- AC is an acute inflammatory condition of the gallbladder(1);
- AC accounts 5% of the patients admitted in the emergency room with right upper quadrant pain (1);
- Most of the cases are related with the obstruction of the gallbladder by gallstones or with acalculous cholecystitis (2);
- Clinical presentation: right upper quadrant pain and tenderness(2);
- In the evaluation of the AC the ultrasound (US) is the initial imaging procedure(2);
- Computed Tomography (CT) is done initially if the cause of symptoms is unclear or if ultrasound findings are equivocal(2);
- Acute calculous cholecystitis (ACC)
-The most predictive US findings of the ACC are (2):
a) the presence of a sonographic Murphy´s sign
b) the presence of gallstones
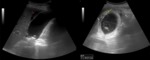
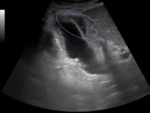
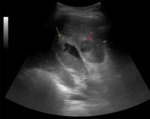
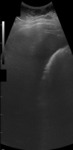
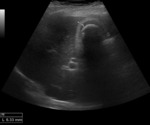
-The secondary US findings of ACC are (2) (Figure 1):
a) gallbladder wall thickening (> 3 mm)
b) distended gallbladder (> 4 cm transverse diameter)
c) pericholecystic fluid
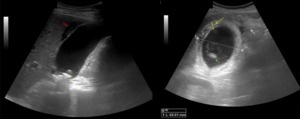
Fig. 1: Ultrasound images showing acute calculous cholecystitis with pericholecystic inflammatory changes: gallbladder distention (69,61 mm transverse diameter), wall thickening (yellow arrow), gallstone (green arrow), echogenic inflamed fat (white arrow) and pocket of oedema fluid (red arrow).
- The gallbladder wall thickening appears in half of the patients with AC,
but it is a nonspecific US finding,
because it can be present in numerous other pathologies.
However,
in the presence of thickening of the gallbladder wall from other causes,
the gallbladder is frequently non-distended (2);
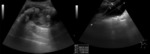
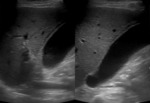
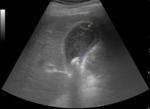
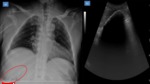
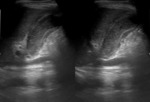
- Adenomyomatosis (Figure 2) and gallbladder cancer (Figure 3) also may result in thickening of the gallbladder wall (2).
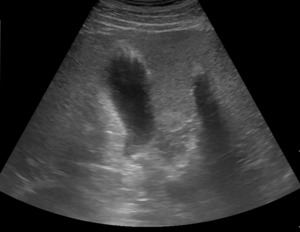
Fig. 2: Ultrasound image showing fundal mural thickening of the gallbladder and echogenic intramural foci from which emanate V-shaped comet tail reverberation artifacts, in adenomyomatosis.
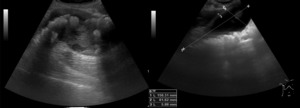
Fig. 3: Ultrasound images showing intraluminal echogenic mass lesion, gallbladder distention (61.62 mm transverse diameter) and diffuse mural thickening wall (5.88 mm), in gallbladder cancer.
-The US finding of pericholecystic fluid is a non-specific finding,
because it can appear with other causes (3).
-There are two types of pericholecystic fluid (3) :
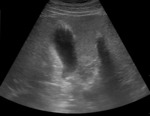
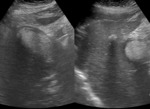
-Type 1 – thin anechoic crescent-shaped collection adjacent to the gallbladder wall,
which is non-specific (Figure 4);
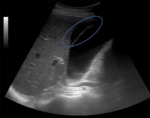
-Type 2 – a round or irregularly shaped collection with thick walls,
septations,
or internal debris,
is more likely to be associated with gallbladder perforation and abscess formation (Figure 5).
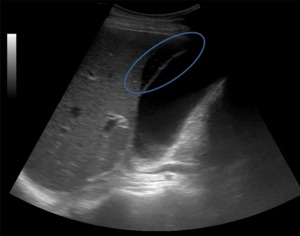
Fig. 4: Ultrasound image showing pericholecystic fluid collection with a thin anechoic crescent-shaped adjacent to the gallbladder wall.
