Pleural disease:
Pleural disease is one of the most frequent thoracic complications of RA.
It can affect in up to 50% of patients and englobes pleural effusions,
pleural thickening,
empyema and pneumothorax.
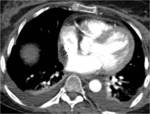
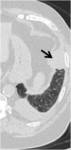
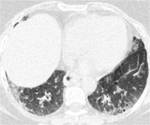
-Pleural effusions and pleural thickening:
Pleural effusion is a common finding in patients with a long-standing RA,
middle-aged men with high rheumatoid factor titer and rheumatoid nodules.
It is usually small to moderate in size and unilateral (Fig. 1),
may be loculated.
Unresolved effusions may lead to marked pleural thickening,
causing a trapped lung with progressive restriction of lung volume,
necessitating pleural decortication and even lung resection.
-Empyema:
Commonly results from colonization of necrotizing subpleural rheumatoid nodules and formation of a bronchopleural fistula and pyopneumothorax.
TB infection must be ruled out in patients treated with TNF-α antagonists.
-Pneumothorax:
Rare complication of RA,
probably caused from perforation of cavitating rheumatoid nodule into the pleural space.
Interstitial lung disease:
Interstitial lung disease (ILD) is a frequent extra-articular manifestation of RA,
being responsible for a significant part of morbidity and mortality associated with this condition.
The estimated prevalence of RA-ILD using HRCT as a method of detection is 20–44%.
This complication is three times more common in males than in females,
affecting individuals with late-onset disease,
high-titer rheumatoid factors,
and in smokers.
It may present several histopathologic and HRCT patterns,
with the most common patterns being usual interstitial pneumonia (UIP),
nonspecific interstitial pneumonia (NSIP) and organizing pneumonia (OP).
There is evidence that HRCT patterns have good correlation with the underlying pathologic pattern,
being able to predict progression and outcome in RA-ILD.
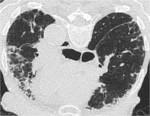
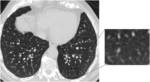
-Usual interstitial pneumonia:
Unlike other connective tissue diseases in which prevails the NSIP pattern, UIP is the most common pattern in RA.
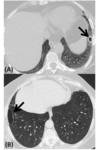
The typical HRCT pattern includes reticulation and honeycombing with subpleural and basal predominance,
traction bronchiectasis,
architectural distortion (loss of volume) and minimal ground-glass opacity.
An anterior upper lobe involvement is also common in RA-UIP (Fig. 2).
This pattern as in the idiopathic pulmonary fibrosis is associated with worse prognosis.
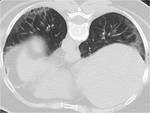
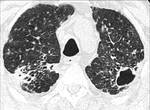
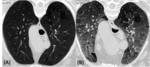
-Nonspecific interstitial pneumonia:
This pattern is characterized by ground-glass opacities with reticulation,
predominantly basal and bilateral (Fig. 3).
Honeycombing may be seen,
but compared with UIP is smaller and less extensive.
Subpleural sparing is a feature that when present helps in recognition of NSIP pattern.
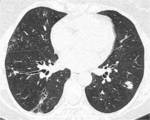
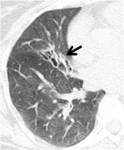
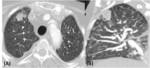
-Organizing pneumonia:
The HRCT hallmarks of OP are bilateral patchy consolidations,
with a predominantly basal/peripheral or peribronchovascular distribution that could change location and size in follow-up exams (Fig. 4).
A highly suggestive finding of OP is the atoll sign (reverse halo sign),
that consists of a ground-glass attenuation surrounded by a ring of consolidation.
Pulmonary rheumatoid nodules:
There is some disagreement about the prevalence of pulmonary rheumatoid nodules; however,
histologically they are similar to rheumatoid nodules located at other sites.
They range in size from few millimetres to 5 cm,
may be solitary or multiple,
predominating in the lung periphery.
Rheumatoid nodules are typically well-defined (Fig. 5),
and may undergo cavitation,
with thick walls (Fig. 6A) that become thinner with healing (Fig. 6B).
Pulmonary rheumatoid nodules must be differentiated from malignant or infectious processes,
especially in a solitary nodule context.
This implies follow-up and in some cases biopsy to exclude malignancy.
