ANATOMY: PERITONEAL SPACES
The peritoneum consists of a single layer of mesothelial cells lining the abdominal and pelvic walls (the parietal peritoneum) and covering the external surface of most abdominal organs (the visceral peritoneum).
The peritoneal cavity is the virtual space between these two layers.
The compartmentalization of the peritoneum by its reflections and mesenteries commands the direction and flow of fluid within the abdominopelvic cavity.
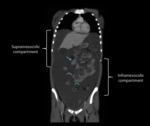
The two main peritoneal compartments - supramesocolic and inframesocolic - are separated by the transverse mesocolon (Fig. 1).
THE SUPRAMESOCOLIC COMPARTMENT
Divided by the falciform ligament into the right and left supramesocolic spaces (Fig. 2).
The right supramesocolic space is further divided into:
- Right subphrenic space: extending over the diaphragmatic surface of the right liver lobe to the right coronary ligament (posteroinferiorly) and the falciform ligament (medially).
- Right subhepatic space: bounded superiorly by the inferior surface of the liver and communicating freely either with the right subphrenic space and the right paracolic gutter.
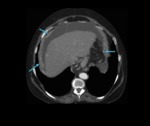
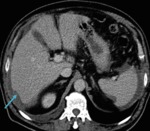
The posterior right subhepatic space (Morrison’s pouch,
Fig. 3) extends posteriorly to the peritoneum overlying the right kidney and is the most dependent portion of the peritoneal cavity in the supine position.
- Lesser sac (Fig. 4): located posterior to the lesser omentum,
stomach,
duodenum and gastrocolic ligament and anterior to the pancreas.
Communicates with the rest of the peritoneal cavity through the epiploic foramen (of Winslow).
The left supramesocolic space is divided into four compartments in communication:
- Left perihepatic space: further divided into the left anterior perihepatic space,
bounded medially by the falciform ligament,
posteriorly by the liver and anteriorly by the diaphragm; and the left posterior perihepatic space,
bounded posteriorly by the lesser omentum,
extending from the surface of the liver into the fissure for the ligamentum venosum.
The left perihepatic space communicates superiorly and to the left with the left subphrenic space and inferiorly with the peritoneal cavity over the surface of the transverse mesocolon.
- Left subphrenic space: divided into the left anterior subphrenic space,
which lies between the stomach and the left hemdiaphragm; and the left posterior subphrenic space, which covers the superior and inferolateral borders of the spleen and is bounded inferiorly by the phrenicocolic ligament and superiorly by the gastrosplenic ligament.
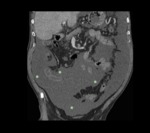
THE INFRAMESOCOLIC COMPARTMENT (Fig. 5)
Divided by the root of the small bowel mesentery into:
- Right inframesocolic space: between the transverse mesocolon superiorly and to the right and the small bowel mesentery inferiorly and to the left.
- Left inframesocolic space: Larger than the contralateral right inframesocolic space,
is in communication with the pelvic cavity to the right of the midline.
The sigmoid mesocolon forms a barrier to the left of the midline.
- Paracolic gutters: peritoneal recesses situated between the posterior abdominal wall and the ascending and descending colon.
The right paracolic gutter is larger than the left and communicates superiorly with the right subhepatic and subphrenic spaces (from the supramesocolic space).
The left paracolic gutter is partially separated from the left subphrenic spaces by the phrenicocolic ligament.
THE PELVIC PERITONEAL SPACES
- The peritoneum reflects inferiorly over the dome of the bladder,
the anterior and posterior surfaces of the uterus and the upper vagina (in females) and the superior portion of the rectum.
The urinary bladder divides the pelvic cavity into the left and right paravesical spaces.
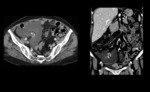
- In women,
there are two potential spaces of fluid accumulation: posteriorly to the bladder (uterovesical pouch) and the rectouterine pouch (of Douglas) (Fig. 6).
- In men,
there is one potential space of fluid collection only,
the rectovesical pouch (Fig. 7).
- The pelvis is the most dependent portion of the peritoneal cavity in the erect position.
ANATOMY: PERITONEAL FLUID CIRCULATION
The normal peritoneal cavity contains a small volume of sterile fluid.
The clearance of this physiologic fluid is potentiated by upward circulation to the subphrenic spaces (where the subphrenic lymphatics provide the majority of the lymphatic clearance from the peritoneal cavity).
