We illustrate and discuss radiologic findings and features of:
1/Malleolar Fracture:
The malleolar fracture is very common: ranked 3rd after wrist and the proximal end of the femur fractures.These fractures are joint fractures and thus generating osteoarthritis if the bone reduction was not perfect.
The bimalleolar fractures are the most common.
Uni-malleolar fractures are usually associated with a contralateral ligament rupture of the ankle making an equivalent bimalleolar fracture.
Bimalleolar fractures have been classified according to the AO depending on the topographyof the fibular line with respect to lower tibio-fibular liagaments (tibio-fibular syndesmosis),
or samely,
with respect to tibial tuberosity on which is inserted.
1.
Type A
The fibular fracture is below syndesmosis (infra-tubercular),tibio-fibular ligaments are intact and the lesional mechanism is on supination-adduction.
Trauma on the fibula can be reflected either in a rupture of the lateral collateral ligaments,
either by avulsion of the tip of the external malleolus,
or by a transverse fracture of the external malleolus.
There exist three subgroups depending onif the internal malleolus is affected or not:
- A1: medial malleolus intact.
- A2: fracture of the medial malleolus without posterior extension.
- A3: fracture of the medial malleolus with posterior extension.
2.
Type B
The fibular fracture is trans-syndesmosis.The lesional mechanism is on external supination- rotation.
It is the most frequent case.Fibular fracture can be at a definite single line with intact syndesmosis or a rupture of the anterior syndesmosis (avulsion fracture) or multi fragmentary.
There exist three subgroups depending on if the internal malleolus is affected or not:
- B1: medial malleolus intact.
- B2: fracture of the medial malleolus without posterior extension.
- B3: fracture of the medial malleolus with posterior extension.
3.
Type C
The fibular fracture is above the syndesmosis,
the lower tibio-fibular complex is rupturedas well as the interosseous membrane up to the height ofthe line of the fibular fracture.Affection of the medial side is constant(fracture or ligament rupture).
There exist three subgroups depending on the height of the fracture of the fibula:
- C1: Simple fibular diaphyseal fracture.
- C2: Multi fragmentary fibular fracture.
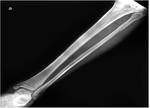
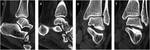
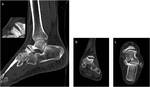
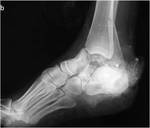
- C3: proximal fibular fracture = “Maisonneuve fracture” (Fig 1): the fracture is located in the neck or head of the fibulaor at the proximal tibio-fibular interline which is then dislocated.
Associated lesions:
- Avulsion of the tibial tubercle on which one of the lower tibio-fibular liagaments is inserted: posterior tibial tubercle in inter-tubercular fractures,
anterior tuberclein associationwith spiroid fractures of the lateral malleolus =“Astley-Cooper‘slesion”.
- Partialfracture of the tibial pilon which was essentially observed in case of inter-tubercular fractures.
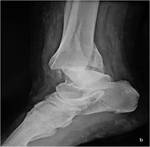
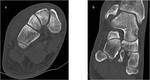
It may concern a marginal fracture of the tibial pilon = “trimalleolarfracture” (Fig 2).
- Tendon lesions
2/Fracture of the distalTibia:
They are less frequent and happen almost after a violent trauma (road traffic accident,
vertical fall,
Skiing accident).
We divide them into simple or comminuted extra-articular metaphyseal fractures,
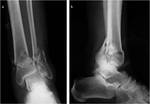
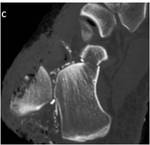
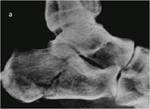
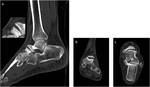
and tibial pilon fractures (Fig 3) which are articular presenting a high risk potential of a secondary osteoarthritis development.
In case of joint damage,
the CT scan with 3D reconstructions specifies the articular congruence defects and the position of bone fragments as well as an eventual extension of the fracture line in the tibial diaphysis or associated fractures of the fibula,
talus and calcaneus.
