Procedure details
- Based on the recommendations of the European Society of Urogenital Radiology (ESUR) we use the following MR protocol to investigate prostate cancer on a 1.5 T MRI unit with the body coil.
We recommend the use of anti-peristaltic drugs.
We also recommend using the same scan parameters for acquisitions in the axial plane for a proper evaluation of the prostate: thickness,
spacing,
matrix and FOV.
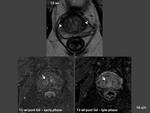
- T2-wi sagittal through the entire pelvis. Sequences included: type FSE JET,
TR = 5907 ms,
TE = 120 ms, NAQ = 1,
Speeder 1,
Thickness/Spacing = 4 mm / 0.4 mm,
Resolution = 0.8 x 0.8 mm.
This acquisition helps us to program the next acquisitions focused on the prostate.
- T2-wi axial cover the entire prostate. Sequences included: type FSE,
TR = 4876 ms,
TE = 120 ms, NAQ = 2,
Speeder 1,
Thickness/Spacing = 4 mm / 0.4 mm,
Resolution = 1.1 x 0.7 mm.
- T2-wi oblique cover the entire prostate with sections positioned perpendicular to the interface between prostate and rectum,
respectively in the plane of the seminal vesicles and ejaculatory ducts. Sequences included: type FSE,
TR = 4389 ms,
TE = 120 ms, NAQ = 4,
Speeder 1,
Thickness/Spacing = 4 mm / 0.4 mm,
Resolution = 0.7 x 0.7 mm.
- T1-wi axial cover the entire prostate. Sequences included: type SE,
TR = 625 ms,
TE = 15 ms, NAQ = 1,
Speeder 1,
Thickness/Spacing = 4 mm / 0.4 mm,
Resolution = 0.9 x 1,2 mm.
- DWI axial cover the entire prostate with b values of 0,
1000 and 1500 s/mm2. Sequences included: TR = 4218 ms,
TE = 84 ms, NAQ = 9,
Speeder 2,
Thickness/Spacing = 4 mm / 0.4 mm,
Resolution = 1 x 1 mm.
- MR-dynamic contrast enhanced (DCE MRI) cover the entire prostate in axial plane. Sequences included: type 3D FFE (Fast Field Echo) FatSat Dynamic,
TR = 4.8 ms,
TE = 1.9 ms, NAQ = 1,
Speeder 2 (parallel imaging),
Thickness/Spacing = 4 mm / 0 mm interpolated to 2 mm / 0 mm,
Resolution = 0.6 x 0.6 mm,
duration 10 seconds per cover; repeated as many times as necessary (eg 5-10 minutes continous scan).
- T1-wi late phase cover the entire prostate. Sequences included: type 3D FFE Flow Compensation Isotropic Fat Sat,
TR = 30 ms,
TE = 5.5 ms, NAQ = 1,
Speeder 2,
Thickness/Spacing = 0.6 mm / 0 mm,
Resolution = 0.6 x 0.6 mm.
- STIR coronal through the entire pelvis,
optional seguence when we evidentiated bone lesions. Sequences included: type FSE STIR,
TR = 3950 ms,
TE = 48 ms, NAQ = 1,
Speeder 1,
Thickness/Spacing = 4 mm / 1 mm,
Resolution = 1,2 x 0.9 mm.
MR findings in the prostate cancer using mp-MRI
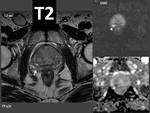
- T2-wi acquisitions. Prostate cancer is easily detected in the peripheral zone,
which appears as an area of low signal intensity,
in contrast cancer located in the central gland in older patients is difficult to distinguish from benign prostatic hyperplasia using only T2-wi sequences (Fig. 11).
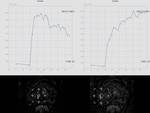
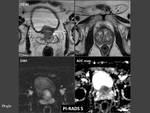
- MR-dynamic contrast enhanced (DCE). A lesion is suggestive of prostate cancer if it shows early intense enhancement and fast washout of contrast agent with type 3 of time-intensity curve,
especially if associated a focal asymmetric enhancing lesion or lesion at an unusual place (Fig. 12, Fig. 13).
When the tumoral lesion is located in the transitional zone in older patients is difficult to differentiate from adenomatous nodules of benign prostatic hyperplasia,
using only DCE-MRI sequence,
these showing more frequently a type 2 of time-intensity curve (plateau).
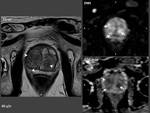
- DWI / ADC map. The prostate cancer appears as a lesion with high signal intensity on DWI corresponding to low signal intensity on ADC map indicating restricted diffusion (Fig. 14).
Using a high b values increase the detection of prostate cancer,
especially in the transition zone and it helps the differential diagnosis between malignant and benign lesions (Fig. 15).
- For a better detection and characterization of prostate cancer is recommended to use all these MR acquisitions.
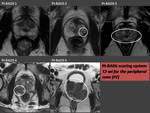
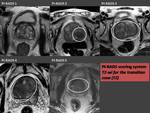
The PI-RADS scoring system
- In the following figures each PI-RADS score are present with MRI examples for each acquisition as follows:
- T2-wi in the peripheral zone (Fig. 16);
- T2-wi in the transition zone (Fig. 17);
- DCE MRI (Fig. 18, Fig. 19);
- DWI / ADC map (Fig. 20,
Fig. 21).
Local staging of prostate cancer
- Using mp-MRI improves detection of prostate cancer,
and also its characterization,
indicating more accurate extracapsular extension and invasion of seminal vesicle,
distal sphincter,
bladder neck or other surrounding structures.
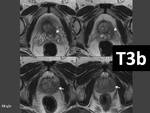
- This improved staging of prostate cancer,
especially in differentiating stages T2 and T3a.
It is much easier to identify abutement,
irregularity,
bulge or loss of the prostatic capsule.
- In the following figures are present MRI examples regarding the T staging of prostate cancer (Fig. 22,
Fig. 23,
Fig. 24,
Fig. 25).
The differential diagnosis of the prostate cancer
The differential diagnosis of the prostate cancer is mainly performed with these pathological entities:
- Benign prostatic hyperplasia appears as a well-defined area with nodular structure located in the central gland that compress the peripheral zone (Fig. 26).
- Chronic prostatitis,
scars or post–radiation therapy changes usually appears as an area of low signal intensity with a wedge/linear shape and a diffuse distribution within prostate without mass,
more easily identified in the peripheral zone (Fig. 27).
Acute prostatitis appears as an area with high signal intensity on T2-wi and low signal intensity on T1-wi; acute prostatitis can extend through the prostatic capsule into the surrounding structures.
- Prostatic changes after biopsy. Blood within prostate after biopsy appears as areas with high signal intensity on T1-wi and low signal intensity on T2-wi.
We suggest to avoid MRI examination for 6-8 weeks after the procedure (Fig. 28).
- Prostatic calcifications appears as punctuate areas with low signal intensity on both T1-wi and T2-wi sequences (Fig. 29).