We selected and analized with US/contrast-enhanced US and MRI/contrast-enhanced MRI six unusual clinical cases from the archives of Operative Unit of Diagnostic Radiology,
C.T.O.
Hospital,
Turin: three lipoma-like well-differentiated liposarcomas, fat necrosis of a lipoma,
an intratendineous lipomatosis,
a posterior interosseous nerve syndrome caused by a supinator intramuscular lipoma.
LIPOMA-LIKE WELL-DIFFERENTIATED LIPOSARCOMAS: SUSPECT ELEMENTS
There are some clinical and imaging features helpful to identify well-differentiated liposarcomas1,2:
- patient age (middle-age);
- large lesion size;
- thickened septa (> 2 mm);
- nodular and/or globular areas of nonadipose tissue within the lesion;
- associated nonadipose masses;
- promiment foci of high T2 signal;
- a total amount of nonadipose tissue composing more than 25% of the lesion;
- enhancement of septa.
But we should be aware that nonadipose areas may be present even within a simple lipoma (muscle fibers,
blood vessels,
calcification,
fibrosis,
myxoid chance),
and there are secondary inflammatory processes that can affect fatty components changing their normal aspect,
such as fat necrosis,
panniculitis,
lipogranuloma formation (events that can occur in a well-differentiated liposacroma,
too).
Triyng to semplify,
we could use this rule: all intralesional components different from few thin and discrete septa and/or bands of muscle fibers (in intramuscular lipomas) raise suspicion for well-differentiated liposarcoma.
It’s important to distinguish these lesions preoperatively.
With these criteria,
in a series of 126 consecutive grossly fatty masses,
Gaskin et al2 reported that MRI was 100% sensitive and 83% specific for well-differentiated liposarcoma,
100% specific for simple lipomas,
showing a poor positive predictive value (38%) for well-differentiated liposarcoma: anyway,
10 of 16 suspicious masses had alternative benign histology.
As a matter of fact,
there’s a number of benign lipoma variants that may present nonspecific imaging features,
such as chondroid lipoma,
osteolipoma,
hibernoma,
angiolipoma,
lipoleiomyoma,
necrotic lipoma.
We want to apply the previously described criteria to three cases with MRI and ultrasonographic aspects that raise the diagnostic suspicion of malignancy.
All cases underwent complete surgical excision,
and histologic diagnosis was “well-differentiated lipoma-like liposarcoma”.
These are mass-type (Figg.
1,
2,
3),
painless and slowly grew lesions,
located respectively deep,
intramuscular,
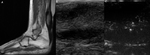
in the proximal third of the forearm (a),
within the right gluteus minimus (b) and in the interfascial plane of the proximal third of the thigh (c).
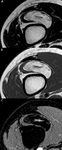
In case (a),
the lesion,
approximately 2.5 cm in diameter,
shows oval morphology and well-defined edges with net margins; the MRI signal is mostly fat,
except for a central tick linear area,
hyperintense in the high contast sequence with fat suppression (STIR),
which directs us to a lesion other than simple lipoma.
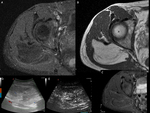
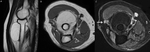
In case (b),
the patient complained of a swelling of the right buttock appeared about 5 months before; MRI highlights a formation within the gluteus minimus muscle,
of about 13 cm,
with adipose signal,
some thick septa inside,
and shaded areas of hyperintensity in STIR sequence at the level of the medial portion,
where the margins appear slightly hazy and a concomitant enhancement both after intravenous administration of gadolinium and ultrasound contrast medium is observed.
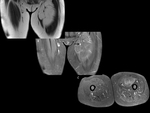
In case (c),
there is a voluminous mass (15 cm) in the interfascial plane,
mainly with fat signal,
that shows thick septa,
nonadipose nodular areas and areas of hyperintensity in STIR sequences,
with some nodules markedly hyperintense on T2-weighted sequences.
