Inclusion of patients
This was a prospective,
monocentric,
institutional review board approved study and patient’s enrollment was performed at the Unit of Infectious Diseases of our Institution.
From January 1st,
2013,
through December 31st,
2013,
81 consecutive untreated patients with chronic viral C hepatitis were enrolled into the study after giving written informed consent.
All patients were untreated (i.e.
not under interferon–based therapies) at the time of enrollment.
Exclusion criteria were the presence of major contraindications to 1.5T MRI (e.g.
cardiac pacemaker,
claustrophobia,
foreign bodies and implanted medical devices with ferromagnetic properties [28]) and/or to liver biopsy (e.g.
uncorrectable coagulopathy [29]).
All included patients underwent MRI,
transient elastography (TE) and liver biopsy within a time interval <10 days.
Severe respiratory and motion artifacts on MR images were considered as an additional,
post–MRI exclusion criteria to avoid unreliable measurements of MRI PDFF.
After inclusion,
the following laboratory values were obtained for all patients: aspartate aminotransferase (AST,
expressed in IU/l),
alanine transaminase (ALT,
expressed in IU/L),
gamma–glutamyl transpeptidase (GGT,
expressed in IU/L),
total bilirubin (expressed in mg/dL),
platelet count (103 cells per μL of blood),
and serum ferritin levels (expressed in ng/mL).
Serum HCV–RNA levels were assessed in all patients by means of a quantitative method (real time polymerase chain reaction),
and expressed in IU/mL.
MRI examinations and PDFF measurements
MRI of the liver was performed in the supine position on a 1.5T MRI scanner (Signa HDx,
General Electric Medical Systems,
Milwaukee,
WI,
USA) using a phased array,
eight–element,
flexible torso coil.
All patients were carefully instructed to suspend respiration at the end of inspiration during the MRI sequence acquisition.
A two-dimensional,
spoiled,
multiecho gradient–echo sequence with 16 echoes was performed in the axial plane to measure hepatic PDFF.
The parameters of this sequence were adjusted in order to achieve a complete correction for confounding factors such as T1 bias,
T2* decay,
and water–fat signal interference [10,
12,
20].
To minimize T1 effects,
a 20° flip angle was used at repetition time (TR) ranging from 120 to 270 msec,
adjusted by the technologist to individual breath-hold capacity.
To estimate water–fat signal interference and T2* effects,
16 echoes were obtained at serial opposed–phase and in–phase echo times (TE) (1.1,
2.25,
3.4,
4.55,
5.7,
6.85,
8,
9.15,
10.3,
11.45,
12.6,
13.75,
14.9,
16.05,
17.2,
18.35 msec) during a single breath hold of 12–34 seconds.
Other imaging parameters were: 10 mm section thickness,
0 intersection gap,
125 kHz bandwidth,
one signal average,
and rectangular field of view with a 128×96 matrix adjusted to individual body habitus and breath–hold capacity.
The multiecho gradient–echo MR images were exported in DICOM format for offline post–processing.
Image interpretation and data analysis
All MRI datasets derived from multiecho gradient–echo images were post–processed by a single experienced abdominal radiologist.
The quantification of liver PDFF was performed with a publicly available software named C–Iron (Camelot Biomedical Systems SRL,
Genoa,
Italy; website: http://c-iron.camelotbio.com).
C–Iron is a stand–alone software tool dedicated to the voxel–wise measurement of T2* decay for the quantification of iron overload and liver PDFF.
Once acquired,
the multiecho gradient–echo MR images are imported into the software.
T2* values and PDFFs are estimated by fitting the MRI signal (S) acquired at different TEs with the following decay model proposed by Bydder et al.
[20]:
|S(TE)| = sqrt [S12 exp (-2TE/T2,w*) + S22 exp (-2TE/T2,f*) + 2 S1S2 exp (-TE/T2,w*) exp (-TE/T2,f*) cos (ωTE)]
where S1 and S2 are the signal amplitudes of water and fat respectively,
T2,w* and T2,f* are the transverse relaxation times of water and fat,
and ω=2π/4.6 ms is the chemical shift between water and fat at 1.5T.
The algorithm simultaneously estimates T2* and PDFF in each voxel of the image by using nonlinear least–squares fitting from all 16 echoes,
assuming exponential decay and considering that fat has its own inherent T2 decay of 12 ms.
The quality of fit is assessed by means of the coefficient of determination R2 and pixels with low–quality fit are excluded from further processing by applying appropriate thresholds on the R2 value.
The PDFF is then calculated by the following formula: FF=S2/(S1+S2).
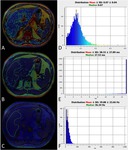
A color–coded map reflecting the estimated PDFF values in each pixel of the image is displayed and juxtaposed on the corresponding axial MRI slice.
The histogram of pixel distribution with mean,
median and standard deviation of the PDFF values,
is computed in a freehand,
elliptical or rectangular user–adjustable ROI.
A single abdominal radiologist,
blinded to the results of both TE and histology,
performed ROI positioning.
A single freehand ROI was drawn in a mid–hepatic axial slice including the right lobe of the liver and systematically excluding large blood vessels,
biliary ducts and focal lesions.
The mean area of the ROIs was of about 40–60 cm2,
depending on patient’s anthropometric features (Figure 1).