Fractures of the distal tibia are classified by the AO depending on the fracture if it has a joint damage or not and its partial or total character.articular fractures are called partial when part of the articular surface remainscontinuous with the diaphysis
For children,
fractures of growth cartilage followthe classification of Salter-Harris
3/Talocrural dislocation
The lesional mechanism associates a forced plantar flexion and an axial compression of the tibial resulting in a dislocation,
mostly posterior-medial (75 % of cases),
of the talo-pedal blocout of the mortise which is intact.
An urgent reduction is imposed regarding the high risk of a posterior tibial nervous-vascular compression and skin opening.
4/TalusFracture
This type of fractures happens in a context of a violent trauma.
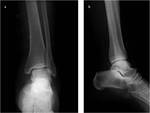
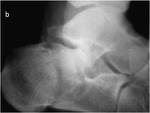
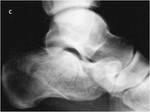
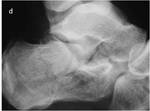
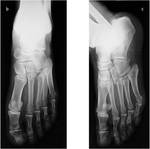
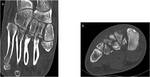
Diagnosis is generally radiographic (Fig 4).
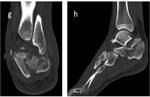
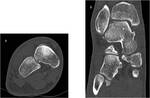
CT may be necessary to identify displacement and integrity of articulary areas in a complex trauma or to confirm the existence of an osteochondral lesion and identify its size and displacement (Fig.5)
Separation Fracture
It is the most frequent type,
caused by a shearing mechanism and it exposes to necrosis risk.
Fractural line,
mostly frontal,
passes through the body or the neck of the talus and we classify these fractures according to Hawkins in four stages expressing necrosis risk:
- Type I: Non displaced.
- Type II: Subtalar dislocation.
- Type III: Subtalar and tibiotalar dislocation.
- Type IV: Subtalar,
tibiotalar,
and talonavicular dislocation (Fig 6,
7).
Other fractures of the talus
- Osteochondral fracture:classically,
an after effect of a serious sprain,
in inversion,and it happens at the anterior-lateral part of the talus trochlea.
- Fracture of lateral process: complicating a lateral twist.
- Fracture of a posterior process:secondary to a forced plantar hyper-flexion
- Comminuted Fracture: secondary to a dorsiflexion.
5/Peritalar dislocation:
Peritalar dislocation is an injury involving both the talo-calcaneal and talo-navicular joints.
It results from a high-energy trauma[7].
Peritalar dislocations are rare and represent approximately 1 to 2% of all dislocations
We distinguish four types of peritalar dislocation:: Medial dislocation (70%),
lateral dislocation (20%),
posterior dislocation (8%),
and anterior dislocation (2%).
In reality as anterior and posterior dislocations always have some degree of medial and lateral displacement,
it is suggested that only two groups of injuries exist: the medial and the lateral types.
The mechanism of injury has been reported as severe inversion (medial dislocation) or eversion (lateral dislocation) of the foot.
6/ Calcaneus fracture:
It represents 60 % from tarsal fractures.
We distinguish:thalamus fractures (3/4 of cases) and extra thalamus fractures (1/4 of cases).
Thalamus fractures are bilateral in 20 % of cases.
We distinguish:
- Separation fracture (through shear).The fracture line separates two calcaneal fragments:an antero-medial fragmentcomprising the sustentaculum tali and part of the posterior talar articular surface,and postero-lateral fragmentincluding the tuberosity of the calcaneus and the remaining posterior articular surface.In one third of cases,
a second line of sagittal fracturesubdivides the antero-medial fragment into two fragments.
- Compaction fracture(through compression) with displacement of the postero-lateral fragment upward and outward.In some cases,
the posterior line extends up to the posterior cortex of the calcaneus,
it is the "tongue-type fracture".If the postero-lateral fragment moves at compression,
which is rare,
it dislocates upward and outward: it is fracture-dislocation of the calcaneus.
On the lateral radiograph,
the angle formed by the anterior and posterior talar surfaces (Bohler angle),
normally between 25 ° and 40 °,
is reduced in case of depression of the posterior talar articular surface.