FAT NECROSIS OF A LIPOMA: NOT A SIMPLE DIAGNOSIS
Fat necrosis within large lipomas is described in literature,
but rare3.
Because of its rarity,
it’s not well known that a lipoma with fat necrosis may show similar MRI findings to atypical lipomatous tumor.
The appearance of the fat necrosis may consist in globular areas of altered signal,
hypointense on T1 and T2,
with peripheral enhancement,
hypointense stranding due to the presence of fibrous tissue and scarring in or adjacent to the area of fat necrosis,
central fatty signal with a hypointense rim,
or other nonspecific patterns that may vary from those described1,2,3.
Some authors3 suggest incisional biopsy of lipomatous tumors which are indistinguishable in the imaging findings,
and to take samples of not only adipose lesions,
but also the thickened septa in order to reach the correct diagnosis,
because of the risk of harvesting only mature adipose tissue in lipomatous regions.
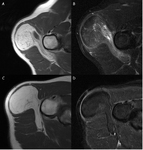
We report a case of a 45 year old man with a mass in the soft tissues of the shoulder (Fig.
4),
already diagnosed three years before as an intramuscular lipoma of the deltoid muscle (diameter 9 cm).
The patient complained of pain and swelling from a month.
The MRI showed a globular hypointense area (1,5 cm) in the context of lipoma,
with rim enhancement and surrounding thick enhancing septa.
Result of needle biopsy was “adipose and connective tissue”.
A magnetic resonance exam was repeated about four months later,
and the globular area of signal alteration previously reported within the lipoma had disappeared,
as well as the septa.
Surgical excision’s been raccomanded,
and the definitive histological diagnosis was that of a lipoma with fat necrosis foci.
We must keep in mind that fat necrosis can happen within both lipoma and liposarcoma.
In low-grade well-differentiated liposarcomas,
both areas of dedifferentiation and fat necrosis can occurr.
For Kransdorf et al,
a well defined nonlipomatous mass juxtaposed with a predominantly fatty tumor is suggestive of dedifferentiation,
but it’s not a rule.
INTRATENDINEOUS LIPOMAS
The appearance is that of hypoechoic well-defined masses within the tendon with loss of normal fibrillar structure.
Obviously they don’t have enhancement after intravenous administration of either gadolinium or ultrasound contrast medium.
Intratendineous tumors are rare4.
We present a case of multiple simple lipomas within the Achilles tendon (Fig.
5),
studied through magnetic resonance and contrast-enhanced ultrasound.
Diagnosis was confirmed histologically.
POSTERIOR INTEROSSEOUS NERVE SYNDROME DUE TO A SUPINATOR MUSCLE LIPOMA: A RARE PARADIGMATIC CASE
When we are sure about the simple lipomatous nature of a mass,
we have to look for harmful effects that the mass can determine,
despite of its benign histology.
Compression effects belong to this category.
Posterior interosseous nerve (PIN) syndrome is a paralysis of the posterior interosseous nerve,
that passes beneath the extensor carpi radialis brevis muscle and then continues between the superficial and deep layers of the supinator muscle.
The PIN is vulnerable in this area5.
Usually PIN syndrome has neither pain nor other sensory symptoms,
but there are cases of forearm pain and paralysis of the extensor muscles of the forearm5.
Rehabilitation is needed for rapid functional recovery of the upper extremity5.
We describe a rare case of compression neuropathy of PIN due to the presence of a 3 cm lipoma within the supinator muscle (Fig.
6),
with MRI signs of neurogenic myopathy of extensor digitorum muscle (reduced volume of muscle and high signal in T2/STIR).
The patient was a 80 years old woman who presented with inability to extend the fingers of the hand gradually extending over 1 year.
Nerve compression must be early diagnosed because the recovery after surgery depends on the duration of symptoms.
For PIN syndrome,
the longest reported duration of symptoms with full recovery postoperatively is 18 months5.