This upward movement is driven by fluctuations in the intraabdominal pressure caused by diaphragmatic movement during normal respiration.
While initially the peritoneal fluid collects in the gravity dependent spaces (pelvic peritoneal spaces,
such as the rectouterine and rectovesical pouches),
it then ascends through the paracolic gutters to reach the subphrenic compartments.
The right paracolic gutter is the preferred way up because the phrenicocolic ligament acts as a partial barrier on the left and the falciform ligament prevents passage of fluid from the right to the left subdiaphragmatic compartments.
Fluid is then driven inferiorly to the inframesocolic space,
completing the circuit.
In pathologic conditions (e.g.
ascites),
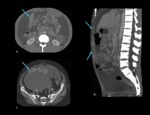
fluid usually is located in well-defined areas of stasis: the pelvic recesses,
the right lower quadrant (the ileocecal junction and the right paracolic gutter),
and the superior aspect of the sigmoid mesocolon.
Thus,
these anatomic landmarks should be thoroughly evaluated when looking for peritoneal carcinomatosis (Fig. 8).
SPECTRUM OF CT FINDINGS IN PERITONEAL CARCINOMATOSIS
Diffuse metastatic seeding of the peritoneal cavity is relatively common with abdominopelvic tumors and neoplastic processes can disseminate through this space with relative ease.
As neoplastic cells freely circulate in peritoneal fluid,
driven by gravity and diaphragmatic pressure gradients,
there are some characteristic locations of intraperitoneal seeding such the dome of the liver; the concave surfaces of the anterior abdominal wall; the omentum; the transverse mesocolon; the small bowel mesentery; and the dependent portions of the pelvis.
On the other hand,
direct invasion to the peritoneum occurs through direct extension of gastrointestinal primary malignancies or tumor extension through the peritoneal ligaments and mesenteries.
Hematogenous spread can also occur from extraabdominal tumors,
such as melanoma,
breast or lung carcinomas.
Lymphatic dissemination is probably a minor route of spread of gastrointestinal tumors to the peritoneal cavity.
CT is almost 90% sensitive in the detection of peritoneal neoplastic lesions greater than 5 mm in diameter,
decreasing significantly for lesions less than 5 mm.
CT manifestations of peritoneal carcinomatosis are protean,
and include:
PERITONEAL THICKENING AND NODULARITY
- Peritoneal thickening and tumor nodules personify typical peritoneal carcinomatosis (Fig. 9).
- May range from infiltrative masses to multifocal discrete nodules that may be missed on CT (Fig. 10).
- Lymphadenopathy may also be a prominent feature (Fig. 11).
ASCITES
- Common finding in peritoneal carcinomatosis.
- Loculation is one of the most helpful features indicating a malignant etiology,
as well as thickening,
nodularity and contrast enhancement of the peritoneal reflections.
OMENTAL “CAKE” (Fig. 12,
Fig. 13)
- Refers the thickened and nodular appearance of the greater omentum, which displaces bowel away from the abdominal wall.
- Most commonly arises from metastatic ovarian,
gastric or colon cancer.
PSEUDOMYXOMA PERITONEI (Fig. 14,
Fig. 15)
- Refers to a clinical syndrome characterized by the presence of thick gelatinous material on the surfaces of the peritoneal cavity.
- Arises from moderately or poorly differentiated mucinous carcinomas of the gastrointestinal tract (mostly from the appendix),
gallbladder,
pancreas or ovary.
- Rare condition,
occurring more commonly in women (mean age at diagnosis – 49 years).
- On CT,
it is described as low attenuation ascites that typically exerts mass effect on adjacent structures with scalloping of solid viscera or displacement of hollow viscera.
- Calcifications may be present.
PERITONEAL IMPLANTS (Fig. 16,
Fig. 17,
Fig. 18)
- Soft tissue masses that can appear as solitary or multiple nodules that can coalesce and form plaques near the surface of the viscera.
- Implants may enhance with intravenous contrast administration.
- Most common locations are the right diaphragmatic surface,
right paracolic gutter,
bowel,
omentum and pelvic cavity.
- Extension of omental disease into the anterior abdominal wall may result in umbilical masses (Sister Mary Joseph nodule - Fig. 19).
- Krukenberg tumor (Fig. 20) is a rare subtype of metastatic tumor to the ovary,
usually arising from signet-ring type gastric cancer.