MRI PDFF and T2* decay were calculated in the same ROI.
Clinically significant hepatic iron overload was defined by MRI T2* values less than 6.3 ms,
corresponding to a liver iron concentration in dry tissue (LIC dry weight) of 4.2 mg/g [30,
31].
Transient elastography
Transient elastography (TE) is a corroborate method for the assessment of liver fibrosis in patients with chronic C hepatitis.
TE was performed with FibroScan (Echosens,
Paris,
France) with liver stiffness measurements expressed in kiloPascals (values between 2.5 kPa and 75 kPa are expected) [32].
Acquisitions that do not have a correct vibration shape or a correct follow–up of the vibration propagation are automatically rejected by the software.
Measurements of liver stiffness were performed on the right lobe of the liver through intercostal spaces in correspondence to the mid–axillary line,
while patients were lying in the supine position with the right arm in maximal abduction.
In all included patients,
TE measurements were successfully acquired (i.e.
10 correct measurements with an interquartile range lower than 30% of the median liver stiffness value [33]).
Liver biopsy
Ultrasound–assisted percutaneous liver biopsy was performed with an intercostal approach using 15– to 18–gauge needles.
All biopsy specimens were fixed in formalin and embedded in paraffin.
A single expert liver pathologist,
blind to the results of both TE and MRI,
read the specimens on site.
Fibrosis was semi–quantitatively evaluated and staged on a 5–point scale from 0 to 4 according to the METAVIR scoring system (F0,
absent; F1,
enlarged fibrotic portal tract; F2,
periportal or initial portal–portal septa but intact architecture; F3,
architectural distortion but no obvious cirrhosis; and F4,
cirrhosis) [34].
Necroinflammatory activity,
represented by piecemeal necrosis and focal lobular necrosis,
was semi–quantitatively evaluated by using the histological activity index described in the METAVIR system,
and graded as follows: 0,
no activity; 1,
mild; 2,
moderate; 3,
severe [34,
35].
Liver steatosis was determined by estimating the percentage of fat–containing hepatocytes on haematoxylin–eosin stained specimens,
and graded according to the method of Kleiner et al.
[36]: S0,
steatosis in fewer than 5% of hepatocytes; S1,
5%–33% of fatty hepatocytes; S2,
34%–66%; and S3,
more than 66%.
We also considered the percentage of fatty hepatocytes as an absolute value which was defined as histological fat fraction.
Following the clinical standard,
a Perl’s Prussian blue reaction was applied to detect the presence of hemosiderin granules in biopsy specimens.
The following ordinal 4–point scoring system was employed: grade 0,
no iron deposits; grade 1,
mild; grade 2,
moderate; grade 3,
high iron content [37].
Statistical analysis
Descriptive statistics were produced for demographic,
clinical,
and laboratory characteristics of patients.
Categorical data were expressed as number and percentage,
while continuous data as mean and standard deviation (SD),
or median and range (from minimum to maximum).
The normal distribution of different datasets was assessed by means of the D'Agostino–Pearson test.
Nominal statistical significance was defined with a P of 0.05.
The correlation of histological FF with MRI PDFF was tested by means of the Spearman's rank test,
using both the arithmetic mean and the median of MRI PDFF values.
Spearman's rho (r) values were interpreted as follows: for values of r of 0.9 to 1,
the correlation is very strong; for values of r between 0.7 and 0.89,
correlation is strong; for values of r between 0.5 and 0.69,
correlation is moderate; for values of r between 0.3 and 0.4.9,
correlation is moderate to low; for values of r between 0.16 and 0.29,
correlation is weak to low; for values of r below 0.16,
correlation is too low to be meaningful.
Since the median MRI PDFF showed a better correlation with the histological FF,
this parameter was adopted for the subsequent statistical analysis.
The correlation of median MRI PDFF values with histological FF was also tested using a partial correlation model,
where liver stiffness,
expressed in kPa,
and T2* decay,
expressed in ms,
were introduced as confounding covariates.
The cohort of patients was further stratified according to each histological feature of the METAVIR system,
including fibrosis stage (F),
inflammatory activity (A) and steatosis grade (S).
Box plots were used to study the distribution of MRI PDFF according to each stage of fibrosis,
inflammatory activity and steatosis,
and the presence of significant differences in the median MRI PDFF values among subgroups of patients was tested using the non–parametrical Kruskal–Wallis test.
After a positive Kruskal–Wallis test (p–value <0.05),
a post–hoc analysis was conducted performing pairwise comparisons between subgroups.
The diagnostic performance of MRI for detecting the correct histological grade of hepatic steatosis was assessed by using receiver operating characteristic (ROC) curves.
For the ROC curve analysis,
the area under curve (AUC),
optimal cutoff values,
sensitivity,
specificity,
positive and negative predictive values were calculated.
Optimal cutoff values of MRI PDFF were chosen to maximize the sum of sensitivity and specificity for two steatosis thresholds: S0 vs S1–S2 (S≥1) and S0–S1 versus S2 (S=2).
Ultimately,
the MRI PDFF was introduced as dependent variable in a multiple regression model,
using patient’s age,
BMI,
TE liver stiffness values,
MRI T2* values,
METAVIR stage of fibrosis,
inflammation,
steatosis,
and histological FF as independent variables.