Renal vein Thrombosis
The renal vein may also contain thrombus after invasion by renal cell cancer.
Other less common causes include,
renal transplantation,
Behcet Syndrome,
Hypercoagulable states,
and antiphospholipid antibody syndrome
Hypercoagulability is the underlying process involved in both arterial and venous renal thrombosis.
Causes of renal vein thrombosis
1. Antithrombin III deficiency
2. Protein C or S deficiency
3. Antiphospholipid antibody syndrome
4. Pregnancy or estrogen therapy
5. Renal vein invasion by malignant cells
6. Post renal transplantation
7. Behçet syndrome
8. Extrinsic compression ( lymph nodes,
tumor,
retroperitoneal fibrosis,
aortic aneurysm)
9. Nephrotic syndrome
In children,
dehydration and sepsis are the factors leading to renal vein thrombosis.
Other causes include polycythaemia,
maternal diabetes,
indwelling venous catheters,
nephrotic syndrome
On ultrasound examination the ipsilateral kidney is enlarged,
initially.
Doppler examination shows reversal arterial flow,
absent venous flow,
direct visualisation of the thrombus within the lumen of the vein. Contrast enhanced CT reveals a filing defect in the vein with parenchymal changes in the involved kidney.
MRI may be useful in patients with renal impairment
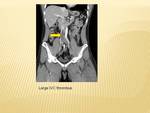
Ovarian vein thrombosis is a rare cause of abdominal pain and can mimic a surgical abdomen.
It usually occurs in the post partum period,
can also occur in patients with pelvic inflammatory disease,
recent abdominal surgery,
malignancy and in patients with known hypercoagulable state.
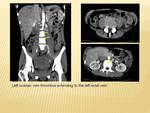
In our patient,
the left ovarian thrombus occurred five days after a miscarriage
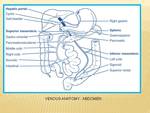
The portal vein is formed by the confluence of the splenic and superior mesenteric veins.
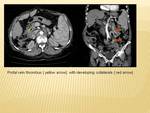
Thrombosis of the portal vein occurs in patients with cirrhosis,
procoagulant state,
intra-abdominal infections,
hepatic malignancies,
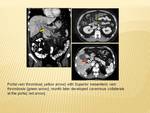
pancreatitis; the thrombus may spread from the splenic vein and extend into the portal vein.
The thrombus can spread into the superior mesenteric vein and lead to bowel ischaemia. If left untreated or delay in diagnosis,
cavernous transformation of the collaterals occurs.
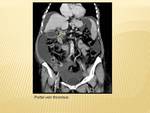
Ultrasound and contrast enhanced CT are usually diagnostic.
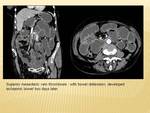
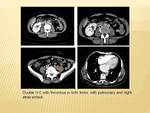
Acute thrombosis of the superior mesenteric vein { Fig 4}occurs in 5-15 % of all acute mesenteric ischaemia,
20-40% cases are idiopathic,
hypercoagulable states account for the rest.
Symptoms of SMV thrombosis are usually non-specific and CT imaging is necessary for diagnosis,
and estimated to be 100% sensitive. Primary findings include filling defect within the SMV with secondary changes of bowel ischaemia.