Although genetic testing is available,
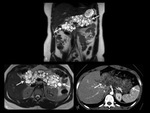
imaging plays a key role in the identification of the most common abdominal manifestations of VHL disease and their subsequent follow-up,
in the screening of asymptomatic gene carriers,
and in their long-term surveillance.
The various lesions can be demonstrated with different imaging techniques such as ultrasonography (US),
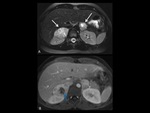
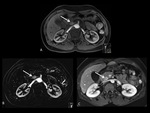
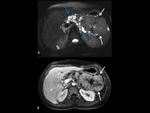
computed tomography (CT) and magnetic resonance imaging (MRI).
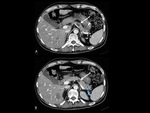
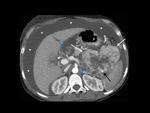
Pancreatic cysts are commonly detected with US or CT (the latter improving the detection of small lesions).
The walls of simple cysts enhance poorly or not at all.
Serous cystadenomas are usually well-circumscribed clusters of small cysts (<2 cm),
which are radially aligned and sometimes show central calcification.
Enhancement occurs at the periphery of these microcysts.
US can show a variety of findings,
such as echogenic masses with or without cystic portions or multilocular cysts.
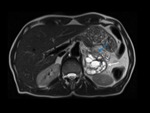
On MRI,
serous cystadenomas have high signal intensity on T2-weighted images.
It may be impossible to distinguish a cluster of benign cysts from serous cystadenomas.
Enhancing septa favor the diagnosis of serous cystadenoma.
The differential diagnosis is not important because these lesions require no treatment.
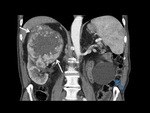
Renal cysts are usually detected with US,
given the purpose to reduce the amount of radiation exposure.
CT is more sensitive than US for detection of small (<2 cm) lesions; cysts demonstrate little or no wall enhancement,
and solid components enhance briskly (50–200 HU) after contrast administration.
MRI is useful in young patients and those with renal failure who still require screening.
Simple cysts are hypointense on T1-weighted images and hyperintense on T2-weighted images,
with no enhancement after administration of gadolinium.
Complex or solid lesions enhance on post-contrast T1-weighted images.
Renal cell carcinomas associated with VHL disease often are multicentric and bilateral solid hypervascular masses or complex cystic masses with mural nodules and thick septa.
CT is more reliable than US for the detection of renal cancer.
MRI is an alternative to CT for patients with impaired renal function and to reduce radiation exposure.
Pheochromocytomas typical appear at CT as solid or complex cystic highly enhancing masses that may have areas of necrosis,
hemorrhage,
and sometimes calcifications.
MRI is superior to CT in evaluating ectopic sites.
At MRI,
the majority of lesions has low or intermediate signal intensity on T1-weighted images and high signal intensity on T2-weighted images and show marked gadolinium enhancement.
Neuroendocrine tumors of the pancreas appear at US as round or oval nodules,
hypoechoic relative to pancreatic parenchyma.
At unenhanced CT,
they are hypo or isoattenuating relative to the normal pancreatic parenchyma.
At MRI,
they are hypointense on T1-weighted images and hyperintense on T2-weighted images,
but not as bright as cysts.
Intense enhancement in the arterial phase is characteristic.
As the tumor enlarges,
calcification,
necrosis,
and cystic degeneration may be seen.