Posterior reversible encephalopathy syndrome (PRES) [1,
2] is a clinicoradiological entity that was well described by Hinchey et al.
This condition has been designated by a variety of names (reversible posterior leukoencephalopathy syndrome,
reversible posterior cerebral edema syndrome,
and reversible occipital syndrome,
reversible posterior cerebral edema syndrome,
and reversible occipital parietal encephalopathy).
PRES is now the accepted term [1,
2,
3] but has been challenged recently based on the risk of neurological impairment and up to 15 % mortality rate [7,
8].
Diagnosis
PRES is a clinicoradiological entity.
The intensity and severity of clinical manifestations vary and may require ICU admission.
Imaging findings also vary in severity. Thorough familiarity with the imaging criteria is crucial to the diagnosis.
The combination of suggestive clinical manifestations and radiological criteria establishes the diagnosis of PRES.
In doubtful cases,
the clinical and radiological improvement that occurs once appropriate treatment is given confirms the diagnosis.
Nevertheless, there are no consensual guidelines to validate diagnosis of PRES.
Clinical Manifestations of PRES
PRES is characterized by variable associations of seizure activity,
consciousness impairment,
headaches,
visual abnormalities,
nausea,
vomiting,
and focal neurological signs.
Acute hypertension is not usually described among the main signs of PRES.
However, hypertension has been reported in most studies [3–5,
7,
8,
11,
12],
in 67 % [11] to 80 % [3] of patients.
Radiological Characteristics of PRES
CT findings are often normal or nonspecific [11].
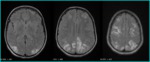
Hypodensities in a suggestive topographic distribution suggest PRES (predominantly in parieto occipital white matter (Fig 1).
MRI: Cerebral MRI is the key investigation for the diagnosis of PRES.
Proton-density and T2-weighted images show regions of high signal indicating edema.
Fluid-attenuated inversion recovery (FLAIR) sequences also visualize the lesions.
The use of FLAIR has been shown to improve the diagnosis of PRES and the detection of subcortical and cortical lesions in PRES [6]. T1-weighted images show low-intensity foci.
Diffusion-weighted imaging (DWI) is normal but the apparent diffusion coefficient is increased [13]. Finally,
enhancement is seen in about half the cases [11].
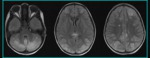
The cerebral imaging abnormalities are often symmetric and predominate in the posterior white matter .
Imaging typically shows areas of bilateral hemispheric edema affecting parietal and occipital lobes,
followed by frontal lobes,
inferior temporal occipital junctions and cerebellum (Fig.
2,
3).
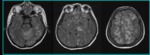
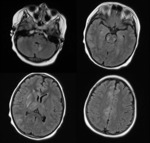
Unusual Locations
- Involvement basal ganglia,
brainstem,
and deep white matter (( external / internal capsule,
corona radiata,
splenium of corpus callosum) are a less common but recognized part of PRES particularly when associated with abnormalities in the typical location (Fig.
4,
5,
6).
- Isolated unusual location in PRES,
e.g central PRES with only basal ganglia and brainstem involvement,
is rare but well known to occur.
- Medulla oblongata and spinal cord at least 4 cases described,
all are associated with hypertension(Fig.
7).
- PRES may occasionally present with minimal or no detectable parietooccipital edema.
In such cases,
it is necessary to exclude other causes,
such as myelinolysis or encephalomyelitis using clinical history and follow-up imaging,
when necessary.
Atypical manifestations of PRES
- Enhancement (up to 37%) : cortical,
leptomeningeal,
parenchymal or pachymeningea (Fig.
8,
9).
- Restricted diffusion (11-26%) (Fig.
10).
- Hemorrhage (10.5-17.1%) : parenchymal or subarachnoid(Fig.
11,
12).
- Unilateral hemispheric involvement (2.6%) (Fig.
13).
- Altered brain perfusion : regional decreased or increased,
depends on disease time course (Fig.
14,
15).
Complications diagnosed radiologically at presentation of PRES
- Cerebral ischemia: Cerebral infarction is seen as high DWI signal intensity
with a decrease in the apparent diffusion coefficient below 20 %.
Cerebral
infarction is among the early signs of non-reversible damage associated with
adverse outcomes [13].
This complication was present at the acute phase of
PRES in 9 (10%) of the 82 patients with available DWI in one study [11]
and in 5 (23%) of 22 patients in another [13].
In this setting,
every effort
must be taken to exclude a reversible cerebral vasoconstriction syndrome
defined as at least two narrowings per artery on two different cerebral arteries at brain magnetic resonance angiography (MRA) or at conventional angiography [15].
Ducros et al.
reported a 9 % incidence of PRES in reversible cerebral vasoconstriction syndrome [15].
- Cerebral hemorrhage: Cerebral hemorrhage is uncommon in PRES (5 % [7] to 17 % [14] of patients).
Reported cases were about evenly distributed in three categories,
parenchymal hematoma,
subarachnoid hemorrhage,
and focal intraparenchymal hemorrhage [14,
16].
Cerebral hemorrhage may be more common among patients with allogeneic bone marrow transplantation or anticoagulant treatment,
whereas blood pressure levels may have no influence on the bleeding risk [16].
A statistically
significant association has been reported between edema severity on
FLAIR sequences and bleeding risk [14]. In the presence of cerebral or subarachnoid hemorrhage,
vascular imaging must rule out cerebral aneurysm and reversible cerebral vasoconstriction syndrome.
- Cerebral herniation: Posterior edema,
particularly when located in the cerebellum and brainstem,
may cause transtentorial cerebral herniation [17].
Retrospective Diagnosis of PRES after Regression of the Initial Clinical and Radiological Abnormalities
In some cases,
the diagnosis of PRES remains in doubt.
In this situation,
regression of the clinical and radiological abnormalities with appropriate treatment supports the diagnosis.
Thus,
repeated brain imaging is helpful.
Differential Diagnosis
The non-specific clinical manifestations and multiplicity of radiological patterns raise diagnostic challenges.
Many conditions may resemble PRES,
including ictal or post-ictal state (with or without status epilepticus),
progressive multifocal leukoencephalopathy (PML),
severe leukoaraiosis,
cerebral autosomal dominant arteriopathy with subcortical infarcts and leukoencephalopathy (CADASIL), infectious encephalitis,
acute disseminated encephalomyelitis,
mitochondrial myopathy encephalopathy lactacidosis and stroke-like episodes syndrome (MELAS),
vasculitis,
Creutzfeld-Jakob disease,
cerebral venous sinus thrombosis, and ischemic stroke (watershed or posterior cerebral artery territory) [18,
19].
Diagnostic Strategy
The diagnostic strategy for PRES is fairly well standardized.
After a careful history and thorough physical examination,
investigations should be performed as appropriate,
starting with the simplest and moving to the more sophisticated.
CT may be easier to obtain first.
However,
MRI must be performed,
either as the first or as the second imaging study.
MRI is considerably better than CT for the diagnosis of PRES and can provide information regarding many of the causes of PRES [1–3,
6,
7,
11,
13].
MRA must be added to MRI to identify an associated cerebral reversible vasoconstriction syndrome.