The most notable characteristic of Crouzon syndrome is craniostenosis,
a deformity of the skull that results from premature closure of the sutures between the cranial bones.
The precise cause of premature sutural closure has not been fully clarified.
In the normal patient,
sutures close when the growth of the brain stops.
Recent molecular biologic studies suggest that interactions of fibroblast growth factors (FGFs) and their receptors (FGFR) influence the balance between the proliferation of osteoprogenitor cells and the differentiation of new bone in the membranous bones of the calvarium.
This processes take place in the sutures.
When the balance is shifted the sutures appear to close.
Gene encoding fibroblast growth factor receptor-2 (FGFR2) participate in molecular pathways involved in this process. 7
Because the skull can’t expand perpendicularly to the fused suture,
it compensates by growing in the parallel direction to the closed suture,
which causes changes in the shape of the scull.
The severity of the malformation depends on which sutures close,
the point in the developmental process where the closure occurred,
and the success or failure in compensating by expansion of the other sutures.
The first symptoms are usually noted in newborn period.
In some cases it can occur later,
during the first two or three years of life,
when the child exhibits neurodevelopmental delays.
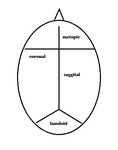
The deformity varies significantly depending on the suture or sutures involved.
(Fig.
1)

Fig. 1: The top view of human skull showing cranial sutures.
We usually observe fusion of both coronal sutures,
which separate the two frontal bones from the parietal bones.
It leads to calvarial deformity named brachycephaly,
which derives from Latin and means "short" and "head".
As a result,
the head of patient is disproportionately wide and shortened in sagittal diameter.
(Fig.
2-6)

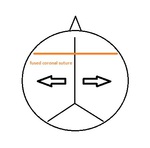
Fig. 2: Brachycephaly caused by premature fusion of coronal sutures.
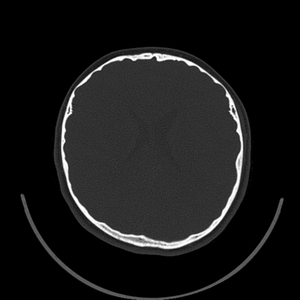
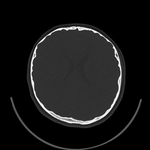
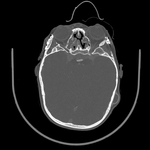
Fig. 3: CT, axial view of skull showing brachycephaly.

Fig. 4: CT, axial view of skull showing brachycephaly.

Fig. 5: Brachycephaly in 18-year-old patient with Crouzon syndrome.

Fig. 6: Brachycephaly in 18-year-old patient with Crouzon syndrome.
In many cases,
not only the coronal sutures are fused,
but other (mainly the saggital suture) as well.
It result in oxycephaly.
In this type of cephalic disorder the skull is elongated in craniocaudal diameter and pointed shape.
(Fig 7-11)

Fig. 7: Oxycephaly caused by premature fusion of coronal and sagittal sutures.

Fig. 8: Oxecephaly in 8-year old patient with Crouzon syndrome.

Fig. 9: Oxecephaly in 8-year old patient with Crouzon syndrome.

Fig. 10: Radiograph showing oxycephaly.
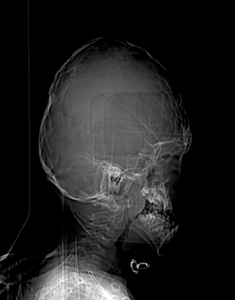
Fig. 11: Radiograph showing oxycephaly.
Other forms of skull deformity including scaphocephaly,
trigonocephaly as well as cloverleaf skull have been reported when others sutures are prematurely fused. 8
Children with Crouzon syndrome have a face,
which once seen,
is not forgotten.
(Fig.
12-15)

Fig. 12: 11-year-old girl with Crouzon syndrome.

Fig. 13: 11-year-old girl with Crouzon syndrome.

Fig. 14: younger sister of the girl from Fig.13 (also diagnosed with Crouzon syndrome)

Fig. 15: Father of these two girls (not diagnosed with Crozuon syndrome)
It is due to maxillary hypoplasia (moderate to severe) and midface retrusion,
caused by lack of growth at the maxillary synchondroses.
Hypoplastic maxilla is flatter and wider than a normal one.
(Fig.
16)

Fig. 16: Radiograph showing midface hypoplasia.
The anterioposterior dimension of the maxillary dental arch is shortened causing tooth crowding.
(Fig.17)

Fig. 17: Hypoplasic maxilla with small dental arch.
Shenoid bone is also changed,
pteroid wings are widened and retruded.
Midface hypoplasia associated with normal growth of mandibula results in malocclusion and mandibular pseudoprognathism.
Dropping of the lower lip results in a half-open mouth.
Psittichorhina (beak-like appearance of the nose) is also a typical characteristic of Crouzon syndrome. 9,10
All these malformations may cause some degree of nasal airway obstructions due to compression of the nasal passages,
often reducing airflow through the nose and therefore causing mouth breathing.
Even up to 50% of infants develop obstructive sleep apnea syndrome,
which not treated may lead to respiratory infections,
cognitive dysfunction,
development delay,
cor pulmonale or sudden death.
Other children with severe breathing difficulty require tracheostomy.
Unusual resonance and speech patterns can develop from either the small nose,
the high palate,
or mandibular malocclusion.
(Fig.
18)

Fig. 18: Hypoplasic maxilla with small dental arch.
The orbits are shallow,
the middle cranial fossa is displaced anteriorly and inferiorly,
the maixilla is hypoplastic which shortens the orbit anterioposteriorly.
This above changes result in considerable reduction of orbital volume which leads to significant exophthalmos,
a feature occurring in 100% of the cases.
(Fig.19)