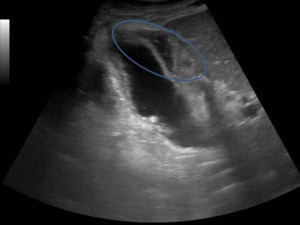
Fig. 5: Ultrasound image showing pericholecystic fluid collection with irregularly shape, thick walls and internal debris.
- ACUTE ACALCULOUS CHOLECYSTITIS (AAC) (Figure 6)
- ACC develops more often in (2):
a) very ill patients,
b) following trauma,
c) surgery,
d) major burns.
- The precise etiology is not totally understood (2);
- The contributing factors for AAC development are(2):
.
ischemia,
. hypotension,
.
sepsis.
-Complications like gangrene or perforation of the gallbladder are more frequent in patients with ACC (4);
-The rate of mortality is higher in patients with AAC (5).
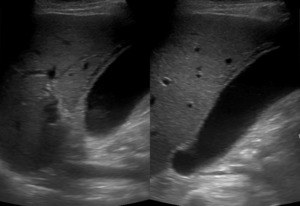
Fig. 6: Ultrasound image showing acute acalculous cholecystitis with pericholecystic inflammatory changes: gallbladder distention, wall thickening, endoluminal echogenic material.
- COMPLICATED ACUTE CHOLECYSTITIS
- Up to 20 % of the patients who have acute cholecystitis can develop complicated acute cholecystitis (2)
-The group of complicated acute cholecystitis include (6):
- empyema,
- gangrenous cholecystitis,
- perforation with pericholecystic abscess or with biliary-enteric fistula,
- emphysematous cholecystitis,
- hemorrhagic cholecystitis.
- Gangrenous Cholecystitis (GC)
-The pathophysiologic explanation for the GC is related with cystic duct obstruction,
that leads to distention of the gallbladder and finally ischemic to necrosis of the wall (7);
-GC is more common in (7):
.
male,
.
elderly patients,
.
patients with coexisting cardiovascular disease.
-There are specific findings on US,
that appear in few minority of patients with GC (7) (Table 1):
- intraluminal membranes (represent desquamated gallbladder mucosa),
- fibrinous strands,
- exudate.
-The sonographic Murphy’s sign may be absent because of denervation of the gallbladder wall (1).
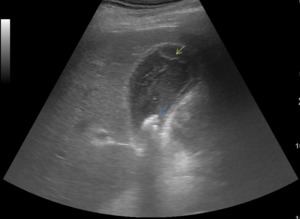
Fig. 7: Gangrenous cholecystitis: sloughed membrane (green arrow) appearing as a linear intraluminal echo, echogenic material within the lumen and gallstones (blue arrow).

Table 1: Correlation between sonographic characteristics and pathophysiology of Gangenous cholecystitis (1).
- Hemorrhagic Cholecystitis (HC)
-HC is a rare complication of acute cholecystitis(8);
-HC appears in the presence or in the absence of gallstones (8);
-The hemorrhage appears in result of the inflammation,
causing mucosal ulceration and necrosis(7);
-Arteriosclerotic change in the gallbladder wall is a predisposing factor (4);
-US findings of HC are (7):
- echogenic material within the lumen (blood in the gallbladder),
more echogenicity than sludge.
- blood clots appear as clumps or masses adherent to the gallbladder wall and as the hemorrhage evolves,
this condition may have a cystic appearance.
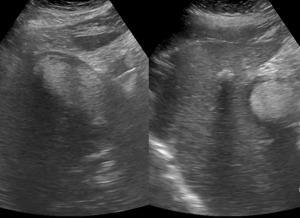
Fig. 8: Hemorrhagic Cholecystitis (HC) – Ultrasound image showing presence of a distended gallbladder, with diffuse wall thickening and filled with echogenic material with a higher echogenicity than sludge representing hemorrhage.
