Subjects:
We included 17 control subjects and 15 patients with COPD patients.
COPD group was defined as: postbronchodilator (postBd) FEV1/FVC<0.7 and postbronchodilator FEV1<80% predicted (pred.) [3]; cigarette smoking history of >20 pack-years; stable condition for at least 2 months; and optimal medical therapy for at least 8 weeks.
Exclusion criteria were history of asthma,
depression,
neuromuscular or disabling cognitive problems,
engagement in any exercise-training program in the last 3 months,
and other pathologic conditions or severe pain syndromes that could affect physical activity.
Eligible persons were invited to participate if they were lifetime never-smokers and they had no known history of respiratory or cardiovascular disease.
Clinical evaluation was based on an extended combination of the ECSC questionnaire on respiratory symptoms [4] and clinical examination.
The exclusion criteria were: history of chest injuries,
exposure to substances known to cause lung injury,
respiratory disease (self-reported or medical doctor diagnosed asthma,
pulmonary tuberculosis,
pneumonia,
frequent bronchitis,
emphysema or chronic bronchitis),
respiratory symptoms during the last 12 months,
morbid obesity (BMI≥35 Kg/m2),
hypertension or hypotension,
clinically relevant alterations upon the physical examination of the heart,
lungs and chest wall,
expired air CO >10 ppm,
abnormal chest radiography,
major ECG abnormalities,
pitting ankle edema,
diabetes (self-reported or fasted glucose level >140 mg/dl) and use of diuretics,
cardiac glycosides or ß-adrenergic blocking agents.
The study was approved by the institutional ethics committee of our hospital (CEIC Hospital Universitario La Paz; HULP-PI-513) and written informed consent was obtained from each participant.
Imaging Technique: MDCT
All CT examinations were performed with a 16-MDCT scanner (Somatom Sensation 16,
Siemens Medical Solutions,
Erlangen,
Germany).
Scanning voltage was 120 kV and current was 160 mA.
CT of the thorax was performed from the lung apices through the level of the diaphragms at full inspiration and it was repeated at full expiration.
All imaging was performed with a collimation of 16 × 0.75 mm,
table feed of 30 mm/rotation,
and rotation time of 0.6 second/360° tube rotation with a standard reconstruction algorithm.
Analysis was performed using syngo InSpace4D Automated Lung Parenchyma Analysis Software (Siemens Medical Solutions).
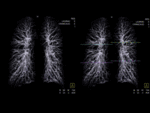
After initial 3D segmentation of the lung,
the program automatically detects the lung contours and the airways (Fig. 1).
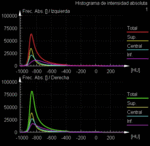
This application display CT values in a histogram,
the program shows volumes,
attenuation distribution,
mean attenuation values,
and standard deviation (SD) of attenuation of the whole lung,
separating right and left lungs,
and superior,
median and inferior thirds,
in tabular form (Fig. 2 , Fig. 3).
The percentage of voxels with attenuation values below a specified level was defined as the lower attenuation volume (LAV) at that threshold; the higher attenuation volume (HAV) is also calculated,
as well as FWHM (Full Width at Half Maximum).
The results were segmented for values for the lower attenuation volume at thresholds (subranges from -1000 to -950 HU to -850 to -801) and in percentiles (from 0 to 90th,
each 15).
Relative area with attenuation values -1000 to -951 is classified as subrange 1 (S1),
from -950 to -901 as subrange 2 (S2),
from -900 to -851 as subrange 3 (S3),
and from -850 to -801 as subrange 4 (S4).
Lung function tests:
They were begun at the same time,
in the morning and at baseline conditions with a MasterLab 4.6 (Jaeger,
Wurzburg,
Germany) system,
which was calibrated with a 3 L syringe each morning and recalibrated at least every 3 to 4 h.
Spirometries were conducted in accordance with American Thoracic Society (ATS)/European Respiratory Society (ERS) recommendations [5].
We required at least three acceptable trials,
defined as a good start of test (extrapolated volume of less than 5% of FVC or 0.15 L,
whichever was larger),
at least 6 s of expiration,
and a plateau in the volume-time curve (change in volume <30 mL for at least 2 s).
