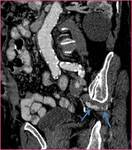
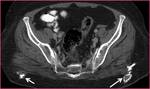
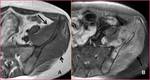
Gluteal arteriovenous malformations (AVM) (Figure 1): AVM’s are congenital vascular lesions that arise secondary to a developmental defect in the vascular system in the 4-6th gestational weeks.
There is a direct connection between the artery and the vein,
but no capillary bed exists.
AVM’s contain tortuous dilated feeding arteries and draining veins.
AVM’s can cause cosmetic defects,
and compression to the peripheral nerves leading to pain and functional disorders.
Eventually,
this abnormal hemodynamic cause steal phenomenon,
venous hypertension and ischemic ulcers,
dermatitis due to venous stasis and progress to gangrene,
dangerous bleeding and cardiac insufficiency.
Imaging studies play an important role in differential diagnosis.
Angiography is the gold standard technique in precise diagnosis and also it is a very important tool in planning the therapy.
MRI is especially valuable for evaluating the extent of the lesion and for detecting the relationship between the lesion and the adjacent anatomic structures.
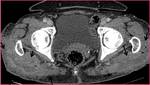
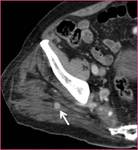
Superior gluteal artery (SGA) aneurysm (Figure 2): Aneurysm of SGA is rare,
and can be detected after pelvic trauma,
fracture,
penetrating injuries and iatrogenic causes (e.g.,
bone marrow biopsies). For this reason most of them are pseudoaneurysms.
Apart from this,
true aneurysms may arise secondary to atherosclerosis,
connective tissue disorders (PAN,
Ehlers-Danlos,
etc),
infections (septic emboli and bacterial endocarditis).
Symptoms include gluteal pain,
pulsatile mass,
findings mimicking degenerative disk disease,
sciatic nerve palsy,
and gluteal compartment syndrome.
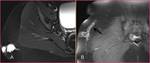
Hidradenitis suppurativa (HA) (Figure 3): HA is a chronic suppurative disease of the skin characterized with occlusion of the apocrine sweat glands.
Common sites of occurrence include axilla,
umbilicus,
mammary,
perineal,
gluteal,
inguinal regions where the regions rich in apocrine sweat glands.
Usually,
HA manifests by recurrent abscess,
multiple sinus tracts,
acute folliculitis,
infection of contiguous glands and subcutaneous fatty tissue.
Squamous cell carcinoma is rare but the most serious complication.
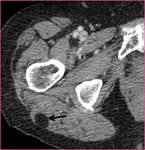
Gluteal abscesses (Figure 4): Abscesses are usually encountered in immuncompromised patients.
Staphylococcus aureus,
tuberculosis,
Brucella,
Salmonella can be identified in the gluteal region abscesses.
Usually clinical history and physical examination are sufficient for abscess diagnosis,
however with the help of cross sectional imaging methods like CT or MRI,
the extension of the abscess can be evaluated easily.
And also if necessary,
percutaneous drainage can be made under CT guidance.
Perianal fistula (Figure 5): Fistula is defined as an abnormal connection between two structures or organs or between an organ and the surface of the body.
Perianal fistula is a connection between anal canal and the skin of perineum.
Because of its significant morbidity,
it is a serious problem.
It predominantly affects young males.
Pain and discharge are the most common presenting symptoms.
Although most of the cases are idiopathic,
fistulas occur secondary to Crohn’s disease,
tuberculosis,
pelvic infections and malignancies,
diverticulitis,
traumatic labor,
and radiotherapy.
MRI is superior to other imaging modalities for detection of the type of the fistula,
for evaluation of the anatomic relationship between the fistula and the adjacent structures,
and for identification of secondary fistulas and abscess formations.
Invasion of anal cancer (Figure 6): Anal canal cancers account for 1.5 % of all gastrointestinal tumors.
Histologically,
most of them (85%) are squamous cell type.
Previous radiation,
Crohn disease,
chronic anal fistulas,
etc are predisposing factors.
Anal canal cancers are locally extensive lesions,
so invasion of adjacent tissues may be seen on imaging methods.
