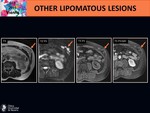
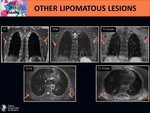
The radiological differentiation between lipoma and WDL seems to be clear.
The problem lies in distinguishing this tumor with different variants of lipomas,
as they can exhibit analogous radiological and histological features.
[2]
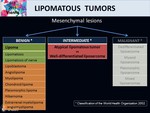
There is a wide range of histological subtypes and we classified this lesions as: Fig. 4
- Benign tumors: lipomas,
lipomatosis and its variants (angiolipoma,
myolipoma,
chondroid lipoma,
hibernoma...).
- Intermediate tumors: WDL or atypical lipomas.
Benign lipomatous tumors
Lipomas
More frequently affect patients between fifty to seventy years.
They usually are located superficially (more commonly in the subcutaneous tissue) or deeply (in the upper back and neck,
shoulder,
abdomen and proximal portions of the extremities).
Microscopically they are composed of mature fat or adipocytes,
similar to the surrounding fat.
And they are well vascularized,
however,
this feature may not be apparent due to vascular compression of the distended adipocytes.
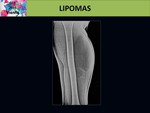
The radiograph may occasionally demonstrate a radiolucent soft tissue mass and rarely osseous deformity by mass effect. Fig. 5
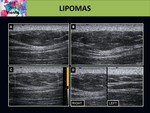
The most frequent sonographic appearance of lipoma is an elliptical,
compressible and well-defined mass parallel to the skin surface.
They usually are hyperechoic in comparison with adjacent muscle,
although they can also be isoechoic or hypoechoic. Fig. 6
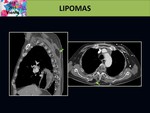
On CT they appear as homogeneous,
well-circumscribed and encapsulated masses of fatty nature,
without enhancement after intravenous contrast administration.
Sometimes regular and thin septations can be identify. Fig. 7
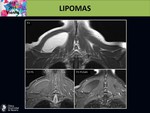
On MRI:
- Lipomas often measure less than 5 cm,
rarely exceeding 10 cm.
- They are homogeneous,
well circumscribed and encapsulated lesions which are isointense to subcutaneous fat on all sequences with complete suppression on fat-saturation techniques.
- After contrast material,
they do not show any enhancement. Fig. 8
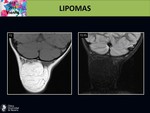
- Sometimes,
regular thin septa can be seen as low-intensity on T1 images with a slight enhancement after contrast material.
[1,
2] Fig. 9 Fig. 10
Lipomatosis
Lipomatosis is characterized by diffuse growth of mature adipose tissue in an infiltrating pattern,
leading to deformities and limb asymmetries.
It usually affects large areas of an extremity or the trunk.
Microscopically,
accumulated fat is indistinguishable from mature fat,
except for varying degrees of fibrosis and,
rarely calcification and ossification.
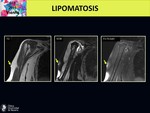
On MRI the disease shows the characteristics of lipomas apart from the fatty depositions being poorly circumscribed and non-encapsulated that affects both the subcutaneous and deep soft tissues.
[2,
3] Fig. 11
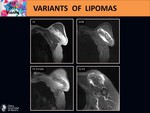
Lipomas' s variants
Like lipomas,
these lesions are typical of people between 60 to 70 years and they appear superficially or deeply.
They are similar to lipomas but with presence of non-fatty elements that classify them in a wide range of subtypes.
This elements could be cartilage,
bony elements,
vessels,
brown fat,
muscle,
necrosis,
fibrosis or mucoid. Fig. 12
According to the nature of the non-fatty component,
different entities are distinguished: lipomatosis of nerve,
lipoblastoma/lipoblastomatosis,
angiolipoma,
myolipoma of soft tissue,
chondroid lipoma,
spindle cell/pleiomorphic lipoma,
and hibernoma.
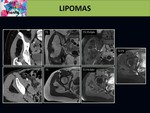
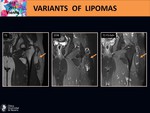
On MRI we can observe a well defined and heterogeneous soft tissue mass,
with fatty and non-fatty components.
Depending on the nature of this non-fatty component its behavior on MRI will differ.
After contrast material,
the non-fatty areas show poor and slow contrast enhancement.
Fig. 13 Fig. 14 Fig. 15 Fig. 16
Lipomas containing other mesenchymal elements,
in parentheses,
are classified as:
- Fibrolipoma (fibrous connective tissue).
This is the non-fatty component more common.
On MRI it is seen as low signal intensity (SI) on T1 and T2 weighted images (WI). Fig. 13
- Myxolipoma (mucoid or mixoid degeneration) with low SI on T1-WI and high signal on T2-WI.
- Chondroid lipoma (myxoid and chondroid material).
It is a well-defined mass with prominent fluid-like areas shown like low SI on T1-WI and hyperintense on T2-WI demonstrating the mixoid component and fine septations with lobulated margin suggesting cartilage matrix.
Calcification is usually present (the differential diagnosis with malignant lesions include synovial sarcoma,
malignant peripheral nerve sheath tumor,
epithelioid hemangioendothelioma...and with benign lesions include myositis ossificans).
This type of lipoma variants are difficult to distinguish from myxoid liposarcoma,
extraskeletal myxoid chondrosarcoma,
and ancient schwannoma so biopsy is required to make a final diagnosis.
- Osteolipoma (bony elements),
radiography and CT scan are useful diagnostic tools to demonstrate the ossified components,
whereas MR allows further identification of the adipose ones.
- Myolipoma (smooth muscle).
Imaging does not allow distinction from a well-differentiated liposarcoma.