Time zero of each maneuver used the back-extrapolation technique.
As recommended by the ATS,
data that did not meet reproducibility criteria were not excluded but subjects were asked to perform up to a maximum of eight maneuvers in an attempt to obtain reproducible results [6].
The highest FEV1 and FVC from tests of acceptable quality were used for analysis.
The other parameters were taken from the trial with the largest sum of FVC and FEV1.
After spirometry,
lung volumes were determined using a variable-pressure plethysmograph,
according to ATS/ERS recommendations [7].
Thoracic gas volume (TGV) at the level of functional residual capacity (FRC) was measured while the subjects made gentle breathing movements against the shutter at a rate of < 1 s-1.
A series of 3-5 technically satisfactory panting maneuvers were recorded,
and after which the shutter was opened,
subjects performed an expiratory reserve volume (ERV) maneuver followed by a vital capacity (VC) maneuver.
Corrections for not occluding the airway at a representative end-expiratory lung volume were made to obtain FRC [8].
FRC was reported as the mean of three or more measurements that differed less than 5% from the mean.
Residual volume (RV) was determined by subtracting the expiratory reserve volume from FRC.
Similarly,
total lung capacity (TLC) was calculated by adding the mean RV to the largest inspiratory vital capacity,
which was within 5% of the mean.
Airway resistance (Raw) and specific airway resistance (sRaw) were computed from pressure and flow measurements breathing warm,
moist air fulfilling BTPS conditions.
sRaw was derived directly from the relationship betweenRaw and TGV.
The frequency of panting was between 0.5 and 1.0 Hz [8].
The mean value of five sequentialspecific resistance loops,
similar in appearance as judged from slopeand shape,
was retained asoutcome.
The diffusing capacity of the lung for carbon monoxide (DLCO) was measured in duplicate by the single-breath method,
according to ATS/ERS guidelines [5].
In a sitting position,
the subjects took a deep breath in,
expired to residual volume,
and inspired a gas mixture containing approximately 0.25% CO,
9% He,
balance synthetic air.
The inspiration had to be free from inhalation artifacts,
last no more than 4 s and has been at least 90% of the subjects’ forced vital capacity.
After inspiration,
subjects held their breath for 10 ± 2 s,
and then expired rapidly (<4 s) into a sample bag.
Breath hold time was calculated as described by Jones-Meade [9],
and washout and sample volumes were set to 0.9 l.
Inspired volume,
alveolar volume (AV),
DLCO and KCO (DLCO/AV),
were calculated from the inspired volume,
room temperature,
barometric pressure and inspired and alveolar sample concentrations of He and CO using estimated values for dead space and for alveolar PCO2.
CO backpressure was ignored in the calculation of DLCO.
The interval between consecutive measurements was at least five minutes.
At least two DLCO measurements were performed which had to agree to within 1 mmol.min-1.kPa-1 or 10%,
whichever was greater,
otherwise further measurements were made until repeatable values were obtained.
At least 5 min elapsed between consecutive measurements,
and to minimize the influence of CO back tension,
the number of measurements was restricted to five a day.
Results were corrected to a standard hemoglobin concentration of 13.4 g.dl-1 for females and 14.6 g.dl-1 for males [5] and they were expressed as mean of two repeatable measurements.
As predicted values for lung function,
ECCS reference equations were used [5].
Statistical Analysis
Data are expressed as mean ± SD for normally distributed variables or as median and interquartile range for non-normally distributed continuous variables,
and as a percentage of the total number of cases studied for categorical variables.
Comparisons between groups were performed using Student’s t,
Mann-Whitney and chi-square tests.
Relationships between CT parameters and lung function tests were determined by Spearman’s correlation coefficient and linear regression analysis. The agreement between lung volumes measured by CT and plethysmography was assessed by the method of differences against the means,
in accordance with Bland and Altman.
These analyses were performed using Statistical Package for the Social Sciences,
version 13.0 software (SPSS Inc.,
Chicago,
IL).
In all cases,
p-values of < 0.05 were considered to be significant.