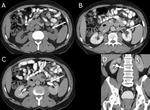
The renal sinus is a spacious central cavity formed by the extension of the perinephric space into the deep recess located at the medial border of the kidney,
and is surrounded by the renal parenchyma.
It is occupied by the major branches of the renal artery and vein,
the major and minor calyces and the renal pelvis,
the kidney’s collecting system.
The remainder of the sinus contains adipose tissue,
lymphatic channels,
nerve fibers of the autonomic nervous system,
and varying quantities of fibrous tissue Fig. 1 .
The renal pelvis is thin-walled.
The tissue composition of the renal pelvis,
ureters,
bladder and urethra is comparatively simple.
Each of these elements has a wall lined by transitional epithelium (urothelium) containing smooth muscle.
Usually the renal pelvis is non-dilated and may be ectatic and extrarenal.
Various imaging techniques can be used to evaluate pathological conditions affecting the renal pelvis,
including US,
CT and MR imaging.
US is the initial screening technique for noninvasive imaging of the kidney.
The normal renal sinus appears as an area of increased echoes with variable contours due to the fat-parenchyma interface.
A collapsed renal pelvis may be indistinguishable from echogenic renal sinus fat.
Though in general US obtains good results,
it has limitations,
especially in the case of small lesions,
when the renal sinus lesion is poorly defined,
or if the echo pattern is similar (or identical) to that of the adjacent renal sinus fat or adjacent renal parenchyma.
CT is the most sensitive,
efficient,
and comprehensive imaging technique for evaluating the kidney and is the technique of choice for a wide variety of renal sinus lesions.
A typical CT urography protocol has three phases which allow complete evaluation of the most common urologic causes of hematuria: that is,
calculi,
renal masses,
and urothelial tumors.
After an initial unenhanced acquisition,
nephrographic phase images are acquired 90–100 seconds after administration of a nonionic contrast agent (100–150 mL of 300 mg I/mL at 2–4 mL/s).
Pyelographic phase images are acquired 5–15 minutes after contrast administration to evaluate the urothelium from the kidneys to the bladder Fig. 2.
Sometimes,
an arterial phase acquired 20-25 seconds after administration of a nonionic contrast agent is obtained.
MR imaging is an alternative to CT for evaluation of renal sinus lesions.
It can also be used in patients with renal failure or contrast material allergies.
The clinical presentation of the thickening of the renal pelvis varies widely: it may be asymptomatic,
cause colicky pain and hematuria,
or present clinical and analytical signs of sepsis.
Treatment options vary depending on the etiology,
which may be inflammatory (pyelitis or pyeloureteritis related to lithiasis),
catheter-related or idiopathic,
infectious (related to tuberculosis or bacterial infection),
or neoplastic (related to urothelial carcinoma or lymphoma).
Knowledge of the various radiological manifestations of the etiologies of thickening of the renal pelvis is the key to correct diagnosis and the selection of optimal treatment.