Legend:1) BM: Bone marrow; 2) CN: Cranial nerve; 3) EBV: Epstein-Barr virus; 4) IJV: Internal jugular vein; 5) NHL: Non-Hodgkin lymphoma; 6) PPS: Parapharyngeal space; 7) SCM: Sternocleidomastoid muscle; 8) SCC: Squamous cell carcinoma
I-DEEP SPACES OF THE NECK

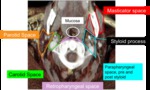
Fig. 1: Deep spaces of the neck
HOW TO LOCALIZE A LESION TO THE CORRECT DEEP SPACE:
Find the center of the mass and evaluate how it displaces the parapharyngeal space (PPS).
For example,
a lesion in the carotid space will displace the PPS medially and anteriorly (See Fig. 1).
This schema works for the four spaces which surround the PPS: parotid,
carotid,
masticator and mucosal.
For the prevertebral and retropharyngeal space,
evaluate the displacement of the prevertebral muscles: the prevertebral muscles are displaced ANTERIORLY by a prevertebral lesion and POSTERIORLY by a retropharyngeal lesion.
II- RELEVANT CLINICAL INFORMATION
Lesions that respect the facial planes tend to be benign or non-aggressive malignant lesions,
while lesions that cross facial planes tend to be aggressive both for neoplastic (benign and malignant) and non-neoplastic etiologies.
-Parotid space (orange in Fig. 1): Bordered anteriorly by the masticator space and medially by the carotid and parapharyngeal space,
it contains the parotid gland (which is divided into superficial and deep lobes),
blood vessels,
the facial nerve (in the deep parotid lobe) and lymphatic tissue (parotid lymph nodes).
Malignant lesions that affect this space include the salivary gland neoplasms (mucoepidermoid carcinoma,
adenoidcystic carcinoma,
malignant mixed tumor,
etc.),
SCC,
adenocarcinoma,
NHL.
-Parapharyngeal space (blue in Fig. 1): Extends from skullbase to hyoid bone and contains only fat,
it is divided into anterior and posterior portions by the styloid process.
Malignant lesions include malignant tumors from salivary gland rest and more commonly direct invasion.
-Masticator space (red in Fig. 1): Contains the muscles of mastication,
ramus and posterior body of the mandible,
the inferior alveolar vein and artery and the masticator and inferior alveolar nerve.
Malignant lesions include soft tissue and osseous sarcomas,
non-Hodgkin’s lymphoma (NHL) and minor salivary gland malignancies.
It is important to note that perineural spread through the mandibular branch of the trigeminal nerve (CN V3) can reach the brain as it enters through the foramen ovale.
-Carotid space (green in Fig. 1): Extends from the aortic arch to the skull base,
contains CN IX-XII,
the mayor blood vessels of the neck (the carotid arteries and jugular veins),
and lymph nodes.
Malignant lesions include SCC direct invasion or metastasis,
NHL.
-Mucosal space,
including the nasopharynx,
oropharynx,
hypopharynx and larynx (white in Fig. 1): Over 90% of tumors are squamous cell carcinoma (SCC) in origin,
although there is an extensive list of possible malignant neoplasms.
There is a strong relationship between Ebstein-Barr virus (EBV) infection and SCC,
especially in the nasopharynx.
III-DWI AND ADC VALUES IN NECK ONCOLOGICAL IMAGING
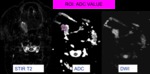
DWI images (Fig. 2) utilized to determine restriction of lesion of interest.
Although still being developed as a tool to evaluate malignant potential and tumor response of a neoplasm,
it is extremely useful during the radiological evaluation,
as it more clearly identifies masses or lymph nodes that might have malignant potential than purely anatomical images.

