We evaluated 257 patients underwent to chemiodiscolysis in the period between June2011 and September 2014 (163 men,
94 women ;age range 22 92years),
(L3-L4,
12 patients; L4-L5,
23 patients; L5-S1,
222 patients) after preliminary clinical evaluation,
performed by one experienced neuroradiologist with 35 years experience.
The procedures were performed by two neuroradiologists(respectively 35 and 5 years experience) .
Prospective trial was approved by the Medical Ethical Committee of our institution.
All participants gave written informed consent prior to enrollment.
Inclusion criteria comprised lumbar disk pathologies documented on CT and MR images,
pain for at least 8 weeks with no or poor clinical improvement after conservative therapy,
and initial mean VAS11greater than 3.
Exclusion criteria comprised pregnancy,
referred allergy to proposed drugs and syndromes that are able to mimic the symptoms of a lumbar disk herniation as facet syndrome,
sacroileitis,
bone lesions,
or previous spine surgery.
Thereafter,
patients were undergone follow-up clinical examination performed at sixth month after oxygen-ozone(O2-O3) discolysis.
The outcome was measured the day of the procedure and subsequent follow up at sixth month,
using a visual analog scale (VAS)11,
ranging from 0 to 10 with cut-off 3.
The questionnaire was administered by the same neuroradiologis.
MR imaging and Injection tecnique-Each participant underwent MRI exams of the lumbar spine in our radiology department (using GE Healthcare - Signa EXCITE 1.5T MRI scanner with a phased-array spine coil) before oxygen-ozone(O2-O3) discolysis.
Sagittal FSE-T2 and T2 Fat-weighted images were acquired with the following parameters: 4000/108/4 (TR/TE/NEX),
while for sagittal SE-T1 weighted images 500/20/2(TR/TE/NEX). Both T1 and T2 weighted images were acquired using the same values of matrix (256 x 192),
slice thickness 5 mm,
spacing 1 mm and a field of view (FOV) of 26 cm.
Axial T2 weighted images were acquired parallel to the disk space with a field of view(FOV) of 17 cm.
According to the recommendations of the combined task forces of the North American Spine Society,
the American Society of Spine Radiology and the ASNR12,
on FSE-T2,
FSE-T2 fat and SE-T1-weighted images, the type of herniated disk was classified as protrusion,
extrusion and bulging.
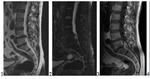
Disk degeneration and dehydration was assessed on the MR T2-weighted sagittal images by using a five-point scale according to the method of Pfirrmann et al13(Figure 1).
All procedures were performed by two neuroradiologists (respectively 35 and 5 years experience),
under CT guidance (Somatom Plus 4; Siemens Medical Systems,
Erlangen,
Germany) and with the patient in the prone position.
Before every procedure,
the patients received premedication with intravenously administered 1 g of cefuroxima (CUROXIM; GlaxoSmithKline) and 50 mg of ranitidine (Zantac: GlaxoSmithKline).
The O2-O3 gas mixture was achieved by using an ozone generator (OZO2 Futura; Alnitec,
Cremosano,
Italy). After local anesthesia using 6mg of mepivacain( about 2-3 mL of MEPICAIN 2%: Monico SPA,
Venice,
Italy),
the spinal needle (9 or 13 cm 22 gauge) was advanced to the intraforaminal space with an angle between 45° and 60°.
Intradiscal and intraforaminal injections were administered with a paravertebral approach in 59 patients and an interlaminar approach in 9 patients.
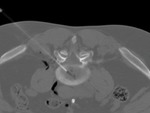
Before injection inside the disk,
a CT scan was used to confirm that the needle tip was inside the nucleus pulposus.
After injection a CT scan was acquired to evaluate O2-O3 distribution which was considered satisfactory when the gas was homogeneously distributed inside the nucleus pulposus with diffusion in the epidural and periganglionic space.
After this last evaluation,
the needle was removed and the procedure was concluded. Overall,
the average injected volume of O2-O3 in patients was 8-10 mL(28µg/ml concentration).
Every patient additionally received 4mg of betamethasone in the periganglionic area(Figure 2).
Statistical analysis-An evaluation of the success rate was performed on the basis of the VAS scale.
The results of the VAS questionnaire were entered in a database.
The success rates at 6-month follow-up was compared by means of the χ2 test.
P< 0.01 was considered to indicate a statistically significant difference.
The software used for statistical analysis was Stata (version 8.2; Stata- Corp,
College Station,
Tex).