This poster is published under an
open license. Please read the
disclaimer for further details.
Keywords:
Neoplasia, Multidisciplinary cancer care, Cancer, Surgery, Diagnostic procedure, Decision analysis, MR-Diffusion/Perfusion, MR, Oncology, Abdomen
Authors:
J. R. Ramos Rodriguez, M. Atencia Ballesteros, M. D. M. Muñoz Ruiz, A. J. Márquez Moreno, M. D. Domínguez Pinos; Málaga/ES
DOI:
10.1594/ecr2015/C-0152
Methods and materials
Patients were prospectively followed after pelvic MRI for rectal cancer preoperative staging was performed with the following MRI sequences:
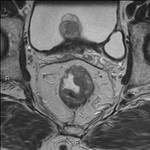
· AXIAL OBLIQUE T2 (TSE): Thin slices (3 mm maximum) perpendicular to tumor,
to accurately assess the tumor and its relationship to the rectal wall,
mesorectal fascia and pelvic organs.
· CORONAL T2 (TSE): Especially useful for patients with low rectal cancer to evaluate elevator muscles,
sphincter complex,
intersphincteric plane and relationship with rectal wall.
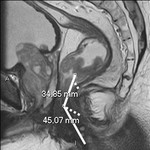
· SAGITAL T2 (TSE): Mainly to calculate the distance to the top edge of the anal sphincter complex and anal verge.
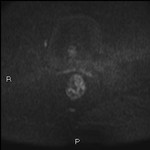
· AXIAL DWI (Difussion): Very useful to locate the tumor without use of cleansing enemas or gel.
May be useful for detection of extramural venous invasion,
location of lymph nodes and evaluation of the response after chemotherapy and radiotherapy.
· ADDITIONAL SEQUENCES (T1 and STIR): Primarily for assessment of regional or distant involvement (lymph nodes,
bone metastases,
etc)
MRI was performed avoiding administration of rectal gel or cleansing enemas in order to prevent discomfort or injury to patients and avoid overdistension of rectal walls that can distort the assessment of tumor depth.
MRI Scan was assessed by a radiologist with more than 5 years of experience,
studying depth of tumor Infiltration (T stage) [1,2,3],
involvement of the mesorectal fascia (fascia is preserved when tumor is farther than 2 mm) [4],
distance to anal verge (considering a margin of error of + / - 1 cm) and nodal involvement (N stage) [2] using TNM classification (American Joint Committee on Cancer/International Union Against Cancer) These results were compared with histological analysis of the tumor after resection.