Case 1
Female, 15 years old at diagnosis (October 2004).
The patient had a left ankle sprain three years ago.
Since then she had had edema and swelling in the lateral aspect of the midfoot,
and pain with exercise which was increasing lately.
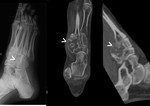
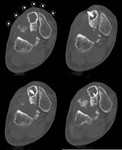
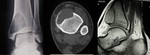
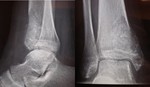
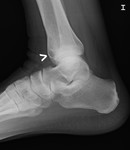
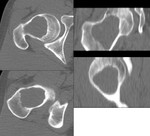
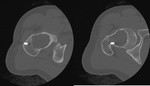
X-ray and CT images show expansive and trabecular lesion in the lateral cuneiform of the right tarsus without soft-tissue component ( Fig. 4 ).
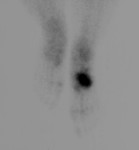
Bone scan shows increased uptake activity(99mTc-phosphates) ( Fig. 5 ).
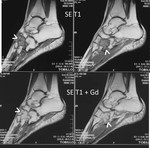
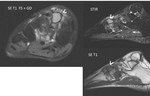
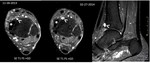
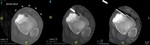
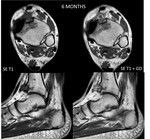
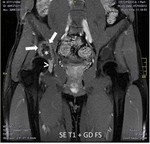
The tumor is isointense to muscle signal on T1 weighted images and light hiperintesity signal on STIR.
High and homogeneous gadolinium enhancement (>) is depicted ( Fig. 6 ).
Pathology following percutaneous ultrasound guided biopsy was reported as bone giant cell granuloma vs giant cell tumor.
Surgery as described in methods and materials was performed with GCT diagnosis.
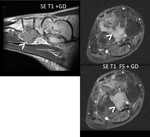
Second surgery was performed due to recurrence one year later (>) ( Fig. 7 ).
Follow-up with MRI monitoring showed slow but clear growth of another recurrence (three years later),
which was treated with radiofrequency thermal ablation,
with a good outcome without any complications ( Fig. 8 ,
Fig. 9 ).
To date,
he patient is asymptomatic with no evidence of recurrence or residual tumor after five years follow-up ( Fig. 10 ).
Case 2
Male,
35 years old when he was operated on September 2007 of a giant cell tumor in distal epiphysis of left tibia ( Fig. 11 ,
Fig. 12 ,
Fig. 13 ).
He was re-operated of a local recurrence in June 2009,
and of another recurrence in medial malleolus in September 2012. Adjuvant cementoplasty was also used this time.
One year later (November 2013),
imaging follow up showed a small lytic lesion in anterior margin of the tibial epiphysis,
adjacent to the subchondral cortical bone (>) ( Fig. 14 ,
Fig. 15 ) * Cement.
Histology was confirmed by percutaneous biopsy.
It was treated by radiofrequency thermal ablation ( Fig. 16 ).
Follow-up: Small residual inflammatory lesion without gadolinium enhancement but peripheral thin wall in the six months post-procedure imaging monitoring ( Fig. 17 ).
The patient is asymptomatic with complete recovery.
Case 3
Male,
25 years old.
He has had pain at the lateral part of the right hip for the last six months after doing exercise.
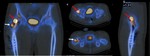
Bone scan showed a positive lesion with increased uptake of the tracer in right femoral neck.
CT and MRI showed an osteolitic
lesion with clear thinning of the cortical bone but no soft tissue component ( Fig. 18 ).
Percutaneous CT guided biopsy was performed with cauda-craneal approach just below greater tuberosity ( Fig. 19 ).
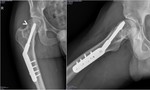
Surgery treatment was performed as described plus screw plate (Zimmer) with uneventful recovery outcome.
X-ray two years later showed small radiolucent lesion at the anatomic femoral neck (>) ( Fig. 20 ),
not evident in previous X-rays.
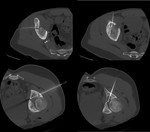
SPECT-CT showed two positive lesions: the proximal one with higher uptake intensity of the tracer (red arrow) and the distal one with lower uptake (white arrow) ( Fig. 21 ).
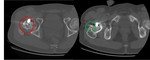
Percutaneous CT guided biopsy showed bone GCT recurrence in the proximal bigger lesion (red circle),
and fibrosis-reparative bone in the smaller one (green circle) ( Fig. 22 ).
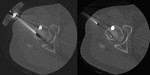
CT guided percutaneous radiofrequency thermal ablation treatment was performed.
Monopolar 17 gauge needle electrode with 10 mm active tip for five minutes ( Fig. 23 ).
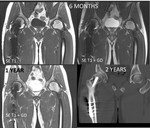
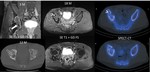
Follow-up: Small stable residual lesion without gadolinium enhancement,
six months,
1 year and 2 years post-procedure.
The patient is asymptomatic with complete recovery ( Fig. 24 ).
Case 4
Male,
21 years old with right hip pain for last six months,
mainly at the beginning of ambulation and exercise.
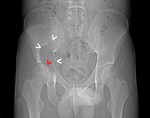
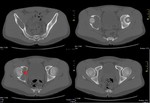
Osteolitic lesion in right iliac bone (white >),
extending to the subchondral cortical of acetabulum which is broken (red >) ( Fig. 25 ,
Fig. 26 ).
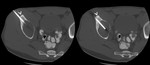
Histology of bone GCT by percutaneous CT guided biopsy through anterior-inferior iliac spine (>),
with 11 G bone biopsy needle ( Fig. 27 ).
Surgery as described was performed without complications.
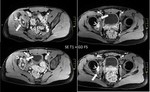
MRI monitoring six months later showed peripheral allograft reactive gadolinium enhancement (arrows),
and suspicion of tumor recurrence at three locations (>).
* Bone allograft.
( Fig. 28 ,
Fig. 29 ).
Recurrence was confirmed by percutaneous biopsy.
We performed percutaneous CT guided radiofrequency thermal ablation treatment by means of four passes at the three foci of recurrent tumour: through anterior approach at the two smaller lesions and two passes through posterior approach at the third bigger intra-articular lesion ( Fig. 30 ).
The treatment of this patient was completed with denosumab.
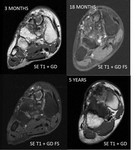
Follow-up 3-18 months post-procedure ( Fig. 31 ): Small stable residual lesion (>) with negative SPECT-CT.
Small stable post-ablation lesion in femoral head (arrows).
The patient had a complete recovery and is asymptomatic.