Fig. 2: DWI and ADC values
IV- DEEP CERVICAL LYMPH NODE CHAIN LEVELS
A significant percentage of tumors,
especially SCC in the oral and oropharynx region,
present with cervical lymphadenopathy.
Lymph node involvement is crucial in staging,
thus an accurate assessment of all nodal chains is required,
Fig. 3

Fig. 3: Deep cervical lymph node chain
- Level I: Submental (IA) and submandibular (IB).
Along the body of the mandible to the angle,
then inferomedially to the hyoid bone and then superomedially back to the mandible.
Drain the submandibular and sublingual glands,
cheek,
nose,
lips (typically bilateral),
gums,
soft palate,
floor of the mouth,
anterior tongue.
- Level II: Upper and anterior to the sternocleidomastoid muscle (SCM).
The anterior upper third of the SCM,
above the level of the hyoid bone.
Anterior,
lateral or medial to IJV (IIA) or posterior to IJV (IIB).
Drain the oral cavity,
oropharynx,
nasopharynx (retropharyngeal nodes first),
hypopharynx,
parotid gland,
lips,
soft palate (IIA)
- Level III: Middle and anterior to SCM.
The anterior middle third of the SCM,
between the level of the hyoid bone and the level of the cricoid cartilage.
Drain the oral cavity (level I and II affected first),
oropharynx,
hypopharynx
-Level IV: Lower and anterior SCM.
The lower third of the SCM,
beneath the level of the cricoid cartilage.
Drain the oropharynx (level II and III affected first),
hypopharynx,
larynx and thyroid gland
-Level V: Posterior triangle.
The triangle formed by the posterior border of SCM,
anterior border of trapezius and superior border of the clavicle.
Drain the larynx,
thyroid gland,
hypopharynx (levels II-IV affected first),
base of tongue,
tonsils
-Level VI: Anterior compartment.
The anterior part of the neck along the hyoid bone to its lateral tip then inferiorly along the anterior border of SCM.
Drain the larynx,
thyroid gland,
infraglottic tumors.
Submental level 1A (red arrow,
Fig. 4)

Fig. 4: Submental level 1A
Submandibular upper jugulodigastric IIA (orange arrow),
upper posterior to jugular vein IIB (double orange arrow) and superior posterior triangle VA (green arrow),
Fig. 5.

Fig. 5: Submandibular upper jugulodigastric IIA (orange arrow), upper posterior to jugular vein IIB (double orange arrow) and superior posterior triangle VA (green arrow)
Middle level III (blue arrow,
Fig. 6)

Fig. 6: Middle level III
Lower level IV (yellow arrow,
Fig. 7)

Fig. 7: Lower level IV
Lower posterior triangle VB (green arrow) and anterior /prelaryngeal / vesperal space VI (purple arrow),
Fig. 8.

Fig. 8: Lower posterior triangle VB (green arrow) and anterior /prelaryngeal / vesperal space VI (purple arrow)
Retropharyngeal- Retropharyngeal nodes (not technically part of cervical deep nodes),
Fig. 9.

Fig. 9: Retropharyngeal nodes (not technically part of cervical deep nodes)
Definition of lymphadenopathy in head and neck: More than 15 mm for jugulodigastric lymph nodes,
more than 10 mm for other nodes (except retropharyngeal lymph nodes,
pathologic at a diameter of more than 8 mm)
V-KEY ANATOMICAL STRUCTURES OF THE NECK
A- Nasopharynx
Fossa of Rosenmüller must always be evaluated in otomastoiditis to rule out an obstructing mass (eustachian tube connects middle ear with nasopharynx),
Fig. 10.

Fig. 10: Fossa of Rosenmüller
Waldeyer ring (white circle,
Fig. 11),
is a ring of lymphoid tissue that can be affected in nasopharyngeal tumors and neoplasms affecting the cavum.
Part of the oral cavity,
the midline raphe of the tongue contains the neurovascular bundle,
it is important to evaluate if it is affected,
as well as to rule out contralateral involvement (precludes partial glossectomy).

Fig. 11: Waldeyer ring
B- Oral Cavity
Squamous epithelium in oropharynx from endoderm= poorly differentiated,
aggressive carcinomas.
Squamous epithelium in oral cavity from ectoderm= differentiated,
less aggressive lesions.
Mylohyoid muscle: Main supporting structure of the floor of the mouth,
serves as a key anatomic landmark separating the sublingual space from the submandibular space,
Fig. 12.

Fig. 12: Mylohyoid muscle
Retromolar trigone (Fig. 13) is a fatty recess that cannot be assessed clinically,
it is imperative to rule out invasion radiologically.
SCC in this region has a predilection for lymph node involvement.

