Our series consists of 70 patients admitted to our center for advanced MR exam whose findings included lymphoma in the differential diagnosis; In all patients,
patochistological examination of leasion was done and only by 11 was PCNLS confirmed .
10 patients underwent presurgical in vivo single-voxel MRS at short echo time (TE,
35 ms) and multi-voxel MR spectroscopic imaging at long TE (144 ms).
3.1.Pathohistology
PCNSLS are large B-cell non-Hodgkin lymphomas,
usually high or intermediate grade.
The brain is the only tissue environment in which large B-lymphoma cells accumulate densely around tumor vessels so tumor exhibit angiotropism [2].
Confluent areas of tumor may show necrosis,
with residual viable tumor cells being found mostly around blood vessels [3].
The degree of necrosis differs between the immunocompetent and the immunocompromised hosts,
with the latter group harboring a higher percentage of intratumoral necrosis.
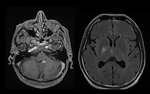
3.2 Anatomical distribution
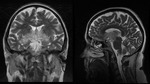
PCNLS are typically located in supratentorial brain parenchyma: the most frequent locations are periventricular white matter,
the basal ganglia and the corpus callosum,
frequently abutting ependymal or subarachnoid surface.
Bilateral basal ganglia (BG) involvement is common.
The brain stem or cerebellum or both are affected in 9%–13%,
and the spinal cord,
in only 1%–2% of patients [5].
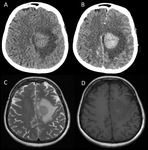
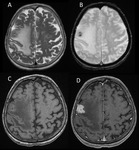
3.3 Imaging findings
Characteristic imaging features of PCNSL are supratentorial contrast-enhancing mass,
relatively homogeneous,
with a diameter of at least 15 mm.
Single tumor manifestations occur in 60–70% of patients,
however,
immunodeficient patients frequently have multiple lesions at diagnosis [1].
The lesions vary in circumscription.
Hemorrhage within the tumor is a rare finding,
more frequent in AIDS patients.
Perilesional edema can be present in variable extent,
from moderate to extensive.
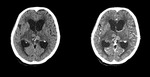
Non-Contrast Imaging: Due to its hypercellular nature,
lymphomas are typically iso- or hyperdense masses on non-enhanced CT,
and iso- or hypointense to gray matter on T1W .
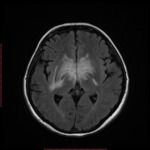
T2W signal intensity varies from hypo- to iso- to hyper- dense.
T2W hypointensity reflects low water content within the cells which have a high nuclear-cytoplasmasmic ratio.
Enhancement patterns: After administration of intravenous contrast in immunocompetent patients,
lymphoma demonstrate pronounced uniform contrast enhancement.
Contrast-enhancing,
thickened ependyma may be seen indicating leptomeningeal infiltration.
Higher degree of necrosis correlates with hyperintensity on T2-weighted MR images and rim enhancement and absence of restricted diffusion.
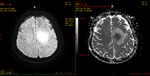
Diffusion-weighted MR imaging: Lymphomas are hypercellular tumors with high nuclear-cytoplasmic ratio; therefore,
PCNSL are frequently hyperintense on DWI and hypointense on ADC maps.
In case of necrotic areas within the tumor the decrease in ADC values is not a consistent finding [4].
High-resolution SWI is much more sensitive than conventional MR imaging for the visualization of small veins,
blood products,
and calcifications,
which appear as low-signal intensity structures.
This is helpful in differentiating PCNSL from high-grade gliomas,
because microhemorrhages and calcifications are rare in PCNSL,
whereas small hemorrhages are frequently seen in high-grade gliomas [5] .
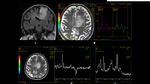
3.4 MRS characteristics
High Cho/Cr ratios and reduced Na are indicators of neoplastic origin,
but nonspecific for lymphoma.
These findings reflects increased cell membrane turnover and breakdown (increased Cho and lipids),
and necrotic portions of the tumor (Lac and lipids) and can also be seen in high grade glioma or metastasis [6].
Increased Lac and lipids along with a prominent Cho peak,
minimal NAA,
Cr,
and mI- depending on the amount of surrounding brain tissue in the voxel - (Figure X).
3.5 Differential diagnosis
Differential considerations include metastasis,
ependymal spread of anaplastic glioma,
demyelinating disorders,
sarcoidosis,
subacute infarcts; space-occupying leasions of infective etiology like toxoplasmosis should be considered in HIV-positive patients.
Involvement of the corpus callosum is suggestive of CNS lymphoma,
but such involvement also occasionally occurs with anaplastic glioma and metastatic neoplasm.
Lymphomas differ from glioblastoma multiforme because they usually have less peritumoral edema,
are more commonly multiple and less commonly necrotic [7] .Metastasis have a predilection for the gray/white matter interface.
Subependymal enhancement should be actively sought on imaging studies as a potential clue to lymphomatous involvement.