Procedure details:
A descriptive,
retrospective study that included MRI and/or CT scans of 22 patients with a congenital CCJ anomaly.
A cerebro-spinal MRI was performed in all patients,
presenting with neurological symptoms such as intense headache,
torticollis or spinal cord compression,
but also as part of the exploration of a polymalformative syndrome.
MR images were acquired at 3Tesla with either a “spine” or a “head” coil.
Multiplanar sequences weighted in T1,
T2,
FLAIR and diffusion were performed.
A CT scan was performed in addition to the MRI in 10 cases of bony abnormalities of the CCJ using a 16-slice scanner.
We realized helical acquisition with thin axial slices on the CCO,
and further study of the brain with multiplanar reconstructions: sagittal,
coronal and 3D.
Findings:
We report :
-10 cases of bony anomalies of the CCJ:
- 3 cases of basilar invagination.
- 2 cases of platybasia,
one case associated with atlas assimilation.
- 3 cases of foramen magnum stenosis,
2 cases associated with atloido-axoid dislocation within the context of mucopolysaccharidosis and 1 case within the context of achondroplasia.
- 2 cases of mobile odontoid apophysis associated with atloido-axoid dislocation.
-4 cases of Chari-I malformation.
-8 cases of Chiari-II malformation.
1-Bony anomalies
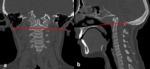
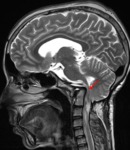
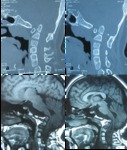
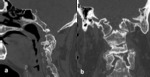
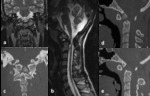
Basilar invagination(Fig.
1,
Fig.
2 and Fig.
3)
Basilar invagination indicates an occipitocervical dysplasia in which there is upward herniation of the margins of the foramen magnum into the posterior fossa [5],
the tip of the odontoid process is more cephalad than normal,
causing compression of the brainstem and spinal cord into foramen magnum potentially resulting in neurological impairment.
The primary form is a congenital skeletal abnormality of the craniocervical junction that is often associated with other vertebral defects such as Klippel-Feil syndrome,
Arnold-Chiari malformation,
odontoid anomalies and hypoplasia of the atlas.
Secondary basilar impression is an acquired deformity of the skull resulting from systemic diseases that cause softening of the osseous structure at the base of the skull,
such as Paget’s disease,
neurofibromatosis or ankylosing spondylitis [6].
Measurements used to evaluate basilar invagination on skull radiographs and CT include [7]:
- Chamberlain's line,
which is drawn between the posterior margin of the foramen magnum and the posterior margin of the hard palate.
In normal conditions,
the tip of the odontoid should not be more than 5 mm above Chamberlain's line.
- McGregor's line,
a line joining the posterior margin of the hard palate to the lowest point of the occipital squama through.
The tip of the odontoid should not be more than 7 mm above McGregor's line.
- Digastric line,
which joins the right and left digastric notches and can be visualized on a coronally reconstructed CT.
The digastric line is supposed to be 11 mm (±4 mm) above the middle of the atlanto- occipital joint.
Basilar invagination is present when the atlanto-occipital joint is at or above the digastric line.
The role of MRI is basically in the evaluation of the cervico-medullary junction for possible mechanic compression and the search of associated abnormalities,
such as the Chiari-I malformation [5].
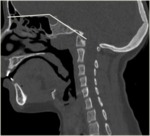
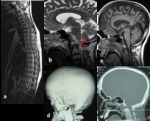
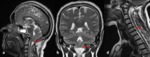
Platybasia(Fig.
4 and Fig.
5)
Platybasia is abnormal flattening of the skull base.
It can occur in a variety of congenital disorders like the Klippel-Feil syndrome [5] or in acquired diseases.Radiographically,
platybasia results in abnormal obtuseness of the basal angle and provides the basis for its evaluation.In the 1940s and 1950s,
basal angles used in the evaluation of the skull base were based on measurements from plain skull images [8].
On radiographs,
the Welcher basal angle can be used to diagnose platybasia.
Lines are drawn from the nasion to the tuberculum sellae and from the tuberculum sellae to the basion.
The angle should be less than 140°.
At present,
evaluation of the brain and skull more commonly involves CT and MR imaging.
The basal angle is measured between a line extending across the anterior cranial fossa to the tip to the dorsum sellae and another line drawn along the posterior margin of the clivus.
Using this technique,
the 95% confidence limits of the means were 116°–118° for adults and 113°–115° for children.
Foramen magnum stenosis
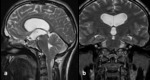
Achondroplasia(Fig.
6)
Achondroplasia is autosomal dominant,
with a frequency of 1 in 26,000 live births [9] and as many as 80% spontaneous mutations.
Clinical manifestations are characterized by short-limbed,
short-trunked dwarfism with craniofacial deformities,
such as macrocephaly,
frontal bossing,
midface hypoplasia and a depressed nasal bridge [10,11].
Newborns with this condition may be hypotonic at birth,
possibly as a result of brainstem compression,
which may also cause sleep apnea and dysphagia.
Most patients are intellectually normal.