Fig. 13: Retromolar trigone
Extrinsic muscles of the tongue (Fig. 14),
important to evaluate,
as atrophy or edema may correspond to perineural spread of disease and invasion of the hypoglossal nerve (CN XII).
It also represents T4a tumor staging.

Fig. 14: Extrinsic muscles of the tongue
Mandible and osseous invasion imply T4 disease,
look for abnormal low or intermediate signal on T1W or abnormal enhancement.
Always evaluate alveolar nerve recess,
fat infiltration implies perineural disease,
Fig. 15.

Fig. 15: Alveolar nerve recess
C- Pharynx/ Laryngopharynx / Hypopharynx
The hypopharynx is limited anteriorly by the larynx (thus why some authors call it the laryngopharynx),
inferiorly by the esophagic sphincter and inferior border of the cricoid cartilage,
superiorly by the oropharynx and the hyoid cartilage,
posteriorly by the constrictor and longitudinal muscles.
It is divided into three distinct regions: piriform fossa or recess,
postcricoid region and posterior wall.
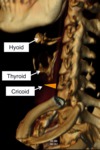
Hyoid,
thyroid and cricoid cartilages,
Fig. 16.
They are key structures as they not only define anatomical landmarks used to separate node levels and neck levels,
they are key structures in tumor staging.
Involvement of these structures indicates T4a stage (T3 if internal margin of thyroid cartilage affected in supraglottic tumors).
They tend to calcify in old age,
disruption of calcification indicates tumoral disease.

Fig. 16: Hyoid, thyroid and cricoid cartilages
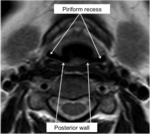
The most common location for tumors in this region is the piriform recess/piriform sinus (60-85%),
Fig. 17,
thus it is imperative to rule out any disease in the radiological evaluation.
Neoplasms in this region tend to show ‘skip growth” and to disseminate underneath the epithelium,
thus they present in advanced stages and tend to have the poorest prognosis.
Invasion of the piriform sinus represents T2 stage in supraglottic tumors.

Fig. 17: Piriform recess/piriform sinus
D- Larynx
The larynx is composed of three regions:
1) SUPRAGLOTTIS,
which contains the false vocal cords,
the ventricles,
vallecula,
the arytenoid cartilages and the aryepiglotic folds
2) GLOTTIS,
which contains the true vocal cords and the anterior and posterior commissure
3) INFRAGLOTTIS,
located inferior to the true vocal cords.
The anatomy of the larynx is extremely complicated,
and thus it is imperative for the head and neck radiologist to be familiar with its structures.
As well,
laryngeal tumors are five times more common than pharyngeal neoplasms.
Supraglottis (Fig. 18,
Fig. 19): The vestibule is the main pathway of extension from glottic tumors into the supraglottis.
The supraglottis has an extensive lymph node network,
this 25-50% of tumors present with cervical lymphadenopathy,
often bilateral.
They tend to originate in the epiglottis,
and present at a later stage than glottic tumors,
as they do not affect phonation.
Tumors in the supraglottis are three times LESS common than the glottic tumors.
Pre-epligottic fat invasion represents T3 disease.

Fig. 18: Supraglottis

Fig. 19: Supraglottis
Glottis (Fig. 20): Glottic tumors are the most common in the larynx.
They tend to present earlier than in the rest of the regions since they affect the vocal cords and thus phonation.
The glottis,
specifically the space of Renke where the true vocal cords lie has NO LYMPHATIC TISSUE.
Thus,
neoplasms localized to the true vocal cords can be cured with surgical excision or radiotherapy.
If glottic tumors present with adenopathy is because they have spread beyond the glottis or into the anterior and posterior commissures,
which are rich in lymphatic networks.
Invasion of the anterior or posterior commissure implies contralateral extension of tumor.
Arytenoid cartilage invasion represents at least T2 disease.

Fig. 20: Glottis
Infraglottis (Fig. 21): Primary tumors are extremely rare and tend to be from locoregional invasion.
They have a predilection for anterior extension through the cricothyroid membrane laterally or cricothyroid ligament centrally.

Fig. 21: Infraglottis