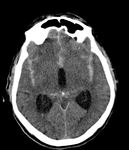
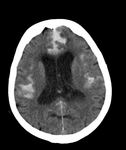
Subarachnoid hemorrhage represents a specific type of stroke,
in which bleeding occurs in the subarachnoid space (Fig.
1,
Fig.
2),
with an average incidence of 6 per 100.000 annually.
Ethiology
The etiology of SAH can be summarized as following:
A. Traumatic SAH (most frequent case)
B. Spontaneous SAH.
It is estimated that more than 80 % of the non-traumatic SAH are caused by the rupture of a cerebral aneurism.
In the rest of the cases,
much less frequent pathologies are involved,
such as:
o Non-aneurismal perimesencephalic hemorrhage
o Arteriovenous malformation
o Cavernous angioma
o Venous thrombophlebite
o Amiloid angiopathy
o Intracranial arterial dissection
o Dural arteriovenous fistula
o Septic aneurism
o Pituitary apoplexy
o Cocaine abuse
The differentiation between traumatic and spontaneous SAH can be sometimes difficult.
This is because sometimes a spontaneous SAH can be itself the cause for an immediate accident,
which leads to traumatic lesions (e.g.
the patient is driving a car while having an aneurism rupture).
Conversely,
sometimes patients can suffer traumatic injuries,
without any visible external wounds.
In these casese,
if it is not possible to obtain an accurate pacient history (e.g.
due to drowsiness),
then a spontaneous SAH can be wrongly suspected.
Clinical manifestations
The manifestations of SAH can vary from an isolated headache,
to sudden death,
but in general its symptoms are characterized by the sudden onset of headaches associated with vomiting and neck stiffness.
The latter represents a very common manifestation,
but it develops several hours after the onset of headache,
and thus its absence at the beginning of the manifestations cannot exclude a SAH.
From a clinical point of view,
the classification of Hunt and Hess recognizes 5 grades of SAH:
· Grade 0: Non-ruptured aneurism
· Grade 1: Non-symptomatic or minimal headache with slight neck stiffness
· Grade 2: Moderate to severe headache,
neck stiffness
· Grade 3: Drowsiness and minimal neurological deficit
· Grade 4: Stupor,
focal deficit,
vegetative disturbances
· Grade 5: Deep coma,
decerebration
The risk of relapse of SAH is maximal in the first 48 hours (50% of relapses),
and then it decreases progressively between the 3rd and the 15th day.
Imagistic diagnostic
The main investigation used when SAH is clinically suspected is unenhanced computer tomography (CT).
In 90% of cases,
the positive diagnostic of SAH is easily established in the first 48 hours,
when spontaneous hyperdensity is visible at the level of basal cistern,
laterals fissures and/or at the level of the interhemispheric cistern (Fig.1,
Fig.
2).
The localization of SAH represents a clue for the localization of the ruptured aneurism.
In very few cases,
at this moment of investigation,
a giant aneurism can be identified at the center of SAH (Fig.
3).
False positive results can be given when generalized brain edema is present,
which causes venous congestion in the subarachnoid space,
and the hyperdense image might wrongly be interpreted as SAH.
The appearance of SAH on a unenhanced CT scan can be classified according to the Fisher scale in 5 grades:
· Grade 1: No visible hemorrhage
· Grade 2: Hemorrhage of less than 1 mm thickness
· Grade 3: Hemorrhage of more than 1 mm thickness
· Grade 4: Parenchymal hematoma or intraventricular hemorrhage
The hyperdensity of SAH diminishes rapidly,
in most of the cases the CT scans being normalized after a period of eight days.
The etiologic diagnostic of SAH is based on the angiography of both common carotid arteries and both vertebral arteries.
However,
since the more frequent use of multislice CT,
the technique of CT-angiography (CTA) has proved to be useful in the visualization of aneurisms responsible of SAH.
It is expected that in the following years,
the angiography performed only as a diagnostic method,
will be used only for the patients with negative CTA.
However,
even if the sensitivity of CTA for the detection of aneuvrisms responsible for SAH approaches that of angiography,
CTA is useful only when it provides a positive diagnostic,
and this is because there are cases when CTA gives false-negative results.
Some already known limitations of CTA in the diagnostic of aneurisms are represented by factors such as the small dimensions of aneurisms or some specific localization of the aneurisms.
It has been shown that aneurisms smaller than 3 mm are much more difficult to detect with CTA.
The same is true for aneurisms located in the intraosseous or petrous segments of the carotid artery.
It is also known that in 15-20% of the cases of SAH,
the angiography cannot identify an aneuvrism.
On the one hand,
this could occur due to the inadequate opacification of the arterial system (non selective or incomplete catheterism,
arterial spasm etc.) or to the superpositions that could make it difficult to differentiate between an arterial loop and an aneurism.
It has also been reported that narrowing of blood vessels because of the vasospasm,
or thrombosis of the neck of the aneurysm or of the whole sac,
might determine the impossibility of visualizing the aneurism.
On the other hand,
it might be also possible that the cause of SAH is non-aneurismal,
in which case other etiologies,
such as the ones previously listed,
should be investigated.