I.
Hepatocellular carcinoma (HCC)
1) Typical finding
Hepatocellular carcinoma (HCC),
the most common primary malignant tumor of the liver is a hypervascular tumor,
usually arising in the cirrhotic liver.
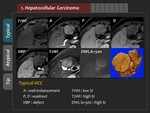
The usual findings of HCC are rapid enhancement in the arterial phase,
decreased signal intensity (“washout”) from the portal phase to the equilibrium phase,
and low signal intensity (“defect”) in the hepatobiliary phase (HBP) (Figure 1,
2).
Rapid enhancement in the arterial phase reflects the fact that HCC receive most of blood supply from the hepatic artery.
Decreased signal intensity in the portal and equilibrium phases corresponds to the “washout” of the contrast materials from the tumor blood spaces and is attributed to the lack of portal venous supply.
As time goes on,
surrounding liver parenchyma absorbs Gd-EOB-DTPA to the maximal degree,
whereas HCC devoid of functioning hepatocytes shows marked low signal intensity in the HBP (“defect”).
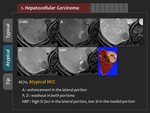
2) Atypical finding
Although hypointensity in the HBP is the typical finding of HCC,
approximately 6-15% of HCCs show iso- or hyperintensity in the HBP (Figure 3,
4).
In functional hepatocytes,
Gd-EOB-DTPA is taken up via the organic anion transporter proteins (OATPs) and excreted into the biliary canaliculi via the multidrug resistance-associated proteins 2 (MRP2).
Previous studies have suggested possible mechanisms of the paradoxical uptake in the HBP.
One study has shown that overexpression of OATP8 and MRP3,
an uptake transporter and an export transporter of gadoxetic acid in the human HCC cells,
respectively was significantly associated with paradoxical uptake in HBP (Figure 5).
Another study has demonstrated that positive expression of OATP1B1 and/or OATP1B3,
combined with decreased expression of MRP2,
or increased expression of MRP2 at the luminal membrane of pseudoglands in the human HCC cells may result in paradoxical uptake in HBP (Figure 6).
3) Tips
In HCC with paradoxical uptake on HBP, images of other phase rather than HBP may be helpful for diagnosis of HCC (Figure 7).
II.
Cholangiocarcinoma
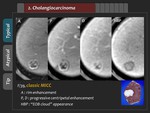
1) Typical finding
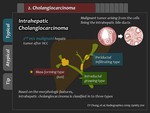
Intrahepatic cholangiocarcinoma (ICC),
the second most common malignant hepatic tumor after hepatocellular carcinoma,
is a tumor arising from the cells lining the intrahepatic bile ducts.
It is classified into three types based on the morphologic features: mass-forming,
periductal infiltrating,
and intraductal growing types.
Among them,
mass-forming ICC (MICC) is the most common type,
accounting for 60% of ICC (Figure 8).
Typical findings of MICC are hypointensity on T1-weighted image,
mild to moderate hyperintensity on T2-weighted image,
irregular rim-like enhancement in the early arterial phase with centripetal enhancement in the late arterial phase,
and delayed washout from the portal phase to the HBP (Figure 9,
10).
Signal intensity on T2-weighted image is dependent on its fibrous tissue and mucin contents,
that is,
fibrous tissue and mucin contents contribute to the lower and higher signal intensities,
respectively.
Characteristic delayed washout pattern,
attributed to the fibrous tissue component make “EOB-cloud” appearance with cloud-like hyperintensity in the central portion and hypointensity in the peripheral portion.
The peripheral portion of the mass with early enhancement and rapid washout represents the active growth of viable tumor,
whereas the central portion corresponds to the loose connective tissue with abundant fibrous stroma (Figure 11).
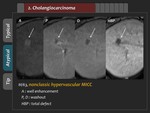
2) Atypical finding
Some MICC may show rapid enhancement in the arterial phase,
complete or nearly complete washout in the delayed phase,
and total defect in the HBP (“hypervascular” ICC).
(Figure 12,
13) Rapid arterial enhancement and complete washout is attributed to abundant tumor vasculature in the fibrous stroma without prominent necrosis,
seen in a well-differentiated tumor.
3) Tips
It may be difficult to differentiate hypervascular MICC from HCC. Capsular retraction,
satellite nodules,
vascular encasement,
hepatolithiasis associated with the dilatation of the bile ducts and obliteration of the portal vein,
and tumor marker such as CA 19-9 may be helpful for diagnosis of hypervascular MICC (Figure 14).
III.
Metastasis
1) Typical finding
The liver is the most common site for metastasis of primary cancers that arise in many other organs,
including colon,
rectum,
pancreas,
breast,
and lung.
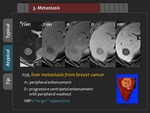
Liver metastasis,
the most common hepatic malignancy,
is far more common than the primary hepatic malignant tumor.
Metastatic lesions in the liver are classified into hyper- and hypovascular types based on the degree of vascularization.
