Introduction
Tuberculosis (TB) was known lethal disease prior to the development of the antibiotics before 1950s,
which thereafter showed a steady fall in incidence.
However,
Tuberculosis is still remained endemic in developing countries wherein poverty,
malnutrition and the presence of drug resistant strains aid in spread of the disease.
In addition there is resurgence of the disease since mid-1980s in developed countries,
mainly in immigrants from countries where the disease is prevalent and in patients with immunodeficiency diseases or chronic diseases like DM,
chronic renal failure,
COPD,
cirrhosis of the liver,
leukemia,
and lymphoma.
The other factors contribute to this resurgence of the disease are growing elderly population,
poor living conditions,
poor nutrition status,
alcohol and drug abuse.
*TB involves both pulmonary and extrapulmonary sites.
*The incidence of the skeletal tuberculosis is 1-5% of the patients with
tuberculosis.
*In developing countries the skeletal tuberculosis is most common in
children whereas in industrialized countries adults are commonly affected.
*There is no predilection for either sex.
Koch’s spine or spinal tuberculosis is the most important skeletal presentation of the disease.
Percival Pott presented the classic description of spinal tuberculosis (TB) in 1779.
Hence,
spinal TB was called 'Pott's Disease'.
*It constitutes about 50% of the musculoskeletal tuberculosis.
*In developing countries the presentation is common in children and young
adults and is more aggressive in extension and abscess formation.
*Consequently the neurological complications and deformities are frequent.
The varied presentation,
serious complications and association of the spinal tuberculosis with immunodeficiency and chronic health diseases warrants its inclusion in the differential diagnosis in spinal disorders.
MR imaging is currently the modality of choice for the evaluation of potential spinal infections and spinal disorders.
*The advantages of MR imaging over other modalities include capability of
multiplanar imaging,
direct evaluation of the bone marrow and
simultaneous visualization of the neural structures.
Pathology and pathogenesis
- Tuberculosis is caused by a bacillus,
Mycobacterium tuberculosis.
- Spinal tuberculosis is usually secondary to the primary or reactivated infective focus either from the lung or genitourinary system.
- Spread of the infection to the spine is through hematogenous in most of the instances.
- Other types of spread are from paraspinal infection and lymphatic spread from adjacent structures like pleura or kidney.
- Tuberculosis infection is characterized by a delayed hypersensitivity immune reaction.
- In the vertebrae the granulomatous lesion develops containing central caseating necrosis,
multinucleated giant cells,
epitheloid cells and peripheral lymphocytes.
- The inflammatory reaction with formation of granulation tissue causes bone expansion and trabecular destruction,
progressive demineralization,
bone destruction and in later stages cartilage destruction with involvement of adjacent disc space.
- The osseous lytic lesions with distinct margins show no bone regeneration or periosteal reaction,
which eventually undergoes fibrosis,
sclerosis and ankylosis in chronic stages.
- The proliferative granulation tissue causes thrombosis of the vessels,
tissue necrosis and breakdown of the inflammatory cells results in paraspinal abscess.
- The pus may localize or track along the tissue planes.
Progressive necrosis of the bone leads to kyphosis.
- Typically the infection begins in the anterior aspect of the vertebral body adjacent to the disk.
The infection then spreads to the adjacent vertebral bodies under anterior longitudinal ligament.
- Noncontiguous (skip) lesions are also seen.
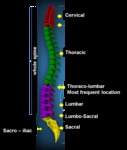
Site of infection:
Most frequent site of involvement of spinal tuberculosis is the thoracolumbar junction (fig 1).
The frequency of incidence of the infection is low above and below this level.
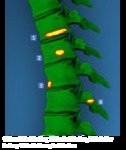
Pattern of spine involvement (figure 2)
Ø Typical presentation-
Involvement of contiguous vertebrae with extension into the
intervertebral disk.
Ø Atypical presentation-
· Involvement of noncontiguous vertebrae with no evidence of involvement
of intervertebral disk.
· Isolated involvement of the posterior spinal elements.
Pattern of vertebrae involvement (fig 3)
The primary focus can be in the vertebral body or in the posterior elements.
In the vertebral body three patterns of involvement is recognized.
- Paradiskal
- Anterior
- Central.
Paradiskal lesions
- This is the most common pattern of spinal tuberculosis.
- The lesion is adjacent to the intervertebral disk (fig 3) leading to narrowing of the disk space.
- The narrowing of the disk space is either due to destruction of the subchondral bone with herniation of the disk into the vertebral body or direct involvement of the disk.
Anterior lesion
- This is a subperiosteal lesion under anterior longitudinal ligament (fig 3).
- The infection/pus spreads over multiple vertebral segments resulting in stripping of the periosteum and anterior longitudinal ligament from the anterior surface of the vertebrae.
- The stripping of the periosteum renders the vertebrae avascular and susceptible to infection.
The ischemia and pressure causes anterior scalloping of the vertebrae.
Central lesion:(fig 3)
- This lesion is centered in the vertebral body .
- There is vertebral collapse leading to formation of vertebra-plana appearance.
- There is no involvement of the disk.
Posterior spinal elements lesion:(fig 2,
3)
- This is infrequent presentation.
- The lesion is seen in pedicle,laminae,
spinous process or articular processes.
- There is erosion or abscess formation.
Skip lesions (Fig 2,3)
- Noncontiguous vertebral body involvement without involvement of intervening disk.
- This is a rare presentation.
Complications of TB spine (Fig 4):
- The most serious complications include paraplegia or quadruplegia which are seen in 10% of the patients.
- Cord compression is another complication due to either epidural abscess or granulation tissue or in combination with vertebral collapse,
subluxation,
or dislocation.
- Rarely results in meningomyelitis due to penetration of pus into dura.