This poster is published under an
open license. Please read the
disclaimer for further details.
Type:
Educational Exhibit
Keywords:
Metastases, Cancer, Diagnostic procedure, Complications, Fluoroscopy, CT, Liver, Biliary Tract / Gallbladder, Abdomen
Authors:
A. J. Wigham, N. davies, F. P. Y. Lam, S. Vyas, C. Imber, M. Malago, L. A. Grant; London/UK
DOI:
10.1594/ecr2015/C-1130
Findings and procedure details
ALPPS involves a two-stage hepatectomy.
The first stage involves right portal vein ligation (with preservation of the hepatic artery) and in situ splitting of the liver.
This results in rapid hypertrophy4.
The second stage is usually performed after 10 days,
and it involves interruption of the hepatic artery,
hepatic veins and biliary drainage in a manner similar to a conventional right hepatectomy.
Cross sectional imaging is usually performed one week after the first stage.
The purpose of this is to measure the degree of hypertrophy and to assess any complications.
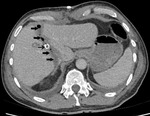
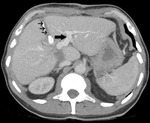
The ligated portal vein should be identified and the contralateral portal vein and main portal vein should be assessed for patency (Figures 1 and 2).
The hepatic artery supply to both lobes should be accurately detailed to ensure there is no vascular injury.
Major complications of ALPPS include bile leak and vascular injury.
Timely diagnosis of bile leak and drainage is important to prevent the development of biliary sepsis,
which may delay the performance of the second stage and is associated with increased mortality5.
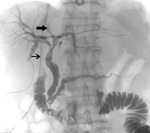
Figure 3 demonstrates a case of bile leak after the first stage of ALPPS.
The patient was planned for ALPPS and a right hepatectomy for colorectal cancer metastases.
Following the first stage,
a bile leak was suspected due to the nature of the drain content.
A T- tube cholangiogram was performed,
which demonstrated a leak from the right anterior duct (nNote the aberrant insertion of the RAD into the LHD).
A subsequent CT was performed,
which showed the surgical drain to be in good position and there was no drainable collection.
The patient proceeded to the second stage right hepatectomy without delay or further complication.
Vascular complications affecting the planned liver remnant can have serious consequences.
Contralateral PV thrombosis is a rare but serious complication.
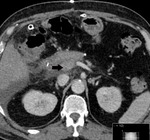
Figure 4 demonstrates main and left portal vein thrombosis following first stage of ALPPS,
in a patient who was planned for a right hepatectomy for pancreatic cancer metastases.
This case was complex and patient developed pancreatitis,
which was thought to be the main aetiological factor in the development of portal vein thrombosis rather than due to the ALPPS procedure per se.