The mean age of the patients in the study group,
182 women,
was 56 years (range 31-93 years).
Relative to localization of the tumor,
81 were located in the right breast,
100 in the left breast and 1 tumor was bilateral,
total 183 axillae included in the study.
Out of these,
74 patients had surgery as the primary treatment and 72 had neoadjuvant treatment; after surgery,
19 patients are in palliative care,
11 died and 6 lost follow up in our institution.
The primary cancer tumor mean size in the surgical specimen was 2.8 cm.
There were 165 invasive carcinoma of no special type (invasive ductal carcinoma),
10 invasive lobular carcinoma,
2 metaplastic carcinoma,
4 mucinous carcinoma,
1 invasive micropapillary carcinoma and 1 secretory carcinoma.
Patients were eligible for neoadjuvant treatment according to the severity criteria: patients with abnormal lymph nodes on ultrasound,
or with positive FNA cytology result,
or with palpable lymph nodes or with tumors above the stage T3.
For analysis,
we divided the study group in two: without neoadjuvant treatment (WONT) and with neoadjuvant treatment (WNT).
The mean age in the subgroup WONT was 58 years old and 78.6% of these patients were postmenopausal.
In the subgroup WNT the mean age was 54 years old and 61.6% of these patients were postmenopausal (p=0.034).
In the subgroup WONT most FNA cytology results were negative,
most lymph nodes had normal cortical thickness and preserved fatty hilum.
The lymph nodes were smaller and the tumor size at mammography,
ultrasound and MRI were also smaller compared with the subgroup WNT.
In the subgroup WONT we had 53.4% of breast conserving surgery versus 46.6% of mastectomy and in the subgroup WNT we had 70.4% of mastectomy versus 29.6% of breast conserving surgery (p=0.006).
The feature distribution on these two subgroups are shown in Tables 1 and 2.
In the subgroup without neoadjuvant treatment (WONT),
we correlated FNA cytology results with lymph node surgical pathology results and also the lymph nodes ultrasound features with lymph node pathology results.
Considering that 9 of the 15 lymph nodes with inconclusive FNA results had normal appearance at ultrasound,
we included FNA inconclusive results in FNA negative results.
Also FNA suspect results were included in FNA positive results.
Ultrasound-guided fine needle aspiration Sensitivity,
Specificity,
Positive Predictive Value (PPV) and Negative Predictive Value (NPV) were 39.3%,
92.6%,
81.2% and 65.5% in this subgroup (p=0.01).
Ultrasound Sensitivity,
Specificity,
Positive Predictive Value (PPV) and Negative Predictive Value (NPV) were 72.7%,
53.6%,
55.8% and 70.9% (p=0.022) according with lymph node surgical pathology results,
to differentiate normal and abnormal lymph nodes.
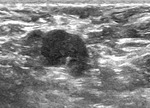
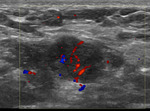
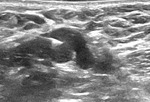
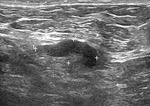
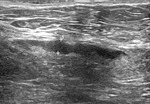
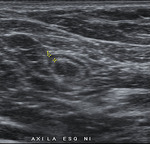
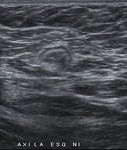
When we correlated lymph nodes ultrasound characteristics with metastatic involvement,
in the subgroup without neoadjuvant treatment,
features most associated with malignancy were diffuse cortical thickening and partial or complete fatty hilum obliteration as shown in Table 3; (Fig.
1-3).
There was no statistical difference in size of lymph nodes,
morphology,
margins and palpability.
As we expected tumor size was bigger in patients with metastatic involvement of the axilla.
Comparing in this subgroup without neoadjuvant treatment patients with metastatic lymph nodes had mean tumor size at mammography,
MRI and surgical specimen of 3.4 cm,
4.6 cm and 3.2 cm respectively and patients without metastatic involvement had mean tumor size at mammography,
MRI and surgical specimen of 2.3 cm,
3.0 cm and 2.3 cm respectively.
The subgroup with neoadjuvant treatment (WNT) was divided in two: with partial or negative response and with complete response [12].
There were 62 patients with partial / negative response and 10 patients with complete response.
In the group with partial / negative response ultrasound-guided fine needle aspiration Sensitivity,
Specificity,
Positive Predictive Value (PPV) and Negative Predictive Value (NPV) were 64.8%,
55.2%,
64.8% and 55.2% (p=0.259).
Ultrasound Sensitivity,
Specificity,
Positive Predictive Value (PPV) and Negative Predictive Value (NPV) in this group were 97.3%,
13.7%,
59.7% and 80.0% (p= 0.085),
according with lymph node surgical pathology results,
to differentiate normal and abnormal lymph nodes (Fig.
4,5).
As we can see in these patients with neoadjuvant treatment there was no statistical difference (p>0.05).
In the group with complete response it was not possible to calculate the values of FNA and ultrasound once all lymph nodes were negative at surgical pathology.
Finally,
when we correlated ultrasound with FNA cytology results,
ultrasound Sensitivity,
Specificity,
Positive Predictive Value (PPV) and Negative Predictive Value (NPV) to differentiate normal and abnormal lymph nodes were respectively 100%,
38%,
55% and 100% (p<<0,01),
since all lymph nodes classified on ultrasound as normal (n=39) had negative (n=29) or inconclusive (n=10) FNA cytology results (Fig.
6,7).