Clinically,
IVL presents as fever of unknown origin or intermittent fevers.
Skin rash may be seen mainly in the abdomen and thighs in 50% of the cases.
When CNS involvement appears it manifests as subacute encephalopathy ranging from disorientation to focal signs such as hemiparesis and myelopathy,
dementia (most common form of presentation),
seizure,
multifocal cerebrovascular events or memory loss.
Among the procedures used for diagnosis are CSF analysis which may show mild leukocytosis or an increased amount of protein,
but cytologic results are negative.
On laboratory examination,
results are nonspecific such as,
anemia,
increased CRP and LDH levels; elevated erythrocyte sedimentation rate.
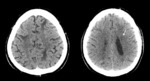
Unhenhanced CT findings are frequently normal or inespecific,
such as: focal lesions,
bilateral and asimetrical hipodensity in the cortex o basal ganglia.
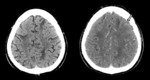
Fig. 1 While enhanced CT may show increased vascular attenuation or enhanced wall vessels or perivascular space,
because of proliferation of tumor cells.
Fig. 2
On the other hand,
MR imaging is the best imaging technique for diagnosis.
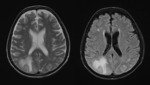
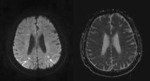
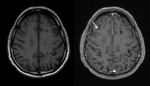
Findings have been categorized in five patterns: infarctlike lesions,
nonspecific white matter lesions,
meningeal enhacement,
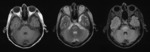
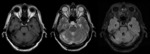
masslike lesions and hyperintense lesions in the pons on T2WI.
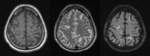
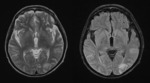
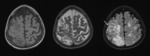
Infarctlike lesions suggest that the tumor predominantly involves small arteries.
MR imaging shows severe vascular occlusions by tumor cells and multiple infarctions.
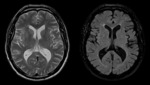
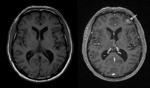
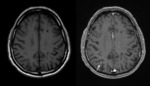
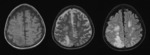
Fig. 3 High intensity in the basal ganglia and thalamus on T2-weighted images suggest minimal lacunar infarcts. Fig. 4
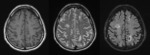
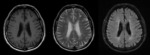
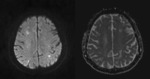
Nonspecific white matter lesions have been reported specially in the periventricular area and with patchy morphology.
Fig. 5 Fig. 6 This pattern is caused by congestion and chronic isquemic change due to severe vascular infiltration by tumor cells.
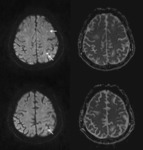
Usually the tumor cells are noncohesive and free in the lumen with slow flow in the capillaries secondary.
Fig. 7 Fig. 8 These lesions may show diffusion restriction and hemorrhagic transformation. Fig. 9 Fig. 10 Fig. 11
Contrast enhacement varies from no enhacement to variable parenchymal enhacement,
including either linear and punctuate,
patchy,
irregular,
nodular,
cortical or periventricular enhacement. Fig. 12 Fig. 13 Fig. 14
Meningeal enhacement is sometimes present in patiens with IVL.
A contrast enhanced T1-weighted image can show dural-aracnoid enhacement.
Autopsies show severe inflammatory reaction with tumor cells. Fig. 15
Masslike lesions present with extensive vasogenic edema and mass effect.
These finding possibly predict extraluminal spread of the disease. Fig. 16
Hyperintense lesions in the pons on T2WI can be observed without enhacement or diffusion restriction.
These lesions are usually similar to the findings in pontine osmolytic demyelination syndrome and PRES in the brain stem or intracranial dural arteriovenous fistula with venous congestion. Fig. 17 Fig. 18
MR imaging might show development of new lesions or progressions of existing lesions,
fluctuation in size or number of the lesions in a relatively short period during corticosteroid therapy or reduction of the lesion size after chemotherapy.
Other imaging techniques are cerebral angiography that reveals findings consistent with those of CNS vasculitis.
Also,
nuclear medicine,
such as,
PET may be used.
The differential diagnosis should be made between:
- Vasculitis: shows mutifocal areas of subcortical ischemia with enhacement that might mimic IVL.
- Primary lymphoma of CNS: demonstrate lesions located in the basal ganglia,
periventricular white matter and corpus callosum.
The ependymal affectation is caractheristic.
- Neurocisticercosis: meningeal enhacement might be observed.
The cerebral parenchyma is typically preserved.
Clinically,
the patients manifest systemic disease.