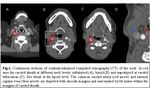
Carotidynia is defined as a neck pain episode,
usually unilateral,
associated with tenderness along the carotid bifurcation and that normally implies an idiopathic benign self-limiting condition.
Initially described by Fay in 1927 [1],
the clinical criteria for the diagnosis of idiopathic carotidynia were established in 1988 by the International Headache Society (IHS) in the first International Classification of Headache Disorders (ICHD-I) [2] as a diagnostic entity consisting in a self-limiting neck pain syndrome and tenderness along the carotid bifurcation without structural abnormality.
In the second edition of the ICHD in 2004,
the Subcommittee of the IHS removed the carotidynia from the main classification [3] and suggested that it was preferable to consider it a symptom of various and heterogeneous causes rather than a primary entity.
However,
they admitted some reports of patients that fulfilled clinical criteria of idiopathic carotidynia according to the first ICHD and that showed radiological findings in the tissue surrounding the symptomatic artery. In 2013,
the third and last edition of the ICHD continued to not recognise carotidynia as a specific cause of craniocervical pain [5].
Different authors have been using the term carotidynia to refer to both the idiopathic clinical syndrome diagnosed according to the clinical criteria described in ICHD-I or,
more generally,
the symptom of pain in the carotid area.
Although the clinical criteria of carotidynia in the former classification of the IHS included absence of structural abnormalities,
several recent publications of isolated case reports describe both histologic (upton et al.
12 in 2003) [5] and radiological findings.
These last ones were initially described with magnetic resonance (MR) [6,7] and,
more recently,
with other other imaging techniques [8-10].
The presence of focal eccentric thickening of the carotid wall and enhancing soft-tissue generally surrounding the distal portion of the common carotid artery and/or carotid bifurcation within the carotid sheat,
without haemodynamic nor lumen changes,
are typical imaging findings in patients suffering from carotidynia.
These findings both indicate that carotidynia could be a distinct entity with structural abnormalities and not just a syndrome as stated by the IHS,
,
possibly caused by inflammation of the carotid adventitia within the carotid sheat,
and point out the practical usefulness of radiological methods in diagnosing this syndrome.
However,
the etiology of this anomaly remains inexplicable.
Carotid sheath
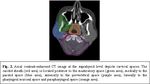
The carotid sheath refers to the anatomical space that surrounds the vascular compartment of the neck and it is where tipically radiological findings of carotidynia appear.
Its wall has contributions from the superficial,
middle and deep cervical fascia and it is located at the lateral boundary of the retropharyngeal space,
extending from the base of the skull to the first rib and sternum deep to the sternocleidomastoid muscle (Fig.
1 and 2).
The four major structures contained in the carotid sheath are the common carotid artery and internal carotid artery,
the internal jugular vein laterally,
the vagus nerve posteriorly between the two vessels and deep cervical lymph nodes.
In the upper part,
the carotid sheath also contains the glossopharyngeal nerve,
the accesory nerve and the hypoglossal nerve.
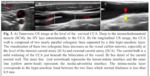
Normal carotid artery ultrasound
Ultrasound (US) evaluation of the cervical carotid arteries is the imaging modality of choice for screening,
diagnosis and monitoring wall disorders of these vessels.
Grayscale imaging evaluates the course and caliber of the carotid arteries as well as allows the evaluation of carotid wall disorders (Fig.
3).