Ultrasound is very helpful in the guidance of percutanous musculoskeletal procedures on the lower limb either to the relatively deep location of some joint structures,
such as the hip (where free-hand techniques are affected by a low level of accuracy) or to the superficial location of other structures that are too small or very close to neurovascular structures.
Diagnostic and subsequent interventional procedures of upper limb are performed using high frequency broadband (7-15MHz) linear transducers,
depending on the depth of the target and the local anatomy.
Needle selection is based on the clinical question to be answered as well as the kind of drugs to be injected.
All devices and drugs (Fig.1) must be prepared in full sterility before the procedure commences and all US-guided interventional procedures must be performed with an aseptic technique in order to avoid any risk of contamination by infectious organisms (bacteria,
fungi,
viruses).
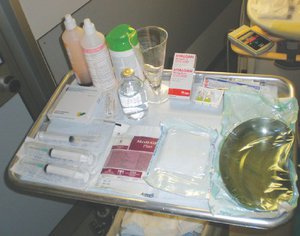
Fig. 1: A well-organized tray containing all the required materials is strongly recommended and includes syringes, anesthetic, antiseptic solutions,saline solution,containers,sterile tissues,gloves and drugs.
Guidance of the needle under US can be performed with either the lateral or co-axial approach.
In the former,
the needle is kept perpendicular to the US beam and is inserted on the short side of the probe.
In the latter,
the needle is inserted on the long side of the probe, parallel to the US beam.
The lateral approach has the advantage of excellent visibility of the needle,
which,
however,
crosses a larger amount of tissue before reaching the target than is the case with the co-axial approach.
On the other hand,
the coaxial approach is burdened by a reduced needle visibility,
but it can be used when the space around the target
is greatly restricted.
However,
adequate experience is needed to achieve satisfactory results (Fig.2).
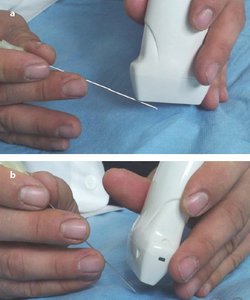
Fig. 2: a)In US-guided lateral approach the needle is inserted on the short side of the probe allowing for an excellent visibility.b)In US-guided coaxial approach the needle is inserted on the long side of the probe, allowing for a reduced path in soft tissues but a poor visibility.
After the interventional procedure the treated skin is covered with a plaster and a compressive dressing and the patient is instructed to apply an instant ice bag over the treated area.
Patients should be monitored for the after-effects of anesthesia for at least half an hour after the procedure.
After they have been instructed regarding the management of possible complications,
such as pain and skin reddening,
in the following hours/days,
they can be discharged from the hospital/clinic.
GENERAL WORKFLOW FOR US-GUIDED
INTERVENTIONAL PROCEDURES
- Verbal and written informed consent is obtained after the patient has received a comprehensive explanation of the risks and possible complications associated with the procedure.
Local regulations may vary among different countries and hospitals.
A representative of the pertinent institution should be involved in formulating an appropriate informed consent form.
- Pre-interventional planning should include a deep knowledge of the procedure and of the materials, as well as a preliminary US evaluation of the lesion.
- Patient positioning on the bed or operating table is particularly important,
with the comfort of both the patient and the operator confirmed in order to avoid any sudden movements by either one.
- Operator sterility: accurate and effective hand hygiene is the most important component of good infection prevention and control,
given that the hands are a common route of infection transmission; transient bacteria can be removed by effective hand hygiene techniques, by washing the hands with an antimicrobial liquid soap and water,
or by using an alcohol-based hand rub.
Sterile gloves, coats and hats are mandatory.
- Both the US equipment and the probe are swiped with dedicated antiseptic tissues and,
if required for the procedure,
a sterile probe cover is used.
- All devices and drugs should be prepared in full sterility before the procedure commences.
The availability of an organized tray with all materials is recommended.
- Operating field delimitation with adhesive sterile towels should be performed by the sterile operator.
- Skin antisepsis should be as accurate as possible,
thus we recommend a 2-step antisepsis procedure: (1) the area to be treated is wiped with a brown water-based 5% povidone-iodine solution; (2) after 3–5 min (time required to let this antiseptic to act),
the same area is wiped with a transparent 2% chlorhexidine-based solution,
which denatures the proteins and disrupts the cell walls (this second step improves skin sterility and avoids staining of the US probe).
- Antiseptic solutions usually create a good coupling between the skin and the US probe.
When longer procedures are performed (e.g.,
the treatment of calcific tendinitis),
a small amount of sterile contact gel can be used.
« Learning objectives





