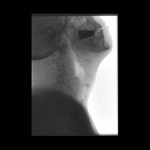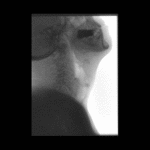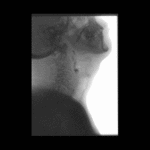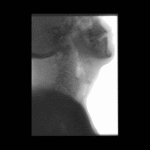
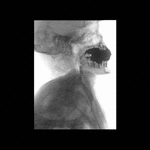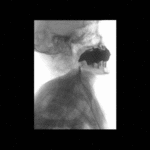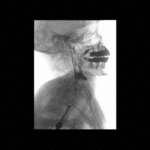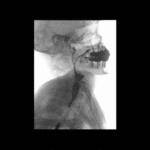
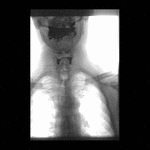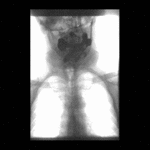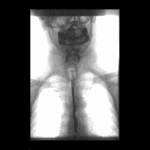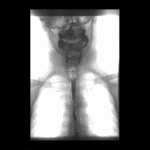
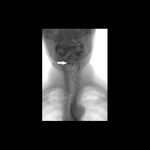
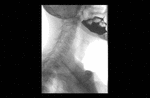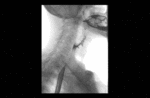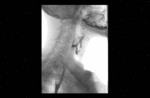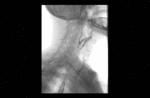
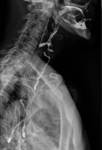
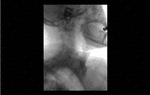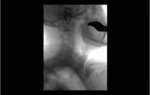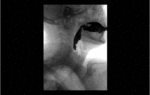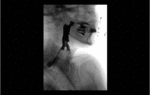
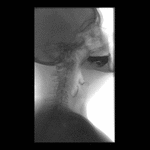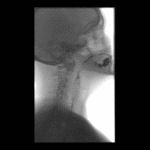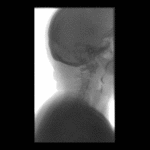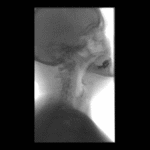
Positioning and acquisition
The patient is placed standing,
in a lateral position.
Following the experience of our centre the lateral projection is enough to achieve an optimal imaging of the structures in most of cases,
therefore it is the only positioning included in our routine protocol.
We reserve the oblique and anteroposterior projections for specific cases,
for example when any asymmetries are suspected.
We use a high image acquisition rate (30 images per second).
In contrast to what it may seem,
it has been reported that a high rate reduces the possibilities of overlooking subtle findings,
so we need fewer swallows to reach a reliable diagnosis.
This shortens the length of the study,
and thus reduces the overall radiation and makes the examination more comfortable for the patient (sometimes it is quite difficult to prevent the patient from losing his patience along the examination).
If the clinical suspicion includes any tumoral pathologies,
or the radiologic findings suggest it,
it is indicated to practise an oesophagogram immediately after the swallowing exam due to the association between neck and oesophageal tumours.
Procedure
The protocol of our institution is based on the model described by Clavé P et al.
We use three different contrast viscosities: pudding,
nectar and liquid (from thicker to less thick).
We add a concrete quantity of a thickening agent (Nutilis powder from Nutricia® in our institution) to a low-density barium suspension.
High osmolar iodine-based contrasts are not recommended in a suspicion of aspiration because of their reported risk of chemical pneumonitis.
We may initially use a water-soluble contrast in patients who have undergone surgery to assess for anastomotic leaks.
To obtain each viscosity,
the thickener amounts that must be added are:
- Pudding: 8 g.
- Nectar: 3’5 g.
- Liquid: 0 g (No thickener added).
- (Optional) Honey: 5 g.
Not in our main protocol,
can be used for the assessment of an intermediate thickness.
A complete VFSE consists of 9 swallows.
We administer increasing volumes of contrast (5,
10 and 20 ml) of each contrast viscosity,
beginning with nectar.
If no security disorders are noticed with the first amount (5 ml),
we continue with the second (10 ml) and then with the third (20 ml).
Then,
after completing the study with nectar viscosity,
we begin again from the first amount,
now administering liquid viscosity.
When the examination with liquid viscosity is finished (with no findings),
we consider that there are no security disorders,
so the administration of any food consistence is safe.
After this,
we can continue the examination with the pudding viscosity if we want to assess the efficacy of a high-density food swallowing.
If a security disorder is noticed within the study,
we write down the viscosity and amount which have caused it.
From here,
we must not administer any higher volume of the same thickness,
nor any volume of a lower viscosity contrast.
If we want to keep on with the examination,
it must be by administering only a higher viscosity.
We follow these criteria because we understand that in a patient who suffers from oropharyngeal dysphagia,
the aspiration risk increases with lower food densities and higher food volumes,
so we take for granted that aspiration will also occur if we decrease the density or increase the amount given.
Pathological findings
The following are the main swallowing disorders we can find:
Efficacy disorders
Oral (preparatory and propulsive) phase:
- Decreased labial closure: contrast falls from the mouth.
- Swallowing apraxia: difficulty,
delay or inability to start the process (often in neurologic diseases,
most common after a stroke).
- Lingual control and propulsion disorders: the bolus is not correctly formed and there can be seen a residue in oral cavity or valleculae.
Pharyngeal phase:
- A symmetric residue in both piriform sinuses is caused by a weak pharyngeal contraction and usually found in neurologic patients.
It also predisposes to aspiration.
- An asymmetric residue in piriform sinuses is often consequence of an unilateral pharyngeal paralysis.
- Cricopharyngeal disfunction: the contrast does not penetrate the oesophagus,
accumulates in hypopharinx and highly predisposes to security disorders.
Security disorders
Oral phase:
- Palatoglossal seal dysfunction: bolus falls to hypopharynx while the airway is still open,
which causes a predeglutory aspiration.
Pharyngeal phase:
- Penetration: the contrast enters the laryngeal vestibule,
without overflowing the vocal chords.
- Aspiration: the contrast overflows the vocal chords and gets into the trachea.
- Lack of coordination of swallowing movements,
for example the delay on the closure of laryngeal vestibule which implies a high aspiration risk.
The report
Although the ideal would be the presence along the examination (beside the radiologist) of a clinician specialized in oropharyngeal dysphagia,
this usually isn’t possible.
This makes crucial the development of a good report by the radiologist so that the clinician can,
after reading it,
understand which is the problem and,
from that point on,
approach his attitude on the most accurate way.
After our experience,
a complete VFSE report,
under our point of view,
must include:
- Pre-test clinical suspicion,
based on the previously made clinical examination and medical history.
- Kinds of contrast viscosities and amounts given.
- Found security or efficacy disorders,
being important to specify which kind and amount of contrast we have administered for each disorder to occur.
- If a security disorder (mainly aspiration) happens,
we should strive to note if it occurs before,
during or after the swallowing.
- Stage where the disorder occurs,
if possible.
- We must indicate if the patient showed any clinical sign or symptom during the examination (for example,
cough),
specially if a security disorder was present.