Patients are usually asymptomatic,
but nodules can complicate and be associated with pleural effusion,
pneumothorax,
empyema and hemoptysis.
Caplan’s syndrome (rheumatoid pneumoconiosis):
Caplan’s syndrome is a rare complication of RA,
defined by the presence of pulmonary nodules occurring in coal workers or patients with history of occupational exposure to silica dust.
These nodules resemble to rheumatoid nodules,
however histologically in Caplan’s syndrome the nodules are surrounded by pigmented cells.
As with rheumatoid nodules,
they could be single or multiple,
and may cavitate (Fig. 7).
Airway involvement:
-Upper airway obstruction:
The cricoarytenoid joint is one small diarthrodial articulation.
As in other diarthrodial joints,
the cricoarytenoid joints can be affected in RA.
Although most of the RA patients have minor laryngeal symptoms or are asymptomatic,
the prevalence of RA involvement of cricoarytenoid joints in CT is high (54-72%).
Abnormalities that can be seen in CT include cricoarytenoid erosions,
cricoarytenoid luxation,
cricoarytenoid prominence and abnormal position of the true vocal cords.
It is important to remember the involvement of cricoarytenoid joint by RA,
because cricoarytenoid arthritis can be mistaken with a malign tumor (squamous cell carcinoma) or lead to a life-threatening airway compromise.
-Bronchiectasis:
Bronchiectasis is frequent associated with RA-ILD,
however isolated cylindric bronchiectasis with a predominant or exclusive involvement of the lower half of the bronchial tree is a common finding (Fig. 8).
-Follicular bronchiolitis:
Follicular bronchiolitis is characterized by the presence of abundant lymphoid tissue in the walls of bronchioles that may cause compression of the bronchi with airflow obstruction.
This complication manifests in HRCT by the presence of small centrilobular nodules associated with patchy ground-glass opacity and peribronchial nodules.
Nodules and ground-glass opacity are frequently bilateral and with a diffuse distribution (Fig. 9).
Mild bronchial dilatation and with wall thickening is also a common a finding.
-Constrictive bronchiolitis (bronchiolitis obliterans):
Constrictive bronchiolitis is a rare condition characterized by progressive concentric narrowing of membranous bronchioles.
This RA complication is associated with a rapid onset of dyspnea and dry cough,
with a marked obstructive impairment on pulmonary function tests.
The most frequent HRCT findings are bronchial wall thickening,
centrilobular emphysema and a mosaic attenuation pattern with air trapping on expiratory images (Fig. 10).
Unlike the follicular bronchiolitis,
which commonly responds to corticosteroid therapy,
the constrictive bronchiolitis usually has a poor response to therapy and prognosis.
Vascular involvement:
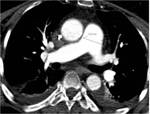
The main vascular complication of RA in chest is pulmonary arterial hypertension (PAH),
which is present in 20 % of patients.
The HRCT signs of PAH include dilatation of the pulmonary arterial trunk (> 29 mm) (Fig. 11),
enlargement of the right heart chambers and contrast reflux into inferior vena cava and hepatic veins.
Infections:
Patients with RA have an increased risk of infections compared with the general population,
this is influenced by RA-treatment (corticosteroids,
disease-modifying agents (DMARDs) and TNFα antagonists).
Pneumonia is a major cause of mortality in these patients.
It was found a dose-related relationship between prednisone use and pneumonia risk,
with no increase risk associated with anti-TNFα agents or methotrexate use.
Mycobacterium tuberculosis,
Listeria monocytogenes and Pneumocystis jiroveci are more common in the therapy with anti-TNFα agents.
Treatment of RA with anti-TNFα agents is associated with an increased risk of reactivation of latent Mycobacterium tuberculosis. The HRCT findings of tuberculosis include cavitary lesions (Fig. 12),
consolidations and nodular lesions with tree-in-bud sign.
Drug-related lung toxicity:
Drug-related pulmonary disease is an important consideration in the differential diagnosis.
Methotrexate is the most commonly used DMARD in RA.
Lung damage or exacerbation of pulmonary disease may occur with low doses.
There are several patterns associated with use of methotrexate,
the most common is acute pneumonitis.
The predominant abnormality in HRCT is ground-glass opacity (Fig. 13).