-Perforation occurs in 5% to 10% of patients who have acute cholecystitis,
more often in association with gangrenous cholecystitis (2);
-Gallbladder perforation can be classified into three types (9):
Type 1 - Acute free perforation into the peritoneal cavity which will result in peritonitis,
it is less common but has the higher mortality rate (40 %);
Type 2 - Subacute perforation with a pericholecystic abscess,
it is the more common,
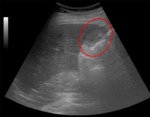
being the fundus the most frequent site of perforation because it has the least blood supply (Figure 9);
Type 3 - Chronic perforation with a cholecysto-enteric fistula,
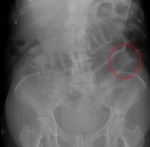
about one-third of these patients will develop biliary ileus (Figure 10).
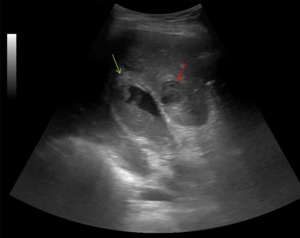
Fig. 9: Ultrasound image showing subacute perforation in the fundus (green arrow), with a pericholecystic abscess (red arrow).
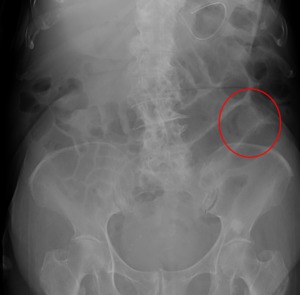
Fig. 10: Abdominal radiogram showing dilatated bowel loops, in relation with intestinal obstruction caused by biliary ileus (red wheel).
-Patients with intraperitoneal abscesses require immediate surgery.
Liver abscesses can be treated effectively with percutaneous drainage,
and abscesses in the gallbladder wall or gallbladder fossa (Figure 11) may respond to conservative treatment (10).
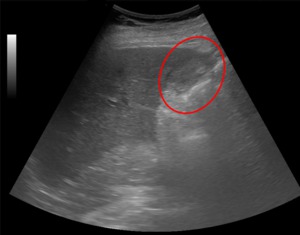
Fig. 11: Ultrasound image showing abscess in the gallbladder fossa (red wheel).
- Emphysematous cholecystitis (EC)
-EC accounts for less than 1% of complicated cases of acute cholecystitis(2);
-EC is caused by gas-forming bacteria in the gallbladder lumen or in the gallbladder wall (2);
-The vascular compromise of the cystic artery is believed to play a role in the pathophysiology of the EC (7);
-There are differences between emphysematous cholecystitis and acute cholecystitis,
which suggest distinct pathogenesis namely:
- EC has male dominance (7;11);
- EC is frequent in diabetic patients (7;11);
- In EC the absence of gallstones is observed in up to one third of patients (7;11);
- EC has an higher risk of gallbladder gangrene (75%) and perforation (20%) (2).
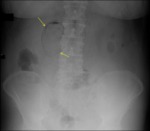
- The abdominal radiographs are used to make the diagnosis of EC and the classic three stages are (7) (Figure 12):
Stage 1 - includes gas in the gallbladder lumen;
Stage 2 - includes gas in the gallbladder wall;
Stage 3 - includes gas in the pericholecystic tissues
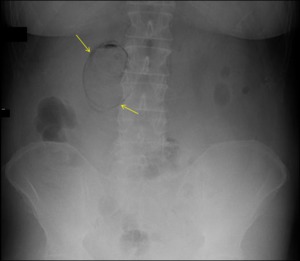
Fig. 12: Abdominal radiogram showing a radiolucency bordering the bile fossa and inside the gallbladder lumen (yellow arrows).
-CT and ultrasound are more sensitive for the detection of small amounts of gas (2);
-The extremely echogenic gas at the nondependent portions of the gallbladder lumen which encloses a distal shadow - “dirty” shadow (not accurately differentiate between calcium and air),
is the US finding that characterizes the EC (2) (Figure 13) (Table 2);
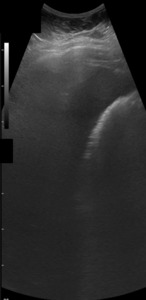
Fig. 13: Ultrasound image showing absence of a normal gallbladder with highly echogenic reflectors, low-level posterior shadowing and reverberation artifact , around/inside the gallbladder ("dirty" shadowing).

Table 2: Correlation between sonographic (1) and plain film (4) characteristics of the emphysematous cholecystitis.
