CONGENITAL URACHAL ANOMALIES
Congenital anomalies of the urachus are twice as common in men than in women.
There are five types of congenital anomalies: patent urachus,
umbilical-urachal sinus,
vesicourachal diverticulum,
urachal cyst and alternating sinus.
The patent urachus is purely congenital and represents about 50% of all cases of congenital anomalies.
The others are normally closed at birth,
but become reopened in association with pathological conditions that are often classified as acquired diseases.
These anomalies are usually associated with congenital abnormalities of the lower urinary tract such as posterior urethral valves or complete ureteral atresia.
Most patients with urachal anomalies (except those with a patent urachus) are asymptomatic.
The most common complication is infection,
which occurs in about 25% of symptomatic cases.
Other complications include bowel obstruction,
urinary tract injury,
hemorrhage and cyst rupture causing peritonitis.
The urachal anomalies are best treated with surgery combined with antibiotic therapy.
Incision and drainage are not considered suitable due to the risk of recurrence of infection and,
more importantly,
because of the hidden risk of adenocarcinoma or malignant degeneration of the lesion.
Patent urachus
The patent urachus is a tubular connection between the anterosuperior wall of the bladder and the umbilicus.
This abnormality occurs in 1 in 200,000 live births.
If there is a persistent communication,
loss of urine is usually observed during the neonatal period.
In about one third of cases,
this condition is associated with posterior urethral valves or urethral atresia.
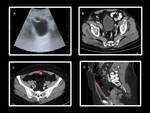
A definitive diagnosis can be made with sinography or cystography,
or can be demostrated with ultrasound or CT during the bladder-filling stage.
Urachal sinus
The umbilical-urachal sinus consists of a blind dilatation of the urachus at the umbilical end,
being patent therefore only in the umbilicus.
This rare congenital lesion is usually associated with an urachal cyst.
The urachal sinus is clinically evident as inflammation or umbilical mass,
with or without drainage,
and is usually associated whit an infection.
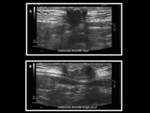
Ultrasound can show a thickened tubular structure along the midline or below the umbilicus,
with an echogenic center,
confirmed with sinography.
Urachal diverticulum
The urachal diverticulum develops when the supravesical portion of the urachus is not closed and therefore the urachus communicates only with the bladder dome.
Represents 3% of all urachal abnormalities and is usually asymptomatic in adults.
It is usually discovered incidentally on CT performed for reasons unrelated,
and appears as a cystic lesion in the midline just above the anterosuperior wall of the bladder.
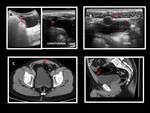
Ultrasound easily demonstrates a fluid-filled sac protruding extraluminally and not communicating with the umbilicus.
They are best demonstrated in cystography and urography,
when the bladder is opacified.
This lesion tends to be found in patients with chronic urinary tract obstruction and may be complicated with urinary tract infection,
the formation of intrauracales calculations,
and an increased prevalence of carcinoma after puberty.
In infants,
the vesicourachal diverticulum is commonly accompanied by the Prune-Belly syndrome.
Urachal cyst
The urachal cyst develops when the urachus is obliterated in the bladder and umbilical ends,
remaining a permeable portion between these points. They are the most commonly described abnormalities (1 in 5000 individuals found in autopsies),
representing 30% of all urachal anomalies.
It occurs mainly in the lower third of the urachus and less frequently in the upper third.
Urachal cysts are usually small but vary considerably in size.
They become symptomatic when enlarged but sometimes are found in the form of incidental masses during a routine examination.
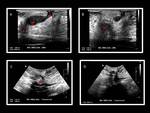
CT or ultrasound show a fluid-filled cavity in the midline lower abdominal wall.
The scan can show a better definition of the anatomical relationship of the cyst with the bladder and its morphology and extension.
The eggshell calcification of the cyst wall is seldom reported.
As with other urachal anomalies,
infection is the most common complication and most cysts are infected at the time of diagnosis.
Superinfected urachal cyst is seen as a thickening of the wall showing greater attenuation than water on CT and mixed echogenicity on US.
Alternating sinus
The alternating sinus is a cystic dilatation of the urachus that periodically empties into the bladder or the umbilicus.
It is a very rare anomaly whose clinical and radiological characteristics are similar to those of urachal sinus.
US can confirm the diagnosis in about two thirds of cases.