Sinus complicated with a sebaceous cyst (Figure 7): Sebaceous cysts are subcutaneous lesions filled with oily material.
They may become infected and form abscesses.
Hematoma (Figure 8): Hematoma in the gluteal region may occur due to blunt or penetrating-perforating traumas,
antithrombotic therapy,
coagulation disorders,
and iatrogenic injuries.
Clinically,
patients present with palpable lump,
pain,
and skin discoloration.
Massive hematomas may cause gluteal compartment syndrome.
In chronic phase it can be confused with soft tissue tumors.
MRI is a valuable method in differential diagnosis of complicated cases.
Lipoma (Figure 9): Lipoma is the most common mesenchymal soft tissue tumor in adults,
composed of mature fat cells.
It usually presents as a painless soft tissue mass,
although larger ones can be painful when they compress peripheral nerves.
Most of them are subcutaneous,
but sometimes can be located deeply (intra-intermuscular).
There is no need to therapy in asymptomatic patients.
However in case of mobility restriction,
pain and cosmetic problems ,
or if features suggesting malignancy (old age,
large size,
presence of thick septa,
presence of nodular and/or globular nonadipose mass like areas,
and decreased percentage of fat composition) exist,
surgery must be planned.
Liposarcoma (Figure 10): Liposarcoma is the second most encountered soft tissue tumor in adults.
It is frequently seen in males in 4th to 6th decades.
It arises from multipotential primitive mesenchymal cells.
Usually it occurs in the extremities,
retroperitoneum and inguinal regions.
One of the most prognostic factors is its anatomic location.
Prognosis is better in superficial lesions than the lesions located deeply such as in retroperitoneum or in mediastinum.
Dystrophic calcifications secondary to intramuscular injections (Figure 11): These calcifications are seen very frequent on plain films and on CT’s.
They are also known as injection granulomas.
It forms due to making the injection subcutanously instead of intramuscular.
Then on injection site,
fat necrosis,
scar formation and calcium deposition occurs.
Its appearance and location are characteristic,
and usually does not cause any diagnostic confusion.
Differential diagnosis is made whether the lesion is calcified or not.
If it is noncalcified soft tissue sarcoma,
subcutaneous metastasis,
and if calcified infections (e.g.,
cysticercosis),
neoplasms (e.g.,
osteosarcoma,
tumor necrosis),
autoimmune diseases (e.g.,
dermatomyositis,
scleroderma) and trauma (heterotopic ossification) must be considered in the differential diagnosis.
Myositis ossificans (MO) (Figure 12): MO is a nonneoplastic,
heterotopic ossification of soft tissues (skeletal muscle,
tendon,
fascia,
aponeuroses,
etc).
MO tends to be solitary,
localized,
and self-limited.
In its pathogenesis,
generally there is a trauma inducing the differentiation of mesenchymal cells into fibroblasts and osteoblasts.
These cells make osteoid and deposits osteoid in the lesion moving towards centrally.
As the lesion gets matured,
lamellar bone forms in its periphery.
At early phase,
it may be confused with osteosarcoma.
Most of them (approximately 80%) develop in thigh and arm.
Besides it can occur in the intercostal space,
pectoral muscle and gluteal region as well.
Malignant mesenchymal tumor (Figure 13): Pelvic malignant soft tissue tumors can infiltrate and extend into adjacent structures and can cause destruction in the bones.
Ewing’s sarcoma (Figure 14): Ewing’s sarcoma is the second most encountered primary malignant bone tumor in children and adolescents.
The most common sites are pelvis and lower extremities.
In 12.5% of the patients iliac bone is involved.
In general,
it is accompanied by a soft tissue component.
Extraosseous extension is frequent,
and the lesion is usually lytic.
Prognosis is poor in tumors located in pelvic bones.
Metastasis (Figure 15): Although it is not frequent,
metastatic disease as single or multiple nodules can be seen in the gluteal region.
Lymph node metastasis (Figures 16,
17): Lymphoproliferative disorders,
and infectious-inflammatory and neoplastic pathologies of anorectal canal,
perineum,
gluteal tissues,
can cause enlargement of gluteal lymph nodes.