Prior to percutaneous nephrostomy insertion,
acceptable INR,
platelets and coagulation must be achieved and risk stratification undertaken [6].
Urine-analysis to screen for active infection and use of prophylactic antibiotics is necessary.
Imaging should be reviewed for anatomical consideration,
thereby reducing the risk of injury to organs and vessels [7].
With the transplant kidney,
the pelvic bowel loops are especially vulnerable.
The transplant kidney is assessed using combined US and fluoroscopy,
but sole US or CT guidance can be used.
Patients are positioned supine [6].
Conscious sedation is achieved using titrated sedo-analgesia with monitoring of BP,
pulse and oxygen saturation.
The skin,
soft tissue and renal capsule in the expected trajectory are anaesthetised with 1% lidocaine [6].
The ideal calyx for renal access in the transplant kidney is the most superior and lateral as this will be well away from the peritoneal reflections and bowel,
as well as the renal vessels; but sometimes the interpolar or lower pole calyx may be more appropriate.
In any case,
a lateral entry should be ensured.
Under US guidance an appropriate needle is directed into the centre of the chosen calyx (either a 21G access set or a 18G/4F sheathed needle can be used) [6]. Once entry into the calyx is established,
the needle stylet is removed and urine aspirated and reserved for bacteriological culture.
An equal or lesser measure of contrast can then be injected to opacify the renal collecting system.
Greater amounts of contrast cause overdistension and extravasation of infected urine resulting in urosepsis [6].
After correct positioning is confirmed,
a guidewire is advanced out of the calyx towards the ureteropelvic junction.
Following this,
fascial dilators are used to expand the track to one french size larger than the chosen drainage catheter.
We use an 8F pigtail catheter.
The position of the catheter is then confirmed and the catheter attached to a drainage bag and sutured to overlying skin [8].
Functional improvement will be seen in a day or two,
and the nephrostomy tube is replaced with a ureteral stent.
Balloon ureteroplasty can be performed at the same time to ensure long-lasting ureteral patency.
We use a high-pressure 8mm diameter balloon for ureteroplasty.
The ureter can then be held open with a stent,
usually in place for 4-6 weeks [9].
There may be a ureteral leak,
in which case this should be treated with prolonged nephrostomy drainage (with or without stenting).
Recurrent strictures will require eventual surgical re-construction. If surgery is not feasible,
then long term plastic stenting with regular exchange,
or metal ureteral stenting should be considered.
Although measures are taken to reduce the incidence of complications,
major complications occur in 1-4% of individuals [3],
and can be categorised into injury to adjacent structures,
severe bleeding and severe infection [8].
Temporary haematuria occurs in most patients,
but the risk of severe bleeding requiring transfusion is 1-3%.
Transient low-grade fever occurs in almost many cases,
and septic shock with pyonephrosis is a risk [7].
Urosepsis has a high morality/morbidity rate and so prevention is key.
Our population
Between 1994 and 2013,
1477 kidney transplant procedures were performed at our institution.
A total of 73 nephrostomies (PCN) were performed in 52 patients following renal transplantation.
39 patients had 1 nephrostomy,
8 patients had 2 PCNs,
2 patients had 3 PCNs,
1 had 4 PCNs and 8 PCNs were performed in 1 patient.
The mean age was 47 years (Range,
18-72 years) and gender distribution was 50 males (68.5%) and 23 females (31.5%).
The technical success rate was 100%.
There were 3 significant bleeds - one was treated expectantly and one required bladder washouts and blood transfusion.
The third case required embolisation.
There were no cases with septicaemia or bowel injury and no graft losses secondary to renal intervention.
We present some instructive cases from our practice:
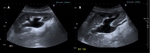
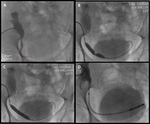
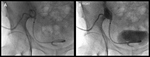
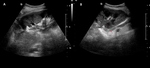
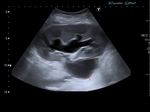
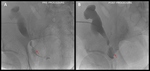
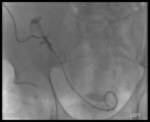
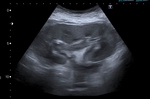
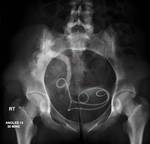
Case 1 – A 69 year old man cadaveric renal transplant recipient.
Past medical history of renal failure,
secondary hypertension,
glomerulonephritis and diabetes mellitus.
(Figs 1-4)
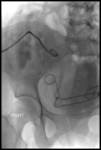
Case 2 – A 45 year old male cadaveric renal transplant recipient.
This example illustrates a ureteric anastomotic leak,
causing hydronephrosis which was successfully stented.
(Figs 5-9)
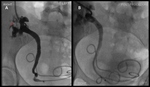
Case 3 – An 18 year old female live renal transplant recipient.
Duplex transplant kidney nephrostomy complicated with renal urinary leak.
(Figs 10-12)