into the pericardial sac is easily detected.
A flattened myocardium in combination with hemopericardium indicates the presence of cardiac tamponade.
In pneumopericardium (Fig.
11) the air within the pericardial space outlines the heart and is limited superiorly by the pericardial reflection.
A complication of air within the pericardial sac is tension pneumopericardium that can cause cardiac tamponade.
Developing tension pneumopericardium has been reported to cause the cardiac silhouette to appear progressively smaller on serial conventional radiographs 15.
Rupture of the heart is associated with high mortality: findings on CT include hemopericardium and extravasation of contrast material into the pericardial sac from the injured cardiac chamber 16.
Acute traumatic aortic injuries
Thoracic acute traumatic aortic injury (ATAI) has a high mortality,
with the majority of deaths occurring at the time of injury.
ATAI is usually caused by trauma mechanisms consistent with rapid deceleration forces,
such as motor vehicle accidents or falls from great heights.
Of traumatic aortic injuries,
90% occur at the isthmus,
between the left subclavian artery and the ligamentum arteriosum.
This is the site where the relatively mobile aortic arch becomes fixed as the descending aorta and,
therefore,
this is an area prone to injury from traumatic shearing forces.
Portable ap-chest radiograph plays an essential role in raising the suspicion of ATAI.
Mediastinal blood is expected in all patients with trauma injury to the thoracic aorta.
Radiological markers of mediastinal hemorrhage (Fig.
12 – Fig.
13) on a ap-chest radiograph include obliterated contour of the aortic arch,
tracheal deviation to the right,
displacement of the nasogastric tube to the right,
widening of the paravertebral and paratracheal stripes,
downward depression of the left mainstem bronchus,
and accumulation of blood around the left apex giving the appearance of a radiodense apical “pleural cap” 17.
The presence of signs of mediastinal hemorrhage has only a 20% predictive value for ATAI.
Therefore,
in most of the cases of mediastinal hemorrhage,
the cause is not major vascular injury but it is a bleeding from smaller vessels for which no specific intervention is required.
However,
the absence of all these signs simultaneously has a nearly 100% negative predictive value for ATAI 17.
CT is more sensitive to confirm or exclude mediastinal hemorrhage than is chest radiography.
Direct signs of ATAI on CT include active contrast extravasation (Fig.
13c),
pseudoaneurysm,
abrupt changes in caliber of the aorta,
aortic dissection,
intimal flap or filling defects,
aortic dissection,
and irregularity of the aortic wall.
Indirect signs of ATAI are mediastinal and periaortic hematoma.
The most common CT scan finding is a pseudoaneurysm (Fig.
13 – Fig.
14),
typically located on the anterior aspect of the proximal descending aorta,
immediately distal to the aortic isthmus.
The pseudoaneurysm is an incomplete tear in the wall in which arterial blood is contained by the adventitia of the artery alone and is therefore quite unstable.
Smaller injuries to the thoracic aorta are now detected as a direct result of thinner collimation techniques.
These lesions,
called “minimal aortic injuries”,
include small intramural hematomas,
intimal flaps and intimal thrombus.
The use of MPR and three-dimensional volume-rendering images demonstrating the exact location and type of lesion can be of great use.
If CT is available and shows periaortic blood without direct signs of aortic injury,
aortography is recommended.
Patients with direct signs of aortic injury on CT do not need further evaluation,
and at many centers they are taken to surgery without aortography.
Venous injuries
Venous injuries (Fig.
15 – Fig.
16) caused by blunt trauma are uncommon imaging findings.
Identification of these blunt trauma-related venous injuries on CT images obtained at admission is important because the clinical signs and symptoms of venous injuries are either non-specific or absent and because primary attention may be given to the more common and obvious injuries.
Current protocols for evaluating trauma with MDCT are designed to look for the most common trauma-related injuries,
primarily arterial and solid organ injuries.
Therefore,
it is important to consider that although current imaging protocols are not designed specifically to evaluate the venous system,
venous injuries may nevertheless be identified.
Direct signs of venous vascular injury are thrombosis or occlusion,
complete tear,
rupture,
active extravasation and pseudoaneurysm; indirect signs are perivascular hematoma and vessel wall irregularity.
We present a rare case of azygos arch rupture (Fig.
15).
Three mechanisms describing how the azigous vein is injured in blunt chest trauma have been suggested 18: damage caused by an adjacent spinal fractures,
by a sudden increase in venous pressure (this may occur when the heart is compressed between the sternum and vertebral column and/or when the abdominal cavity is compressed),
or by an axial twisting force on the more mobile azygous arch (in this case rupture occurs when the heart pivots about its axis and the azygous vein cannot accommodate the twisting force because it is anchored posteriorly to the intercostals).
In addition,
a rupture of the subclavian-innominate venous junction is illustrated (Fig.
16).
Blunt injury to the brachiocephalic vein is rare and is seen most commonly in the setting of iatrogenic penetrating trauma,
such as central venous catheter insertion.
Posterior dislocation of the clavicular head can often be associated with vascular injuries in the anterior mediastinum.
Therefore,
any case of posterior dislocation of the clavicle should raise concern about an associated vascular injury.