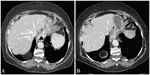
The main source of inspiration for this work was the study by Pickhardt et al.
[1] affirming that small transient sliding hiatal hernias are commonly induced by colonic distention at CTC and should not be reported: their results pushed us to verify if such circumstance was relevant for CT-WE as well,
in order to start correcting a trend of over-reporting and the resulting inappropriate management of these patients.
The evaluation of complex and panoramic exams such as abdominal CT with water enema or CT colonography represents a constant challenge for gastrointestinal radiologists in their daily practice: the number of different findings to consider when assessing this kind of examinations is particularly high and the clinical informations about the recent medical history of the patient play a central role.
Since the amount of unnecessary workup for the wide variety of benign extracolonic findings is particularly relevant for CTC [19,20] radiologists have to correctly assess as well extracolonic findings of CT-WE studies.
It is therefore important to underline,
if possible,
when additional evaluation may not be required.
With this precondition,
incidental findings should be considered according to the clinical background,
and the presence of HH is a classic circumstance in which lack of specific symptoms of gastroesophageal reflux disease may suggest scanty clinical relevance [21].
There are many concerns at this regard.
An inappropriate diagnosis may lead a considerable proportion of patients to consult their own physician which in turn will be tempted to prescribe antacids and antisecretory drugs.
Part of these subjects eventually refer to the gastroenterologist and undergo specialistic investigations.
These latter,
usually consist in barium swallow radiology or esophagogastroduodenoscopy,
which are invasive,
do not affect the management of the patient and do not provide information about the esophageal function and gastroesophageal barrier competency in controlling gastroesophageal refluxes.
Moreover,
although HH itself is not a life-threatening condition its diagnosis may induce on patients,
often not correctly instructed,
worries and psychological distress.
As a consequence of that,
a fictional disease may potentially lead to a true functional disorder that notably impacts on quality of life.
In fact a bi-directionally cause-effect interrelationship exists between gastrointestinal symptoms and psychological distress.
Specifically for the upper digestive tract,
a very recent review reported as a significant proportion of patients - up to 61% - reporting heartburn without any proved pathologies,
improve under antidepressant therapy.
A similar improvement is recorded also for chestpain and esophageal pain thresholds [9].
Beside the costs that burden patients and the healthcare system,
all that has indirect costs for the Society. Several meta-analysis showed a negative impact on work productivity,
defined as absence from work (absenteeism) as well as reduced effectiveness while working (presenteeism) [10,
11,
22].
Although these processes are commonly experienced during our clinical routine,
this study did not asses the effect of the diagnosis of HH on patients’ quality of life,
as it was not part of the aims.
Therefore,
the impact of the misdiagnosis on sociosanitary costs should be considered a mere speculation.
Another concern is who and how should be investigated for HH.
It has wide prevalence in the population,
about 30% even among healthy subjects [23].
No screening and invasive investigations are required in absence of symptoms or alarm signs (i.e.
anemia,
dysphagia,
arrhythmia).
The most frequent finding is the Type I HH (axial) whose major significance is the association with GERD and it is also more difficult to precisely estimate.
When bigger than 2 cm,
it can be easily diagnosed by conventional Barium swallow,
endoscopy and traditional manometry.
However,
the gastroesophageal “barrier” is a dynamic concept where multiple structures vary their anatomic relationship continuously with breathing,
eating,
body movements and even spontaneously.
Moreover,
it can be transitory induced by gastric and esophageal distention during X-ray and upper endoscopy.
Although more sophisticated,
traditional manometry presents also some limitations due to the low number of pressure sensors and the inter-individual variability,
thus potentially jeopardize the reliability of a landmark such as the pressure inversion point.
High-resolution manometry (HRM) seems to overcome these shortcomings,
allowing real time detection of lesser degrees of axial separation between the lower esophageal sphincter and crural diaphragm,
distinguishing swallow and distention related artifacts [2,24,25]. Nowadays,
HRM is considered the “gold standard” for HH assessment.
In addition,
the employment of physiopathologic methodologies allow the recognition of esophageal dysmotilities,
which is of capital importance in the eventuality of fundoplicatio to avoid a complete therapeutic failure and postoperative complications [14].
Our results confirm the relationship between CTC technique and small sliding hernias showed by Pickhardt et al.
[1],
as well as the substantial matching between the external control group and the residual prevalence of hiatal hernias after excluding the estimated subset of small sliding HH most likely due to gaseous colonic distention.
It is interesting to note that we obtained similar results considering a group of patients undergoing CT-WE and comparing them with the external control group.
Considering that the increased intra-abdominal pressure from colonic distention induces migration of part of the stomach through the diaphragmatic hiatus [26],
it is likely that most of small sliding hiatal hernias found at CT-WE and CTC will disappear or reduce in size at routine CT exams used as internal control.
In addition,
the lack of a statistically significant difference between CT-WE and CTC results suggests a merely mechanical pathogenesis of HH,
where the water or air-related colonic distention unsettles the intra-abdominal pressure balance,
thus promoting the onset of HH [27]: moreover in some CTC patients,
the direct compression of distended left colonic flexure on the stomach may contribute to the causative mechanism.
On the contrary,
we noticed that most of moderate and especially of large-sized hernias will not disappear in routine CT evaluation (Figure 3),
thus suggesting that small hernias are the main entities to consider as part of the distention-induced pathogenetic mechanism.
However,
our study has several limitations: first of all,
the diagnosis of HH at CT is limited by a certain grade of subjectivity,
especially at CTC,
being the contrast enhanced CT-WE exams more sensitive in identifying the peculiar findings of HH; the prevalence of symptoms of reflux disease in our group of patients was unknown; we evaluated only supine scans in CTC cohort; we use an end-inspiration phase in all our CT acquisition protocols (same phase for CTC,
CT-WE and routine abdominal CT),
possibly leading to an increase of HH prevalence due to augmented intra-abdominal pressure.
Normal 0 14 false false false IT JA X-NONE