This poster is published under an
open license. Please read the
disclaimer for further details.
Keywords:
Liver, Biliary Tract / Gallbladder, Gastrointestinal tract, MR, Contrast agent-intravenous, Neoplasia, Cancer
Authors:
G. Mamone, G. Marrone, G. Gentile, V. Carollo, M. Milazzo, A. Luca; Palermo/IT
DOI:
10.1594/ecr2015/C-2590
Results
The tumors ranged from 2.7 to 15.5 cm (mean 9.1 cm) in maximum diameter.
In 14 patients (48%) satellites nodules near the largest lesion and/or intrahepatic metastasis were detected.
The lesions were located in the right lobe in 21 cases (72%),
in the left lobe in 3 cases (10%),
and in both lobes in 5 cases (17%). Contours of the lesion were lobulated or irregular in all patients but two (93%),
with absence of capsule.
On T1-weighted images,
the IMC appeared as a homogeneous hypointense mass relative to the liver in 25 patients,
and inhomogeneously hypointense in the other 4 patients.
On T2-weighted images,
all lesions were heterogeneous with intralesional hyperintensity. In the arterial phase,
all lesions showed rim enhancement.
On dynamic MRI images,
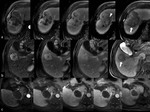
cholangiocarcinoma had the following vascular patterns (Figure 1a,
1b,
1c): a) peripheral rim-like enhancement in the arterial and portal venous phases,
followed by filling-in on the delayed images (n=27; 93.1%); progressive and centripetal filling was observed in 16 cases (59.2%),
while 11 lesions (40.7%) showed progressive dishomogeneous filling.
However,
complete or near complete enhancement in the late phases was observed in only 6 cases (22.2%); b) early inhomogeneous enhancement followed by prolonged complete enhancement (n=1; 3.4%); c) early peripheral enhancement with non-filling of the central area on the delayed images (n=1; 3.4%). In late phases at 10-15 minutes,
24 of 25 lesions (96%) showed late enhancement; 21 lesions (84%) were inhomogenous because of enhancement areas (iso- or hyperintense) mixed with hypointense areas,
while 3 lesions were homogeneously hyperintense; just one lesion was homogeneously hypointense.
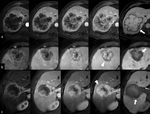
In 56% of cases with 10-15-minute late phase,
a hypointense peripheral rim was identified (Figure 1a,
2b,
2c).
This rim was discontinuous in 12 lesions (86%) but continuous in 2. We had only one case with a hyperintense peripheral rim on 10-15-minute late phase and HBP.
On hepatobiliary images,
only one IMC was hypointense,
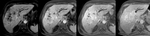
while 28 (96%) lesions showed a mainly central area of enhancement described as a “cloud” (Figure 3).
Furthermore,
82% of IMC (n=24) exhibited a hypointense peripheral rim associated with cloud appearance,
defining a “target pattern” (Figure 1a,1b,2a,2b,2c); this rim appeared continuous in 16 lesions (70%) and discontinuous in 7 lesions.
In 14 lesions (58%) with the hypointense peripheral rim on HBP the hypointense peripheral rim on 10-15-minute late phase coexisted,
but we found no significant association between them (p= 0.150).
Hepatic artery encasement was detected in 8 patients (27%),
invasion of portal vein branches in 10 patients (34%),
and infiltration of hepatic veins in 13 patients (44%).
Narrowing or obstruction of portal vein is not an uncommon finding in IMCs located centrally in the liver. Transient hepatic intensity difference (THID) on immediate gadolinium-enhanced T1-weighted images in the segment with the tumor was observed in 19 patients (65%); 11 patients (57%) with THID showed coexistence of vascular infiltration (no evident causes in the other cases). In 18 cases (62%),
capsular retraction was adjacent to the tumor.
Segmental or lobar atrophy of the tumors lobe was seen in 8 patients (27%),
and encasement of portal vein branches or hepatic veins was observed in 5 patients (62%) with hepatic atrophy.
Dilatation of the intrahepatic bile ducts,
in particular adjacent to the lesions,
was seen in 18 patients (62%).
IMCs originate from bile ducts so biliary obstruction by tumor infiltration can occur.
Metastatic lymphadenopathy was detected in 14 patients (48%),
in the following sites: porta hepatic,
portocaval space,
celiac and para-aortic.
Ascites was observed in 8 cases (28%),
and 4 patients had cirrhosis.