The main problem is defective enchondral growth.
Due to this pathology,
disturbance of enchondral ossification may lead to lethal complications like foramen magnum stenosis [12].
On imaging,
there is a small skull base and a small posterior fossa because of underdevelopment of portions of the sphenoid and occipital bones [6].
Achondroplasia has a known association with foramen magnum stenosis that can result in cervicomedullary compression,
which is most often due to a hypertrophied posterior occipital rim and undersized transverse diameter [13].
Stenosis of the jugular foramina causes retrograde venous hypertension that hinders cerebrospinal fluid reabsorption,
frequently causing communicating hydrocephalus [5].
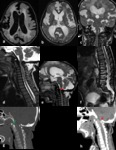
Mucopolysaccharidosis(Fig.
7)
Mucopolysaccharidosis (MPS) represent a heterogeneous group of inheritable lysosomal storage diseases in which the accumulation of undegraded glycosaminoglycans (GAGs) leads to progressive damage of affected tissues.
Seven distinct clinical types of MPS have been identified and described in the literature,
caused by different enzymatic deficiencies.
The typical symptoms include organomegaly,
dysostosis multiplex,
mental retardation and developmental delay.
Definitive diagnosis is usually possible through enzymatic assays of the defective enzyme in cultured fibroblasts or leukocytes.
Radiological and neuroradiological findings are reported.
The most important neuroradiological features include abnormal signal intensity in the white matter,
dilatation of periventricular spaces,
widening of cortical sulci,
brain atrophy,
enlargement of extraventricular spaces and spinal cord compression.
With reference to the skeletal system,
most important radiological findings include multiplex dysostosis,
which is represented by several bone malformations found in the skull,
hands,
legs,
arms and column [14].
The craniovertebral abnormalities found in patients with type VI-mucopolysaccharidosis-(Maroteaux-Lamy syndrome) are described.
The typical finding in patients with this disease is canal stenosis at the level of the foramen magnum and upper cervical spine with or without cord compression.
The stenosis is secondary to thickening of the posterior longitudinal ligament [15].
The atlanto-axial subluxation is also important,
and it is the result of several causes: laxity of the transverse ligament,
dural thickening resulting from deposition of collagen and GAGs,
hypoplasia or absence of the odontoid and indentation of the posterior arch of C1 [16].
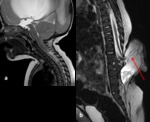
Mobile odontoid apophysis(Fig.
8 and Fig.
9)
The os odontoideum,
or mobile odontoid apophysis,
is a malformation of the cervico-occipital hinge caused by missing unity in the ossification center of the dens on the body of the axis.
This malformation induces atlantoaxial instability and exposes the subject to the risk of bulbar-medullary compression.
The true incidence of this condition is difficult to determine because many cases are asymptomatic [16].
The spectrum of presentation is striking and ranges from patients who are asymptomatic or have only neck pain to those with acute quadriplegia,
chronic myelopathy,
or even sudden death [17].
2-Chiari malformation
Chiari-I malformation
The Chiari-I malformation is characterized by downward displacement of elongated,
peg-like cerebellar tonsils through the foramen magnum into the upper cervical spinal canal,
sometimes associated with distortion of the bulbo-medullary junction and often complicated by hydrosyringomyelia (Fig.
10) and/or hydrocephalus (Fig.
11).
Understanding of the pathogenesis,
clinical manifestations,
and treatment of this abnormality is still controversial [18].
A significant proportion of patients are neurologically normal at presentation,
and the diagnosis is made when an MRI is performed for another reason.
The clinical significance and appropriate management of these patients often remains uncertain.
When present,
symptoms are often vague,
ambiguous,
and may last months to years prior to diagnosis.
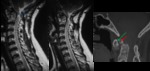
Chiari-II malformation(Fig.
12)
The Chiari-II malformation is a congenital abnormality of the hindbrain characterized by a smaller than normal posterior cranial fossa with downward displacement of the vermis,
brainstem,
and fourth ventricle into the foramen magnum and cervical spinal canal.
Because the posterior fossa is smaller than normal,
there is a lack of vital space for the nervous structures of the hindbrain,
which are squeezed out of the posterior fossa during their growth.
As a result,
there is crowding of the foramen magnum with chronic constriction exerted by bony and fibrous structures on the herniating brain.
This may result in mechanically induced ischemia of the inferior vermis and cervicomedullary junction [5].
Greater than 90% of patients with Chiari-II malformation have open spinal dysraphisms [19].
The most common early symptom of this condition is respiratory stridor,
often occurring within 2 weeks of birth and usually disappearing spontaneously within a few days,
or at most 3 months.
On occasion,
it may be associated with signs of hindbrain dysfunction.
Chiari-III malformation
Since the original paper by Chiari which included the description of a case of cervical spina bifida combined with multiple hindbrain anomalies,
the definition of the Chiari-III malformation has been expanded to include patients with herniation of the hindbrain in a low occipital and/or high cervical cephalocele in combination with pathological and imaging features of Chiari-II malformation,
such as a small posterior fossa,
tectal beaking or enlarged suprapineal third ventricular recess [20].
It is responsible for a significant perinatal mortality.
Prenatal screening is primordial.