ACQUIRED URACHAL ANOMALIES
Infection
Urachal remnants that remain abnormally patent are often subject to infection. The route of infection may be lymphatic,
hematogenous or from the bladder,
and a wide variety of gram-negative and gram-positive microorganisms have been described from infected urachal remnants.
Rarely,
spontaneous rupture of an infected cyst in the abdominal cavity leads to localized or generalized peritonitis.
Due to its complex echogenicity on US and to its variable enhacement with contrast on CT,
makes it difficult to differentiate infected urachal remnant from carcinoma.
In most cases,
percutaneous needle biopsy or aspiration of fluid is required for diagnosis and treatment planning.
In most cases,
you should remove the cyst wall to prevent reinfection and development of neoplasia.
Tumors
The urachal tumors are rare tumors representing 0.5% of all bladder tumors.
They are most common in the middle age and elderly populations and about 70% of affected individuals are male.
Although normal urachus is most commonly cover by transitional epithelium,
carcinoma manifests predominantly as adenocarcinoma (90% of cases). However, 75% of urachal neoplasms in patients younger than 20 years have been sarcomas.
Another histological classification divides urachal adenocarcinomas in tubular,
papillary,
mucinous or colloid,
and signet ring carcinoma.
These histological features are the ones which correlate with survival being the mucinous tumors the ones that have best prognosis compared to other subtypes.
Urachal benign neoplasms including adenomas,
fibromas,
fibroadenomas,
fibroids and hamartomas are extremely rare; however,
they are important because they mimic malignancy of the urachus.
Urachal tumors are typically silent due to its extraperitoneal location,
for this reason,
most patients present with locally invasive or metastatic disease at presentation.
They usually manifest clinically with hematuria and suprapubic mass.
Metastases initially present in the lymph nodes of the pelvis,
followed by systemic metastases to the lungs,
brain,
liver and bone.
Urachal carcinomas can be confused with primary tumors of the bladder dome,
but unlike bladder tumors,
tumors of urachus have a propensity to grow in the perivesical space towards the umbilicus.
A primary bladder carcinoma arising in the mucosa of the bladder dome is often manifested with less extravesical component than seen in urachal neoplasm.
90% of urachal carcinomas arise in the juxtavesical portion of the urachus.
The minority of them are in the center of the urachus (6% of cases) or near the umbilical end (4%).
Some tumors are diverted to the right or left paramedian because during embryonic development.
As with other mucinous adenocarcinomas of the abdominal organs,
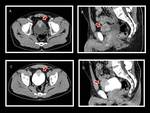
urachal carcinoma may possess typical psammomatous calcifications that are well represented in the scan (50% -70% of cases).
Calcifications in a midline supravesical mass are considered almost diagnostic of urachal carcinoma.
In CT,
urachal carcinoma may be solid,
cystic,
or a combination of the two.
The components of low attenuation are seen in 60% of cases,
reflecting mucin content.
A discrete spiculation or involvement of surrounding fat is suggestive,
but not specific to tumor infiltration because many infections have shown perilesional inflammatory spread overlaid with peritumoral involvement.
US allows tumor localization and detection of highly echogenic calcifications and solid components of the tumor in the anterior abdominal wall.
As mentioned,
it is difficult to distinguish remains of infected urachal urachal carcinoma.
The presence of hematuria,
mural nodularity and calcification on CT,
together with the lack of adjacent inflammatory changes,
may be useful as distinguishing characteristics in some cases.
Suspecting urachal adenocarcinoma should always rule out the possibility that it is metastatic,
excluding prostate disease,
female genital tract or gastrointestinal origin possible. There have been described some techniques as criteria for differential diagnosis of urachal adenocarcinoma from colonic origin : urachal adenocarcinoma presents CK7 and CK20-positive,
while colonic has CK7 negative.
The type of urachal tumors treatment is radical or partial cystectomy with "en bloc" excision of urachal tissues from the bladder to the umbilicus,
including the rectus sheath and performing a bilateral pelvic lymphadenectomy.
The prognosis is not good,
since most are diagnosed in advanced stages.
Between 43 and 50% of patients survive 5 years after surgery.
These tumors are considered radioresistant and does not seem to respond to the usual chemotherapy treatments.
In the first two years after surgery,
to 80% of patients relapse (in decreasing order of frequency) in the pelvis,
bladder,
abdominal wall and the surgical scar.