Sometimes the fracture is hardly visible on the radiograph requiring the submission of further impacts (retro-calcaneal incidence).
Duparc has classified the different calcaneus fractures depending on the number of fragments and their displacement.
- type I (7 %): two fragments,
slightly or not displaced (Fig 8).
- type II (0,5 %): two fragments with dislocation of the postero-lateral fragment (Fig 9).
- type III (43 %): three fragments (antero-medial,
postero-lateral and cortico-thalamic)(Fig 10).
- type IV (44 %): four fragments (plantar crosswallsof the postero lateral fragment) (Fig 11).
- type V (4,5 %): calcaneal crash(Fig 12).
The CT is essential to identify bone lesions,
associated joint calcaneocuboid injuries and damage to the peroneal tendons (tenosynovitis,
dislocation,
subluxation,
tendon incarceration).
Extra-thalamic fractures usually do not require the use of a complementary TDM,
which are those:
- Of The tuberosity of the calcaneus by avulsion of insertion of the Achilles tendon.
- Of the rostrum of the calcaneus (15% of fractures Of the calcaneus)by inversion bending of the foot plantar causing calcaneal avulsion in the bifurcated liagaments
- Of the sustentaculum tali.
- Of the fibular trochlea (rare).
7/Fractures of the navicular bone:
They are an after effect of a tear:
- of the distal insertion ofthe dorsal talo-navicular ligament(Chopartsprain),
- or also the insertion of tendon of the posterior tibial muscleduring a forced eversion of foot causing an extra articular fracture of the medial tuberosity (Fig 13).
We must distinguish them from the accessory navicular bone (with more regular contours,
triangular),
and the intra-tendon sesamoid bone (round or oval,
with no connection to the navicular bone).
Body fractures compromises that of the static medial arch of the footand that of the first ray Delayed healing is common,
as well as osteonecrosis and secondary osteoarthritis.
8/Cuboid fracture
They usually result from a direct hiton the lateral border of the foot.
They are most often associated with a fracture of the calcaneus or tarso-metatarsal dislocation.
9 /Cuneiform fracture
They result from a mechanism in compression or crushing.
They are most often associated with a fracture of the metatarsal bones,
navicular bone or tarso-metatarsal dislocations.
The medial cuneiform is the most frequently affected (Fig.14)
10/ Chopart dislocations
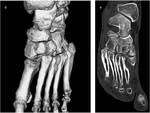
They are dislocations of the mid-tarsal (talonavicular and calcaneocuboid) joints of foot (Fig 15).Four ligaments are interested in the damage: the dorsal talonavicular ligament often affected first,bifurcated ligament,
more rarely,
the calcaneonavicular ligament and the plantar calcaneocuboid ligament.
The lesional mechanism is a plantar flexion possibly associated with a hindfootvarus.
These lesions frequently involve a sprain of talocrural or subtalar joint.
On CT,
we seek a thickening of the dorsal talonavicular ligament as well as of the foot,the bifurcated ligament and bone lesions.Ultrasound also is a simple way to confirm the lesion..Oblique radiographic views can objectify an avulsion of the medial and lateral calcaneocuboidien ligaments.
MRI is only indicated within the framework of a differential diagnosis.
11/ Sprain of the Lisfranc tarso-metatarsal joint
This joint connects of the mid-foot to the joints of forefoot.
It is maintained by two ligaments::
- The Lisfranc ligament uniting the medial cuneiform to the base of the 2nd metatarsal.
It only ensures the cohesion of the first inter-metatarsal space because there are no interosseous ligaments between the medial and middle cuneiforms and between the bases of the first and second metatarsals.
- The deep transverse metatarsal ligament which secures the lastfour tarso-metatarsal joints.
Affection of this joint is rare,
estimated at 1 per 55 000 patients per year.Sprains occur during supination,
pureplantar flexion and forced adduction of midfoot (jump or shoot).
They are most often the result of high-energy trauma.
The last four metatarsals are joined by the transverse ligament and dislocate together.
There are two basic types of Lisfranc injuries
- Divergent: medial or dorsal displacement of the 1st metatarsal and lateral displacement of 2nd to 5th metatarsals (Fig 16).
