The role of breast MRI in the assessment of axillary lymph nodes in breast cancer
The main goal for pre-operative imaging is to identify the presence of axillary metastases with a positive predictive value that is high enough to be useful to the surgeon in deciding when to proceed directly to ALND (axillary lymph node dissection).
ANATOMY OF AXILLARY REGION:
Familiarity with axillary anatomy is important,
both to be able to thoroughly examine the axilla with ultrasonography (US),
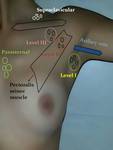
as well as to accurately identify the location of abnormal lymph nodes with any cross-sectional imaging modality (Figure 1).
Level I
- inferolateral to the pectoralis minor muscle
- within the axillary fat
- often seen near the axillary vein
Level II
- receive lymph from level I nodes
- located in the fat behind the pectoralis minor muscle
- also located between the petoralis minor and pectoralis major muscle in an area called the Rotter space
Level III
- receive lymph from level II nodes
- represent the final step in lymph drainage through the axilla and drain into the subclavian lymphatic trunk and supraclavicular nodes,
a path that ultimately leads to the thoracic duct
NORMAL LYMPH NODE MORPHOLOGY:
The normal axillary lymph node should be oval or bean shaped and should have smooth,
well-defined margins.
Normal lymph nodes range in size from few millimeters to about 1-2 cm long.
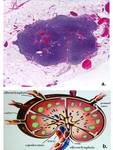
Each lymph node is surrounded by a continuous collagenous capsule and consists of two main regions: outer cortex and inner medulla.
The collagenous capsule is only incomplete at the hilum where a single nodal artery enters the node and a single vein and a single efferent lymphatic vessel exit the node (Figure 2).
METASTATIC LYMPH NODE MORPHOLOGY:
Breast metastases generally enter the node through an afferent lymphatic vessel and then deposit in the subcapsular sinusoids.
Metastatic deposits measuring less than 0.2 mm are called "isolated tumor cells",
and deposits between 0.2 and 2.0 mm are called "micrometastases".
This level of disease is not identifiable at imaging.
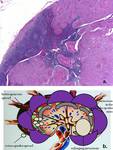
One model suggests that tumor cells spread in orderly fashion from the cortex into the deeper nodal parenchyma,
proliferating along the medullary sinuses and then into the efferent lymphatics (Figure 3).
The growing metastasis coalesces and replaces normal nodal architecture,
resulting then as focal cortical bulge or eccentric cortical thickening,
which is detectable at imaging.
GENERAL IMAGING FEATURES OF LYMPH NODE METASTASIS
US Evaluation
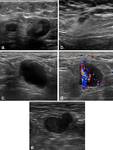
- Diffuse,
focal or eccentric cortical thickening,
partial or complete obliteration of fatty hilum and nonhilar cortical blood flow (NHBF) on color Doppler imaging associated with tumor neovascularity.
The above mentioned findings showed up to be more important than the size criteria in the identification of metastases and this is mainly because metastases can be also present in non-enlarged lymph nodes and thus not all enlarged nodes are malignant.
Imaging findings are described in Table 1 and Figure 4.
Table 1
Selected US Findings of Lymph Node Metastasis
|
US Findings
|
Comments
|
| Diffuse cortical thickening |
Cortical thickness > 3 mm,
relatively nonspecific,
can be seen in reactive nodes |
| Focal cortical bulge |
Should be distinct,
oterwise less specific; more specific if associated with another findings such as NHBF |
| Eccentric cortical thickening |
Should be distinctly eccentric,
otherwise less specific |
| Rounded hypoechoic node |
High specificity in the setting of invasive cancer |
| Complete or partial effacement of the fatty hilum |
High specificity in the setting of invasive cancer |
| NHBF on color Doppler images |
Nonspecific unless combined with another finding,
such as effacement of the fatty hilum |
| Complete or partial replacement of the node with an ill-defined or irregular mass |
High specificity |
| Microcalcifications in the node |
Should correlate with microcalcifications in the primary tumor |
Jacob S.
Ecanow et al.
(2013) Axillary Staging of Breast Cancer: What the Radiologist Should Know.
Radiographics 33:1589-1612.
MRI
- One potential advantage that MR imaging has over US is that it gives a more global view of both axillae.
This capability enhances the detection of potentially abnormal nodes (number,
morphology and functional characteristics) and allows comparison of the axillae.
- It has been shown that the use of dedicated axillary MR imaging protocols improves the accuracy of MR imaging nodal staging.
- Diffusion weighted imaging (DWI) and apparent diffusion coefficient (ADC) are now widely used in routine clinical breast MRI.
- In our practice all patients are imaged in the prone position for both conventional and DW imaging to include as much of the axilla as is possible in the field of view,
from the level of the suprasternal notch line down.
We use axial orientation for bilateral dynamic breast MRI.
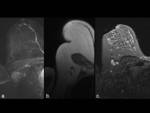
Imaging findings are described in Table 2 and Figure 5.
Table 2
Specific MRI Lymph Node Findings Considered Suspicious
|
Irregular margins or apparent spiculation
|
|
Cortical nodularity or thickening
|
|
Replaced fatty hilum
|
|
Perinodal edema
|
|
Rim or heterogeneous enhancement
|
Jacob S.
Ecanow et al.
(2013) Axillary Staging of Breast Cancer: What the Radiologist Should Know.
Radiographics 33:1589-1612.