This poster is published under an
open license. Please read the
disclaimer for further details.
Keywords:
Oncology, Ultrasound, Brachytherapy
Authors:
T. Akbas, G. Ugurluer, M. Acil, T. Arpaci, M. Serin; Adana/TR
DOI:
10.1594/ecr2016/B-0469
Results
Between January 2010 and June 2015,
412 insertions for intracavitary brachytherapy was performed under ultrasound guidance in 113 consecutive patients with cervical cancer.
Previously,
application for 29 patients was done without ultrasound guidance and 2 patients had uterine perforations (6.9%).
The patients were treated with 3D conformal brachytherapy and CT imaging was used for treatment planning.
After detecting uterine perforations with planning tomography,
we decided to perform ultrasound guidance for applicator insertions.
Only one of 113 patients after ultrasound guidance had uterine perforation (0.9%).
The perforation sites for the patients without ultrasound guidance was anterior and posterior uterine wall,
but for the procedure with ultrasound guidance the perforation site was uterine fundus due to a too advanced tandem.
A preliminary pelvic ultrasonography was performed before application at the first fraction in the operative room to assess the uterus (anteversion,
retroversion,
deviation,
myoma et cetera).
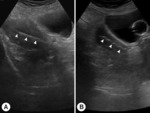
The tandem curvature was selected based upon the uterine flexion before insertion (Figure 1).
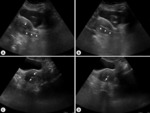
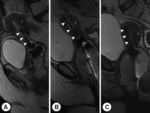
The central placement of tandem was confirmed with axial sweeps and length,
angle and relation with anterior,
posterior and superior walls were confirmed with sagittal sweeps (Figure 2).
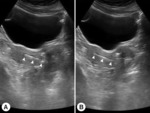
For optimal positioning,
tandem was tracked during procedure with real-time ultrasound guidance.
Tandem was repositioned according to the ultrasound visualization,
i.e.
if short or too advanced,
impinging against anterior or posterior myometrium (Figure 3).
The applicators were removed if perforation was detected and patients were treated conservatively.
The patients were monitored for at least 24 hours and evaluated with pelvic ultrasound for free fluid or hematoma or any other complications.
All patients underwent treatment planning tomography and applicator suitability and complications like perforation were evaluated with tomography.
All planning tomographies were retrospectively reviewed by the radiologist for the optimal tandem placement as well as the uterine characteristics for the study.
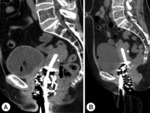
Of the 142 patients,
132 (93%) had anteverted and 10 (7%) had retroverted uterus (Figure 4).
The tandem length was short in two (1.4%) patients,
long in four (2.8%) patients and was in myometrium in three (2.1%) patients before ultrasound guidance (Figure 5).
The uterus was laterally deviated in 76 (53.5%) patients.
No other major complications were seen in our patients.