Fig. 19: CT, axial view showing hyperthelorism
Additionally hyperthelorism (excessive distance between both eyes) and divirgent strabismus are observed.
Visual disturbance results from corneal erosion due to exposed conjunctivitis and keratitis.
In severe cases of Crouzon syndrome there are other possible abnormalities,
including imbalance of extraocular muscles or progressive optic nerve atrophy in cases associated with intracranial hypertension. 11
Moreover,
low-set ears and ear canal stenosis or atresia are observed.
Conductive hearing loss may occur due to repeated middle ear infections that result from the cleft palate and bifid uvula and the high arching palate.
This can lead to speech difficulties.
(Fig.
20)

Fig. 20: 10-year-old girl with Crouzon syndrome, low-set ear.
In Crouzon syndrome premature fusion of the sutures causes abnormal skull expansion and decreased cranial volume in presence of rapidly growing brain.
Over the first year of life,
the brain triples in volume to reach two thirds of its adult size.
It continues to grow rapidly over the next 2 years,
then growth continues more gradually with the brain reaching adult size between 6 and 10 years of age.
The global distortion of the brain in Crouzon syndrome is mechanical and depends on deformity of the skull.
(Fig.
21-23)

Fig. 21: MRI axial plane, distortion of the brain caused by skull deformity.

Fig. 22: MRI axial plane, distortion of the brain caused by skull deformity.

Fig. 23: MRI sagittal plane, distortion of the brain caused by skull deformity.
The most serious complication associated witch craniostenosis is elevated intracranial pressure,
which is present in around 60% of Crouzon patients. The risk of elevated ICP increases exponentially with the number of affected sutures.
Two responsible for this factors are jugular stenosis and crowding of the posterior fossa.
Progressive fusion of cranial base synchondroses leads to stenosis of the jugular foramina and venous hypertension,
which results in increased resistance outflow of cerebrospinal fluid (CSF).
Small crowded posterior fossa and small size of foramen magnum caused by cranial base stenosis,
leads to mechanical resistance to CSF outflow.
Volume of posterior fossa is additionally decreased by low attachment of tentoral.
These signs are observed especially in patients with early closure of the lambdoid suture.
(Fig.
24)

Fig. 24: MRI sagittal plane, small crowded posterior fossa.
Signs and symptoms of elevated intracranial pressure include a soft spot,
irritability or lethargy and a rapidly increasing head size.
Older children may experience headaches,
vomiting and vision disturbance.
The consequences of delayed diagnosis of elevated intracranial pressure can result in optic atrophy,
blindness and developmental delay.
Ventriculomegaly,
that is dilatation of ventricules,
is present in 50% of patients.
It can be characterized as mild,
moderate or severe (hydrocephalus).
In 70% of these cases it is non progressive,
even if hydrocephalus is present.
There are various theories about the mechanism of hydrocephalus.
One theory suggests that hydrocephalus occurs secondary to the defective formation of the cranium,
so it is reasonable that in many cases the hydrocephalus is non progressive.
Most ventriculomegaly in Crouzon syndrome is asymptomatic and does not necessitate any treatment,
unless there is a clear evidence of significantly raised intracranial pressure.
Treatment of severe hydrocephalus is surgical,
generally utilizing various types of cerebral shunts.
Their role is to drain the excess fluid into other body cavities (peritoneal cavity,
pleural cavity or right antrium),
from where it can be resorbed.
(Fig.
25-27) 12,13

Fig. 25: MRI axial plane, ventriculomegaly.

Fig. 26: MRI coronal plane, ventriculomegaly.

Fig. 27: MRI sagittal plane, ventriculomegaly with cerebral shunt in right lateral ventricle.
Small skull base with high cranial pressure are cause of high incidence of Chiari I malformations.
It is observed in 70% of cases,
especially in patients with early fusion of lamdoid suture.
It is characterized by chronic herniation of cerebellar tonsils of more than 3mm below foramen magnum.
It is generally asymptomatic during childhood,
sometimes manifests with headaches and cerebellar symptoms.
Additionally 20 % of patients develops syringomyelia,
fluid-filed cavity within spinal cord.
It is due to obstruction of CSF circulation from posterior fossa to the caudal space.
(Fig.
28-29) 14,15

Fig. 28: MRI sagittal plane, herniation of the cerebellar tonsils in Chiari I malformation.

Fig. 29: MRI sagittal plane, Chiari I malformation and syryngomyelia.
White matters alterations are also observed in patients with Couzon syndrome.
The constellation of abnormalities that selectively involve white matter involve agenesis or hypoplasia of corpus callosum ,
complete or partial absence septum pellucidum and anomalies of hypocampus.
They are more likely to be the cause of the decreased mental function,
observed in approximately 12% of patients.
In general,
patients diagnosed with Crouzon syndrome have normal intelligence.
(Fig.
30-32) 16,17

Fig. 30: MRI sagittal plane hypoplasia of corpus callosum, absence of septum pellucidum and ventriculomegaly.

Fig. 31: MRI coronal plane, hypoplasia of corpus callosum, absence of septum pellucidum and ventriculomegaly.

Fig. 32: MRI axial plane, hypoplasia of corpus callosum, absence of septum pellucidum and ventriculomegaly.
Venous anormalities are common and may be result of diversion of venous outflow through enlarged emissary veins.
They are vessels which carry the venous blood from intracranial to extracranial veins through enlarged emissary foramina in calvarium.
Venous abnormalities have to be identified before surgical planning.
(Fig.
33)

Fig. 33: MRI, emissary veins going through foramen cecum draining venous blood from superior sagittal sinus to nose.