Introduction
Celiac disease also termed as non-tropical sprue is a malabsorptive gastroenteropathy caused by small intestinal autoimmune response to gluten in genetically predisposed individuals.
Gluten proteins are found in wheat,
rye,
barley,
and certain other grains.
It is a chronic disease characterized by mucosal lesions of the small bowel that impair nutrient absorption.
Hence it should always be considered as the possible underlying etiology in cases of Iron deficiency anemia of uncertain cause.
Pathology and pathogenesis
Site of pathology
The small bowel mucosa (Submucosa,
Muscularis and Serosa normal) is primarily affected.
The destruction begins in the duodenum and progresses distally to the ileum.
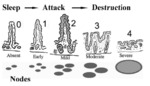
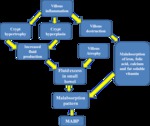
Pathogenesis (Figure 1 and 2)
There is progressive degrees of villous inflammation and destruction with resulting induction of crypt hyperplasia .
Loss of villi,,
which absorb fluid,
and hypertrophy of crypts,
which produce fluid,
result in chronic fluid excess in the small bowel lumen.
The villous atrophy that occurs within the bowel also results in malabsorption of iron,
folic acid,
calcium and fat soluble vitamin resulting in a variety of signs,
some of which may be non-specific.
Chronic excess fluid and its effects on bowel wall structure and tone create the small bowel malabsorption pattern (MABP).
Features of the small bowel MABP
Ø Duodenitis ,
Ø Dilution,
Ø Dilatation,
Ø Slow transit,
Ø Flocculation,
Ø Moulage
Ø Reversal of the jejunalileal fold pattern
Ø Transient small bowel intussusception.
Clinical presentation
The symptoms are wide ranging among patients,
and largely depend on the length and severity of damage to the small bowel.
Malabsorption-
The classic clinical presentation
Ø Diarrhea
Ø Steatorrhea
Ø Flatulence
Ø Weight loss
Ø Fatigue.
Laboratory abnormalities
Ø Iron or folate deficiency anemia,
Ø Hypocholesterolemia,
Ø Hypocalcemia,
Ø Hypoalbuminemia,
Ø Elevated alkaline phosphatase and liver enzyme levels,
Ø Prolonged prothrombin time.
Diagnosis
Radiologic diagnosis /Role of MDCT enterography)
Ø Recognition of small-bowel abnormalities (MABP)
Ø Documentation of normal morphology before biopsy.
Ø Excluding complications like small-bowel intussusception,
ulcerative
jejunoileitis,
lymphoma,
adenocarcinoma,
hyposplenism,
cavitating
lymphadenopathy syndrome,
and pneumatosisintestinalis.
Ø Once the diagnosis is made,
patients with celiac disease need
regular monitoring.
The definitive diagnosis
Ø Peroral suction biopsy material of the jejunum- flat or a villous
mucosal lesion
Other methods
Ø Clinical improvement after the introduction of a gluten-free diet.
Ø endoscopy,
antibody testing.
Antibody testing has
been shown to be both sensitive and highly specific for anti– tissue
transglutaminase and anti-endomysial antibodies.