Introduction:
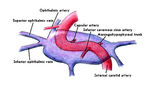
CCF is an abnormal communication between carotid arterial system (Internal Carotid Artery -ICA- or External Carotid Artery -ECA-) and cavernous sinus (CS) (Fig.
1).
Increased pressure within the CS seems to be the mainstay of pathophysiology,
although arterial steal and increased flow plays an important role.
Classification and etiology:
There are several classifications of CCF´s,
according to its etiology (traumatic or spontaneous),
flow dynamics (high or low flow) and anatomy (direct or indirect).
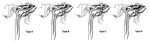
Barrow et al [1] made a classification based on their arterial supply (Fig.
2).
Type A fistulas are direct connections between the intracavernous ICA and CS,
usually associated with high flow rates,
and are mostly secondary to trauma (facial and skull base fractures) [2].
Type B,
C and D are low flow indirect fistulae:
- Type B fistulas have dural branches of ICA to CS,
and are relatively uncommon.
- Type C fistulas have arterial supply from dural branches of ECA.
- Type D fistulas have dural ICA and ECA branches to the CS; is the most prevalent indirect fistula.
Spontaneous CCF´s may fall into any of the previous types.
The most frequent location of direct CCF is at the proximal horizontal intracavernous segment of the ICA near the inferolateral trunk.
Traumatic disruption of the vessel wall is the most common cause for direct CCF´s (trauma,
iatrogenic),
although 20% of cases are regarded as spontaneous (conditions that predisposes weakness of the ICA wall,
e.g.
Ehlers-Danlos syndrome) [3].
Indirect CCF´s are usually spontaneous and occur frequently in post-menopausal women.
Predisposing factors include hypertension,
diabetes,
pregnancy,
collagen vascular disease,
among others.
Sometimes it can resolve spontaneously without treatment [4,
5].
Clinical Features:
Clinical presentation is consequence of the elevated intracavernous pressure.
Moreover,
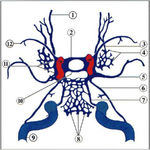
other factors like dominant pattern of venous drainage (Fig.
3),
the size and location of CCF and the presence of collateral vessels (arterial or venous) are important in this setting.
For example,
principal drainage into superior and inferior ophthalmic veins present with orbital symptoms [4].
In direct,
high-flow CCF´s,
symptoms appear suddenly.
The Dandy´s triad (pulsatile exophthalmos,
bruit and chemosis) is not completely observed in all patients,
and is accompanied by other clinical features (diplopia,
pain,
cephalic bruit,
ophtalmoplegia,
visual loss).
Visual loss is one of the most feared complications and requires immediate treatment [6,
7].
Other less common clinical manifestations includes intracranial haemorrhage (secondary to drainage into sphenoparietal sinus and deep middle cerebral vein) and external haemorrhage (otorrhagia,
epistaxis) [3,
8].
Regarding indirect CCF´s,
the onset of symptoms is not as sudden as direct CCF and progess insidiously,
showing progressive glaucoma,
proptosis or red eye.
Differential diagnosis:
Includes a wide spectrum of pathologies (Table 1),
so patients may be carefully evaluated before the presence of vascular pathology is recognized.
|
Vascular
- Marginal sinus fistulas
- Anomalous intracranial venous drainage
- CS thrombosis
|
|
Inflamatory,
allergic,
infectious
|
|
Endocrine
|
|
Other
- Frontal sinus mucocele
- Osteoma
- Ocular neoplasms
- Hemangioma
- Fibrous dysplasia
|
DIFFERENTIAL DIAGNOSIS OF CCF
Table 1.