- On US intramural gas is more difficult to identify,
because it may mimic the mural calcification seen in a porcelain gallbladder (2);
- When US findings are equivocal,
CT should be performed (7);
- CT should be performed in patients with suspected acute cholecystitis in whom the gallbladder cannot be fully visualized (7).
- CHRONIC CHOLECYSTITIS (CC)
- CC is a chronic inflammation of the gallbladder wall in the presence of gallstones with fibrosis of the wall,
which disrupts normal motility and result in a contracted appearance (12) (Figure 14);
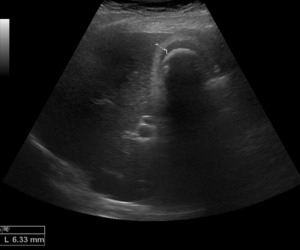
Fig. 14: Ultrasound image showing chronic inflammation of the gallbladder wall (6,33 mm), due to fibrosis, presence of gallstone, which produce a posterior acoustic shadowing with fibrosis of the wall (WES complex).
- At US CC can produce the wall-echo-shadow (WES) and the two echoes are distinguishable by the presence of a thin crescent of anechoic bile in the residual gallbladder lumen (12).
- Porcelain Gallbladder (PG)
-PG is characterized by calcification of the gallbladder wall (13);
-PG is a rare condition (13);
-PG is more frequent in the 6th decade (13);
-PG has greater incidence in women (13);
-On abdominal plain films PG presents as rim-like calcification,
but CT is more sensitive (14);
-On ultrasound PG can be categorized in three patterns (14):
Type I - Hyperechoic semilunar structure with complete posterior acoustic shadowing,
this type should be differentiated from ecogenic content of the gallbladder such as milk of calcium,
gallbladder with stones or collapsed gallbladder with large stones (Figure 15);
Type II - Biconvex curvilinear echogenic structure with less posterior shadowing than type I,
sometimes emphysematous cholecystitis can simulate this pattern;
Type III presents as an irregular aggregate of echoes with less posterior acoustic shadowing than type I.
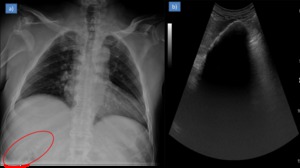
Fig. 15: Abdominal radiogram showing (a)) partial layer of mineralisation outlining the gallbladder wall. Ultrasound image showing (b)) an hyperechoic semilunar structure with complete posterior acoustic shadowing.
-PG is a pre-cancerous lesion,
however controversy has been raised about the association with gallbladder carcinoma,
and therefore,
over the need for prophylactic cholecystectomy (15).
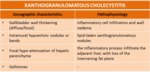
- Xanthogranulomatous Cholecystitis (XGC)
-XGC is a rare form or chronic gallbladder infection (16);
-XGC is characterized by intramural infiltrate of foamy histiocytes and lipid-laden xanthoma cells (16);
-XGC has greater incidence in female gender (16);
-XGC is more frequent at 6th-7th decade (16);
-XGC is highly related with gallbladder stones (80-90%) (16);
-Clinically it presents with cholecystitis or obstructive jaundice (16);
-The US findings that characterize the XCG are (16) (Figure 16) (Table 3):
- hypoechoic nodules or bands in a thickened gallbladder,
- calculi in a patient with chronic disease.
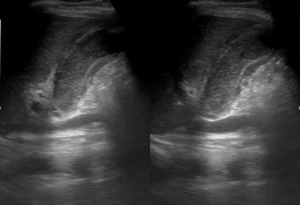
Fig. 16: Ultrasound images showing diffuse gallbladder wall thickening, with intramural hypoechoic bands associated with pericholecystic inflammatory changes.
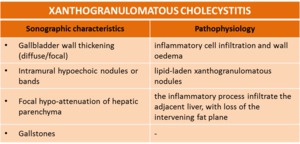
Table 3: Correlation between sonographic characteristics and pathophysiology of the xanthogranulomatous cholecystitis (1).
-The band or nodules histopathologically correspond to macrophages and inflammatory cells or necrosis and/or abscess (17);
-XCG treatment is cholecystectomy,
for two reasons (18):
this condition may have an association with gallbladder carcinoma;
the overlap in imaging features of XCG and gallbladder carcinoma makes preoperative distinction between them almost impossible.