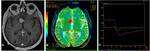
In our study we found the pituitary adenomas to appear in PWI as hyperperfused tumors (Fig.4) with elevated rCBV values and maximum rCBV ranging between 2.42 and 7.55 (mean max.
rCBV= 5.18) (table 1).
In gliomas,
the CBV parameter has been reported to correlate positively with the vascular endothelial growth factor (VEGF) [4],
which is also expressed in the normal pituitary gland and pituitary adenomas.
Moreover,
increased concentrations of VEGF and of VEGF receptor 1 (VEGF-R1) were found in non-functioning pituitary adenomas when compared to normal pituitaries,
suggesting that VEGF and VEGF-R1 expression may be related to pituitary tumor growth and vascularization [5].
These findings coincide with our preliminary results and support our conclusions that pituitary adenomas are highly vascular tumors.
In our study,
apart from high rCBV values,
pituitary adenomas showed characteristic time-intensity curves with little or no return to the baseline (mean value of max.
rPSR=0.36).
Meningiomas of the sellar region (cavernous sinus,
planum sphenoidale,
diaphragm sellae and clinoid process) account for about 15% of nonadenomatous sellar masses and for 20-30% of all intracranial meningiomas [1].
In our study meningiomas (Fig.5) showed perfusion patterns and time-intensity curves identical to meningiomas in other intracranial locations reported in the literature [1].
Moreover,
both adenomas and meningiomas showed very similar perfusion curves with reduced values of rPSR.
This pattern of time-intensity curve is caused by the absence of blood-brain barrier in neovessels of these tumors and thus the high rate of extracapillary leakage of contrast agent [6].
In our study the mean values of maximum rPSR were as follows: adenomas – 0.36; meningiomas – 0.33.
Furthermore,
adenomas as well as meningiomas demonstrated similar mean values of maximum rPH parameter (adenomas – 4.07; meningiomas – 3.57).
There were statistically significant differences between adenomas and meningiomas in the mean and maximum values of rCBV.
Furthermore,
in our opinion,
the usage of fixed cut off values such as 7.14 for max.
rCBV and 5.74 for mean rCBV showing high specificity (91% and 100%,
respectively) and sensitivity (63% and 38%,
respectively) with the analysis of the shape of the time-intensity curve may be very useful in differentiation between intrasellar meningiomas and pituitary adenomas.
Values of max.
rCBV exceeding 7.14 and mean rCBV above 5.74 with a time-intensity curve not returning to the baseline level are very suggestive of the diagnosis of meningioma.
Craniopharyngiomas are the most common suprasellar lesions.
They account for approximately 3% of all intracranial neoplasms and 8% of sellar/parasellar tumors [1].
In plain MR craniopharyngiomas (especially in an intrasellar location and with enhancing the solid part of a tumor),
may be easily misdiagnosed as pituitary adenomas.
Two different clinicopathologically types of craniopharyngiomas can be distinguished: the adamantinous and the squamous-papillary variants [7].
In our study these two types of craniopharyngiomas showed different perfusion patterns.
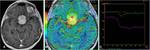
The squamous-papillary type of craniopharyngiomas (Fig.6) presented high rCBV values (maximum rCBV= 5.95),
intermediate PH,
as well as PSR values,
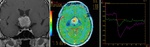
while measurements from enhancing parts of the adamantinomatous type of craniopharyngiomas (Fig.7) revealed low values of rCBV parameter (maximum rCBV = 0.75).
Additionally,
these tumors showed high value of rPSR (rPSR= 1.39) with the characteristic signal-intensity curve,
returning and even exceeding the baseline level (Fig.7c).
This is partially in accordance with Holscher et al.
who reported craniopharyngiomas to be hypoperfused tumors in transcranial duplex sonography,
but the author did not indicate the type of craniopharyngioma [8].
We do believe that the different perfusion patterns can be explained by the different tumor development.
According to the hypothesis concerning tumor development,
the adamantinomatous craniopharyngioma arises from embryonic remnants of the craniopharyngeal duct and the squamous-papillary type from the squamous cell nests of the pars tuberalis of the adenohypophysis [7].
This hypothesis agrees with our preliminary results and may explain the different clinicopathological presentation,
as well as different perfusion patterns of these craniopharyngioma variants.
The squamous-papillary craniopharyngiomas are hyperperfused tumors similarly to adenomas,
because both neoplasms arise from the adenohypophysis [7] and thus may resemble adenomas in perfusion examination.
In our opinion perfusion studies allow us to differentiate not only various types of craniopharyngiomas but also hypoperfused adamantinomatous craniopharyngiomas from hyperperfused adenomas.
This fact is of high importance in everyday clinical practice,
because it enables the correct differential diagnosis,
despite the similar appearance of contrast enhanced intrasellar lesions in the conventional MR sequences.
In our study we also included several other types of sellar/parasellar tumors.
The high perfusion sellar/parasellar tumors were: intrasellar hemangioblastoma,
intrasellar prostate cancer metastasis and suprasellar glioma.
All these lesions showed elevated rCBV values (max.
rCBV>2),
but they demonstrated different signal-intensity curves (with different rPH and rPSR values).
Hemangioblastoma and glioma presented a higher rPH compared to metastasis.
However,
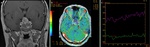
our case of intrasellar hemangioblastoma,
strongly mimicking adenoma in plain MR,
showed a characteristic descending signal-intensity curve with very low rPSR values (rPSR below 0),
which was completely different from perfusions curves of other hyperperfused sellar/parasellar tumors,
including adenomas.
This was our first patient enrolled in the study and initially misdiagnosed as macroadenoma on the basis of conventional MR examination (at that time the perfusion results were not routinely included in the decision making process because of a lack of knowledge and experience).
This patient underwent a huge life-threatening hemorrhage,
and almost died during transsphenoidal surgery,
which should have not been performed in this case.
Finally,
the low perfusion sellar/parasellar tumors also included lymphomas,
which presented low values of rCBV parameter (maximum rCBV = 1.08).
Additionally,
these tumors showed high value of rPSR (mean rPSR= 1.38) with the characteristic signal-intensity curve,
returning and even exceeding the baseline level.
Our findings coincide with other papers reporting that CNS lymphomas are low perfusion tumors [9,10].
We also evaluated the ADC values of sellar/parasellar tumors.
Mahmound et al.
claimed that calculation of the ADC values can help to differentiate between various sellar and parasellar lesions,
especially hemorrhagic pituitary adenomas and non-hemorrhagic lesions with similar structural MR appearance (non-hemorrhagic pituitary adenomas,
Rathke cleft cysts,
and craniopharyngiomas).
ADC was also useful for differentiating between pituitary adenomas vs.
meningiomas and craniopharyngiomas vs.
Rathke cleft cysts [2].
In our study there were no significant differences in ADC values between adenomas and meningiomas,
while other tumors revealed significantly different values of ADC,
compared to pituitary adenomas.
Hemangioblastoma and both types of craniopharyngiomas showed high ADC values.
On the other hand,
metastases and lymphomas presented very low ADC values.
Sellar/parasellar tumors present with different diffusion and perfusion patterns.
The values of ADC,
as well as of rCBV,
rPH and rPSR could be noninvasive in vivo imaging biomarkers of tumor cellularity (ADC) and neoangiogenesis (rCBV,
rPH,
rPSR).
In our opinion PWI and DWI seem to be very useful in the differential diagnosis of sellar/parasellar tumors,
which may be of high importance in clinical practice,
especially in the proper choice of tumor treatment.