Coarse calcification may be seen.
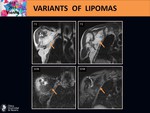
- Angiolipoma (small and thin-walled vessels).
On MR,
they show a mixed composition of both fatty and vascular elements.
The non fatty areas exhibit low SI on T1-weighted images,
high SI on T2-weighted images and enhance markedly after intravenous injection of gadolinium). Fig. 14
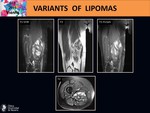
- Intramuscular lipoma may present with irregular margins,
interdigitating with skeletal muscle and with traversing muscle fibers typically causing a striated appearance which is not seen with other lipomas.
On MRI we can identify muscle fibers running through the lesion without other evidence of thick septa or nodules.
Fig. 15 Fig. 16
- Hibernoma (brown fat).
It is generally well-circumscribed,
encapsulated tumor with a lobular pattern,
connective tissue septa and highly vascularization.
Infiltration of the surrounding tissues may occur.
On MRI we observe a heterogeneous or septated mass,
isointense or slightly hypointense to subcutaneous fat on T1-WI,
but frequently hyperintense to normal muscle tissue.
On T2-WI the mass can be nearly isointense to subcutaneous fat,
although hypo or hiperintensity areas can also be observed.
It usually demonstrates inhomogeneous or absence of enhancement after intravenous contrast administration.
The non-fatty components can alter MRI appearance of a simple lipoma,
making the differential diagnosis with well-differentiated liposarcoma sometimes complicated.
Treatment for lipomas and its variants is enough with a marginal excision.
[1,
2]
Other benign lesions we should differentiate from well-differentiated liposarcomas
- Hemangiomas: are benign vascular lesions composed of vascular structures,
fat,
smooth muscle,
hemosiderin and phleboliths.
On MRI they are lobed and isointense to muscle lesions.
We can also identify hyperintense foci on T1-WI (due to fat component or bleeding areas) and hyperintense foci on T2-WI (due to vascular component).
After contrast medium a uniform and intense enhancement is observed.
[4] Fig. 17
- Elastofibroma dorsi: is a benign unencapsulated lesion consisting of fibrous,
elastic and fat tissue.
The most frequent location is the subscapular region.
It can be bilateral (10-66 %).
On MRI we observe a well-defined and inhomogeneous lesion,
with a signal intensity similar to the muscle and with linear fatty areas within the lesion.
After contrast administration there is no abnormal uptake,
but you can see areas with mild enhancement.
[5] Fig. 18
Intermediate lipomatous tumors
Well-differentiated liposarcomas (WDL)
They are the most frequent subtype of liposarcoma,
representing nearly 50 %.
The average age is about 60 years and the most frequent location is the lower limb (especially the thigh),
followed by the retroperitoneum (which is very specific),
paratesticular area,
mediastinum and subcutaneous tissue.
Fig. 19
They are locally aggressive,
with no potential for metastasis although they can degenerate to high-grade sarcomas.
This is the reason why they are known as liposarcomas.
And this means that a wide excision should be done as treatment.
[2,6]
They can recurrence if only marginally excised.
Recurrence may occur after a long delay (5–10 years) following the initial excision.
Retroperitoneal tend to have a higher recurrence rate.
Fig. 20
According to the diagnostic gold standard,
namely,
histopathology combined with cytogenetic and molecular genetic analysis,
medical imaging remains very sensitive for the diagnosis of liposarcoma.
Histologycally we can observe mature adipocytes with atypical focal nuclear hyperchromatic lipoblast or stromal cells.
However,
the diagnosis is sometimes difficult because the atypical stromal cells can be infrequent and scattered throughout the lesion.
Other tools have been described to distinguish these tumors: immunohistochemistry,
reverse transcription polymerase chain reaction,
fluorescence in situ hybridization and antibodies to MDM2 and CDK4.
Genetic abnormalities,
especially MDM2 and CDK4 gene overexpression related to amplification of the 12q13–15 chromosomal region and ring or giantmarker chromosomes,
have been observed in WDL.
[2,
7]
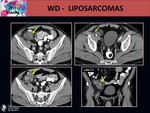
On CT we observe a well-marginated mass,
with attenuation values equal to those of simple fat,
mimicking a benign lipomatous tumor.
However,
this type usually has some thickened (more than 2 mm wide) linear or nodular soft tissue septa,
which enhance after intravenous administration of contrast material.
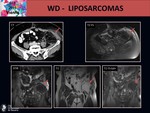
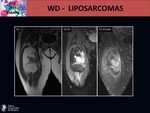
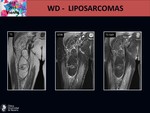
On MRI we can identify:
- A big and heterogeneous lesion with more than 75 % of fatty component.
- Non adipose areas or nodules which enhance after contrast agent.
- Prominent foci of high signal on T2 sequences.
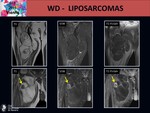
- Thick irregular septa that enhance after contrast agent. Fig. 21 Fig. 22 Fig. 23
However it is important to keep in mind that nodular non lipomatous components larger than 2 to 3 cm or a non lipomatous component that appears in a previously known WD-liposarcoma,
suggest a high-grade sarcoma.
[1,
2,
6,
8] Fig. 23
A summary of the main differences between lipomas,
its variants and well-differentiated liposarcomas are recorded in figure 24. Fig. 24
However,
despite these characteristics,
a lesion consider suggestive of well-differentiated liposarcoma,
is more likely (with sixty-fourth percent) to represent one of many benign lipoma’s variants,
containing non-fatty elements.
And this is due to the high prevalence of benign lesions.
So it is worth to suggest malignancy,
because a thirty-six percent of these patients will have a real WD-liposarcoma.
[8]