Primary tumors causing hypervascular liver metastasis include neuroendocrine tumors such as carcinoid and islet cell tumors,
renal cell carcinoma,
melanoma,
breast,
and thyroid carcinomas.
Colon,
lung,
breast,
and stomach carcinomas can cause hypovascular liver metastasis.
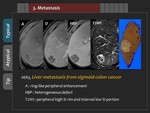
Usual findings of hypervascular liver metastasis are hypointensity on T1-weighted image,
moderate hyperintensity on T2-weighted image,
peripheral enhancement in the arterial phase,
and centripetal progression of enhancement with concurrent peripheral washout in the portal phase and the equilibrium phase.
Hypovascular liver metastasis does not usually show remarkable enhancement in the arterial phase in comparison with the normal surrounding liver parenchyma.
In the HBP,
hepatic metastasis shows “defect” (Figure 15).
Colorectal cancer is an example of primary cancer usually showing “defect” (Figure 16).
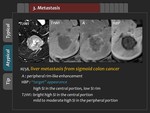
2) Atypical finding
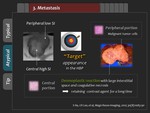
Some hepatic metastasis may show “target” appearance with central high signal intensity surrounded peripheral low signal intensity rim (Figure 17,
18).
However,
"target" appearance is not unusual finding in the liver metastasis from the breast cancer (Figure 19).
Residual enhancement of hepatic metastasis in the HBP can be explained by retention of contrast materials in the intraacinar necrosis or intratumoral desmoplastic area composed of fibrosed tissue (Figure 20).
3) Tips
In the HBP,
"defect" is usual finding in the liver metastasis from the colorectal cancer, whereas "target" appearance is usual finding in the liver metastasis from the breast cancer (Figure 21).
IV.
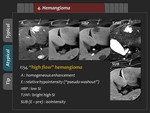
Hemangioma
1) Typical finding
Hepatic hemangioma,
most common benign tumor of the liver,
is made up of a tangle of blood vessels.
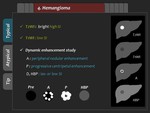
Hemangioma is usually hypointense on T1-weighted image,
and bright hyperintense on T2-weighted image.
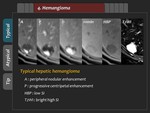
Typical findings of the hepatic hemangioma are early peripheral nodular enhancement in the arterial phase with progressive centripetal enhancement in the portal phase,
and iso- or hypointensity in the equilibrium and hepatobiliary phases.
(Figure 22,
23) Because Gd-EOB-DTPA is taken up by surrounding liver parenchyma,
hepatic hemangioma appears iso- or hypointensity in the Gd-EOB-DTPA-enhanced MR imaging.
2) Atypical finding
“High flow” hemangioma may show rapid,
intense,
homogenous enhancement in the arterial phase.
In the HBP,
“high flow” hemangioma also appears homogeneously hypointense.
(Figure 24,
25) This arterial enhancement and “pseudo washout” pattern makes it difficult to differentiate hemangioma from hypervascular tumors such as HCC.
3) Tips
Signal intensity on T2-weighted image,
apparent diffusion coefficient (ADC) value,
subtraction image,
and extracellular agent may be helpful in distinguishing them.
Hepatic hemangioma shows bright high signal intensity on T2-weighted image,
and ADC value of hemangioma is much higher than ADC value of HCC.
In the subtraction image between the unenhanced and equilibrium phases,
hemangioma demonstrates isointensity or slightly increased intensity,
indicating remained contrast media in the lesion rather than true washout as seen in HCC.
Unlike in the Gd-EOB-DTPA-enhanced liver MRI,
when using extracellular agent,
hemangioma appears hyperintense to the surrounding liver in the equilibrium and delayed phases (Figure 26).
V.
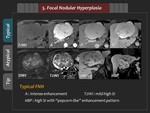
Focal nodular hyperplasia (FNH)
1) Typical finding
Focal nodular hyperplasia (FNH),
the second most common benign tumor of the liver,
is considered a hyperplastic response to a congenital vascular malformation.
FNH are usually iso- or hypointense on T1-weighted image,
and slightly hyper- or isointense with central hyperintense scar on T2-weighted image.
Usual findings of FNH are intense enhancement with “spoked wheel” appearance due to its central scar and radiating fibrous septa in the arterial phase,
and iso- or hyperintensity with “popcorn-like” enhancement pattern due to the accumulation of Gd-EOB-DTPA and poor biliary drainage in the HBP (Figure 27,
28).
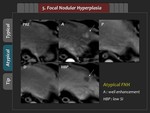
2) Atypical finding
Some FNH may show atypical hypointensity in the HBP (Figure 29,
30).
This atypical hypointensity can be explained by large central scar or abundant fat component within the lesion,
resulting in decreased gadoxetic acid enhancement.
3) Tips
FNH with hypointensity in the hepatobiliary phase is considered containing abundant fat component (Figure 31).
VI.
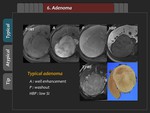
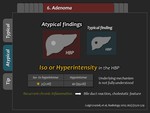
Adenoma
1) Typical finding
Hepatic adenoma is a rare benign tumor,
occurring mostly in young women taking oral contraceptives.
