Materials and Methods
We prospectively studied two adult male patients(34 and 17 years) who attended department of radiology,
Vydehi medical college and research center,
Bangalore.
Both the patients underwent MDCT enterography examination followed by endoscopic biopsy of the duodenal mucosa and histopathological examination.
MDCT Technique
Patient preparation:
The patients were asked to take low residue diet,
ample fluids and laxatives on the day prior to the examination and nothing by mouth on the day of examination.
Preprocedural:
One ampoule of metoclopramide was given intravenously 60 minutes.
200ml of 10% Mannitol was mixed in 1800ml of water.
Patients were then asked to drink 500ml aliquots at 15,
30,
45 minutes after the peristaltic agent is injected.
Metoclopromide is given 60 minutes before procedure.
Procedure
One ampoule of buscopan was given intravenously with the patient on the table.
Non contrast scan was performed initially.
100ml of nonionic iodinated contrast material was injected IV at a rate of 3.5 ml/sec and contrast enhanced scan performed at 20(early arterial),
40(enteric phase) and 70(venous phase) seconds from the start of contrast injection.
Scanning parameters were 140mAs,
120 KVP,
0.6 rot/s,
5mm thickness respectively.
Post procedural
The axial images are reconstructed in coronal and sagittal planes of 1mm thickness.
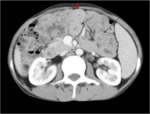
The bowel loops were evaluated for features of small MABP(Both small and large bowels) and enlarged mesenteric lymphnodes.
Results
Both the patients showed classical imaging features.
Both the patients were presented with vague abdominal pain,
chronic diarrhea,
sticky stools and loss of weight.
Radiological /MDCTfindings
Ø Altered jejunal pattern (Figure 3)
Ø Conformation of small bowel-(figure 4 and 5)
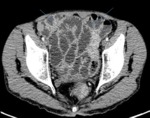
Ø Dilated colon with flatus-(figure 6)
Ø Fat attenuation stool -(figure 7)
Ø Jejunization of ileum -(figure8,
9)
Ø Lymph node prominence-(figure 10)
Ø Prominent mesenteric vessels-(figure 11)
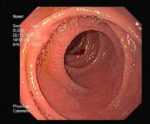
Endoscopic biopsy from the duodenum and the Histopathological specimen of the duodenal biopsy confirmed the diagnosis of the sprue.(figure 12,
13,
14 and 15)
MDCT findings-- Pathophysiology
1.Small bowel MABP
Dilated and fluid filled bowel loops
Ø Chronic inflammatory process of the small bowel loops causes
dilated and fluid filled bowel loops.
Flocculation
Ø There is precipitation of small hyperattenuating flecks in the small
bowel loops termed as flocculation- this will be demonstrated in
CECT examination when it is done with positive oral contrast.
Altered jejunal pattern
Ø Villous distruction and atrophy leads to flattening of the wall,
obliteration of the volulae conniventes and altered jejunal pattern.
there is diffuse thickening of the wall of the jejunum with
submucosal edema leads to dognout appearance.
Jejunalization of ileum
Ø Loss of volvulae conniventes in the jejunum leads to relative
prominent mucosal pattern in ileum.
Telescoping and intussusceptions
Ø The small bowel lumen contains both intrinsic physiologic fluid and
administered enteric contrast material.
Peristaltic waves result in
variable laminar flow of these different fluid components.
Ø The small bowel becomes progressively more flaccid and dilated
leads to telescoping of bowel loops and ultimately intussusceptions.
Conformation
Ø Small bowel loops are prone to conform against each other,
particularly in the pelvis.
2.
Mesenteric lymph node prominence
Ø Autoimmune reaction- regional lymphocytic proliferation
Ø Proliferation of reactive B and T lymphocytes-follicular hyperplasia-
The nodal enlargement.
Ø Prominence of upper mesenteric lymph nodes is a feature of celiac
disease.
Ø The duodenum and proximal jejunum are the initial organs for
autoimmune destruction-nodal prominence in the upper small bowel
mesentery.
Ø Mesenteric lymph node enlargement.
Features of celiac disease lymphnodes
· Low-attenuation lymph nodes
· Cavitating lymph nodes.
3.
Mesenteric vascular prominence
Inflammatory pathology leads to dilatation of the vessels.
4.
Colonic MABP:
All malabsorptive processes affect the colon.
Excess gas in the colon
· The undigested sugar and fat from the small bowel reaches
colon will be “digested” by gas-producing bacteria altering
colonic function and structure.
· Chronic excess gas production leads to colonic distension,
decreased tone ,
altered appearance of colon and stool.
· Gas will be prominent throughout the colon.
Excess colonic fluid
· Excess fluid from small bowel reaches stagnant hypotonic
right colon leads to large volume of colon and cecal plume of
fluid.
Steatorrhea,
encrustated stool, flatulence and constipation
· Unemulsified fat adhere to the colon wall giving the colon wall
an encrusted appearance.
· In lung windows some of the “air” will be revealed to be fat-
attenuation fluid and stool,
a finding indicative of steatorrhea.
· Flaccid,
gas-filled,
low-tonicity colon will not compress and
propel stool.
· The stool will roll and aggregate fatty wall sludge,
producing
large geodes,
round spheres of stool containing fat and air.
With chronic distention,
low tone,
slow transit,
and gas
production,
weak colon peristalsis leads to flatulence and
constipation.
Bowel Calcifications
· With stasis,
the geode wall may calcify due to fat
saponification.
· If the small bowel malabsorption is severe,
large fluid volumes
passed into the colon will overwhelm its absorption capacity
and produce instead of geode formation,
a fluid-filled colon.
Advantage of MDCT over conventional procedures
Each of the listed colonic features alone is insufficient,
but in
summation with small bowel changes,
they should allow the
diagnosis of celiac disease to be suggested.
Because of this summation of small bowel,
mesenteric node,
and colonic appearances,
CT confers a benefit over barium
examination in diagnosis of celiac disease and other
malabsorptive conditions.