- Homolateral: All of the metatarsals are dislocated laterally (Fig 17).
In reality,
the Lisfranc sprain often corresponds to a fracture-dislocation(base of the 2nd metatarsal,
first cuneiform or cuboid)which requires a perfect anatomical reduction because it is very arthrogenic.
Diagnosis is difficult on standard radiography and about 20% of these lesions are ignored on initial radiographs.
The radiographic assessment must contain at least an anteroposterior and lateral views of the foot in a standing position,
if possible.
Medial 30° oblique view of the foot can unmask small fractures.
At the anteroposterior view,
we look for:
- the medial margins of the second metatarsal and the middle cuneiform should be well aligned.
- the lateral margin of the first metatarsal should also be aligned with the lateral margin of the medial cuneiform.
- the medial margins of the fourth metatarsal and cuboid should be well-aligned.
At the lateral view,
we look for:
- Loss of the normal alignment at the plantar edge of the medial cuneiform and the first metatarsal base by sagging the medial arch of the foot.
- Loss of normal alignment of the dorsal side of the 2nd metatarsal base and the intermediate cuneiform.
CT is useful in the diagnosis of subtle midfoot misalignments and fractures as it allows for imaging in various planes and allows for visualization of unobscured anatomy.
Tarsometatarsal misalignment,
subtle fractures,
and joint space fracture fragments are better appreciated than with conventional radiography.
CT also allows detection of interposed bone fragments and tendons,
which may impede adequate reduction
12/Fractures of the metatarsal bones
Fracture of the metatarsal base: Fig.18
Fracture of the 1st metatarsal base often occurs by direct hit.
It is frequently open and poly fragmented and requires surgical reduction.
Medium metatarsals’ fractures are often multiple; associated lesions at the tarso-metatarsal joint should be sought.
Fracture of the second metatarsal base is the most common and willingly observed among tiptoe dancers.
The fracture of the 5th metatarsal base is or not,
articular.
It must be systematically investigated in a context of lateral ankle sprain.
Diaphyseal fracture: Fig.19
It results from a fall on tiptoe (transverse or spiroid fracture) or is secondary to the fall of a heavy object (poly fragmentary fracture exposing to bone splinters and the risk of necrosis).
Col fracture:
It is common because of the fragility of this anatomical region.
It is complicated by a horizontal or vertical displacement.
Impaction fracture of the head
It is rare and occurs particularly in the context of bone disease (algodystrophy,
osteomalacia).
13/Sesamoid fractures
The sesamoid bones (lateral and medial) are located on the bottom of the first metatarsal head in the forefoot.
Their fracture is secondary to a crush: fall or landing from a jump with direct trauma to the metatarsal head,
especially with the ballet dancer,
more rarely,
crushing the forefoot or complication of the 1st metatarsophalangeal dislocation.
The frontal fracture most often affects the medial sesamoid,
unlike the rather sagittal cleavage of bipartite sesamoid (34% of the population,
bilateral in 25% of cases).
Moreover,
in the latter case,
the sesamoid is generally wider than a normal sesamoid.
Axial incidences of GUNTZ or Walter Muller with a tangent ray to the sesamoid used to assess metatarsophalangeal sesamoid spacing and multi-character of fragmentation.
14/Phalangeal trauma
- Sprain metatarsophalangeal is rare and mainly concerns the hallux ,
less commonly the fifth metatarsophalangeal.
It occurs during the sports practice,
most often a result of a hyperextension.
It is secondary to the tearing of the plantar plate,
mainly at its proximal insertion on the metatarsal head.
MRI and ultrasound can reveal the capsular ligament rupture.
- Fracture of the phalanges is secondary to a direct mechanism (crush by dropping a heavy object) or indirect (flexion or torsion in some sports like judo or jump).Radiographs are sufficient for the diagnosis and used to distinguish extra-articular fractures from intra-articular fractures.
- Interphalangeal sprain is readily associated with a dislocation or fracture wrenching; it is secondary to a hyperextension associated with a varus or valgus.
The treatment consists of a syndactyly.