Because hepatic adenoma has risks of spontaneous rupture and malignant transformation,
it is important to differentiate adenoma from other benign hepatic lesions such as FNH or hemangioma.
Hepatic adenoma is usually iso- or heterogeneously hyperintense due to intralesional hemorrhage,
necrosis,
and fat on T1-weighted image.
On opposed-phase T1-weighted gradient echo (GRE) image,
adenoma may show signal dropout because of fatty component.
Typical findings of hepatic adenoma are mild to moderate enhancement in the arterial phase,
washout in the portal phase and delayed phase,
and hypointensity in the HBP (Figure 32,
33).
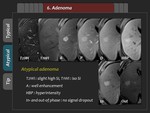
2) Atypical finding
Hepatic adenoma may rarely show iso- or hyperintensity in the HBP (Figure 34,
35).
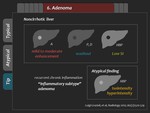
Although underlying mechanism of unusual delayed uptake of adenoma is not fully understood,
one investigation suggested that recurrent chronic inflammation might be attributed to it.
3) Tips
Adenoma with iso or hyperintensity in the HBP is considered as inflammatory subtype adenoma (Figure 36).
VII.
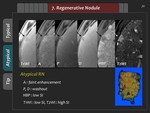
Regenerative nodule (RN)
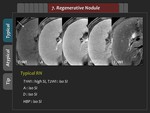
1) Typical finding
Regenerative nodule (RN) is considered localized hepatocellular proliferation entrapped by deposition of extracellular matrix in a cirrhotic liver.
RN is usually iso- to hyperintensity on T1-weighted image,
iso- to hypointensity on T2-weighted image.
Because RN preserves its hepatocellular function,
it appears isointense to surrounding liver parenchyma from the arterial phase to the HBP (Figure 37,
38).
Lipid containing “steatotic” nodules demonstrate signal dropout on opposed-phase T1-weighted GRE image,
and iron-containing “siderotic” nodules appear markedly hypointense on T2- and T2*-weighted images.
2) Atypical finding
Some RNs may show hypointensity in the HBP,
which make it difficult to differentiate RN from HCC (Figure 39,
40).
3) Tips
Arterial phase of Gd-EOB-DTPA-enhanced liver MRI may be helpful in distinguishing them.
Arterial enhancement in the cirrhotic nodules with hypointensity in the HBP is more likely to suggest high grade DN or HCC (Figure 41).
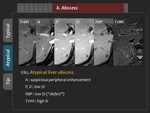
VIII.
Abscess
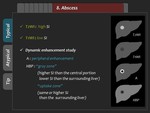
1) Typical finding
Hepatic abscess is a collection of pus in the liver caused by bacterial,
parasitic,
or fungal infection.
Hepatic abscess is usually hypointense on T1-weighted image,
hyperintense on T2-weighted image,
and peripheral rim enhancement in the arterial phase.
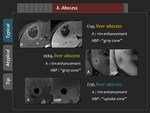
In the HBP,
enhancing rim is seen as “gray zone” (signal intensity higher than central portion and lower than surrounding liver parenchyma) or “uptake zone” (signal intensity same as or higher than surrounding liver parenchyma) (Figure 42,
43).
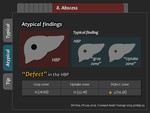
2) Atypical finding
Some hepatic abscess exhibit “defect” rim with signal intensity same as or lower than the central portion in the HBP.
(Figure 44,
45)
3) Tips
Because peripheral washout is a specific sign of metastasis,
“defect” rim of hepatic abscess makes it difficult to differentiate abscess from metastasis (Figure 46).
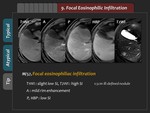
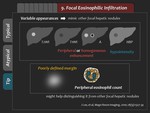
IX.
Focal eosinophilic infiltration
1),
2) Typical and atypical findings.
Focal eosinophilic infiltration (FEI) of the liver is a focal benign hepatic lesion,
occurring associated with a variety of disorder such as parasitic infection,
allergic condition,
internal malignancy,
drug hypersensitivity,
and hypereosinophilic syndrome.
Usual findings of FEI are poorly defined margin,
iso- to slightly low signal intensity on T1-weighted image,
slightly high signal intensity on T2-weighted image,
rim or homogeneous enhancement in the arterial phase with iso- to hypointensity in the portal and equilibrium phases,
and mixed hypointensity in the HBP (Figure 47).
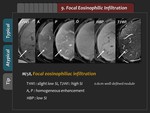
However,
FEI may demonstrate various appearances (Figure 48-50).
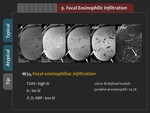
3) Tips
Various appearances of focal eosinophilic infiltration can mimic other focal hepatic nodules.
However,
poorly defined margin and peripheral eosinophil count might help distinguishing it from other focal hepatic nodules (Figure 51).