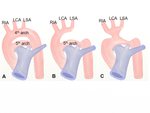
Left aortic arch
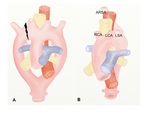
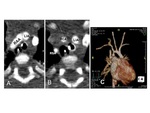
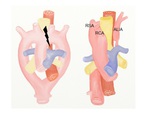
A. Left aortic arch (LAA) with aberrant right subclavian artery (ARSA)
This anomaly is resulted from regression of the right aortic arch between the right common carotid artery (RCCA) and right subclavian artery (RSA) (Fig.
3).
The aberrant right subclavian artery as the last main branch of the aortic arch arises from the descending aorta and goes to the right arm,
passing behind the esophagus (Fig.
4).
It is the most common aortic arch anomaly and reported to occur in 0.5-2% of the population.
Rarely,
symptoms occur if the right-sided ductus arteriosus is present between the ARSA and the right pulmonary artery forming a vascular ring.
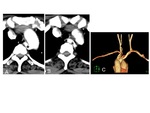
B. Left aortic arch (LAA) and right descending aorta (circumflex aorta)
The distal part of the left aortic arch crosses the midline and passes behind the esophagus and then descends to the right of the spine (Fig.
5).
It is an extremely rare anomaly.
Two anatomic variations based on the origin of the right subclavian artery are: 1) Mirror-image branching; 2) Right subclavian artery arising as the last branching from a diverticulum at the descending aorta.
The chest plain film shows the left-sided aortic knob with the shadow of the descending aorta located at the right side of thoracic spine.
Right aortic arch
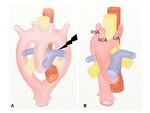
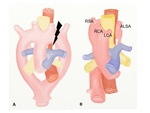
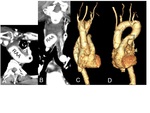
A. Right aortic arch with mirror-image
This anomaly is resulted from regression in the left aortic arch beyond the left subclavian artery (Fig.
6).
Either the left or right sixth aortic arch which becomes the ductus arteriosus may persist.
In this anomaly,
the arch courses to the right of the trachea,
esophagus and passes over the right mainstem bronchus.
The arterial branches of the aortic arch in order are (1) the left brachiocephalic artery,
(2) the right common carotid artery,
(3) the right subclavian artery (Fig.
7).
The proximal descending aorta is located on the right.
It is highly associated with a congenital cardiac disease.
The most common cardiac malformation are tetralogy of Fallot,
persistent truncus arteriosus,
transposition with pulmonary stenosis and ventricular septal defect with infundibular pulmonary stenosis.
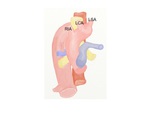
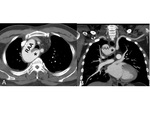
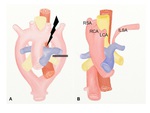
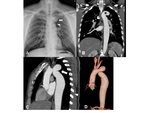
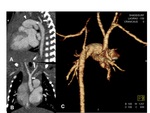
B. Right aortic arch with an aberrant left subclavian artery
This anomaly is resulted from the interruption of a dorsal segment of the left aortic arch between the left common carotid artery (LCCA) and the LSA (Fig.
8).
The left subclavian artery (ALSA) arises as the fourth branch of the aortic arch and passes behind the esophagus to the left arm (Fig.
9).
The ALSA usually arises from the Kommerell's diverticulum,
which is a remnant of the dorsal left aortic arch.
The first branch of the right aortic arch is the LCCA,
followed by the RCCA and RSA.
There may be a ductus arteriosus between the left subclavian artery and left pulmonary artery forming a loose vascular ring,
which cause mild esophageal indentation.
Association with a congenital cardiac malformation is uncommon.
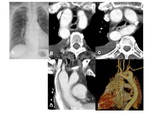
C. Right aortic arch with isolation of the left subclavian artery
This is a rare anomaly with the prevalence rate about 0.8% of patients with right aortic arch.
Isolation of the left subclavian artery (LSA) results from the interruption of a left aortic arch at two locations.
One is between LCCA and LSA,
and the other location is distal to the attachment site of the LDA.
So the isolated LSA is connected with pulmonary artery by the LDA (Fig.
10).
If the LDA is closed,
isolated LSA is supplied by the left vertebral artery and other collaterals such as external carotid arteries and which results in subclavian steal syndrome.
A half of patients have congenital heart disease,
especially TOF.
D. Right aortic arch with an aberrant left innominate artery
This entity is very rare and few cases have been reported in the literature.
The first report was in 1968[1].
The anomaly arises from the interruption of an embryonic left aortic arch between the ascending aorta and the LCCA with regression of the RDA (Fig.
11).
A complete vascular ring is formed by the pulmonary artery anteriorly,
aortic arch on the right,
Kommerell's diverticulum posteriorly,
and the ligamentum arteriosum or ductus arteriosus on the left (Fig.
12).
E. Circumflex retroesophageal right aortic arch
The synonym of this anomaly is right aortic arch with a left descending aorta.
In this anomaly,
the ascending aorta and aortic arch are located on the right side.
The right aortic arch crosses immediately behind the esophagus at the level of 4th~5th thoracic vertebrae after passing over the right bronchus,
and the descending aorta is located on the left side of thoracic vertebrae.
Two anatomic subtypes.
The left subclavian artery may arise from Kommerell's diverticulum or from the left innominate artery.
Double aortic arch
This anomaly is formed by no interruption in the Edward's hypothetical double arch and persistence of bilateral embryologic fourth aortic arches.
One aortic arch lies anterior to the trachea and the other is located posterior to the esophagus (Fig.
13).
Each arch crosses over the ipsilateral bronchus and fuses into a single descending aorta.
Double aortic arches are classified into two types depending on the patency of the two arches: (A) both arches are patent,
(B) one of the arches is atretic.
A.
Complete Double Aortic Arches (Both Arches Patent)
The two complete arches maybe equal in size or one arch may be hypoplastic.
The larger aortic arch is the dominant one,
and the right aortic arch is dominant in 73% of patients.
The left aortic arch is in front of the trachea and the right aortic arch passes behind the esophagus.
The branches of the aortic arch are symmetric.
The RCCA and RSA originate from the right arch and the LCCA and LSA arise from the left aortic arch (Fig.
14) Symptoms are usually present by esophageal or tracheal compression when a tight vascular ring exists.
B. Incomplete double aortic arches (Double aortic arches with atresia of one arch)
When one of the arches is atretic,
it is defined as the incomplete double aortic arch.
Usually,
it presents as the left aortic arch is atretic with fibrous band.
Double aortic arch with right arch atresia is extremely rare.
Cervical aortic arch
In this anomaly,
the apex of the aortic arch is in either the apex of the thoracic cavity or base of the neck (Fig.
15).
This anomaly is very rare with a prevalence of 0.01% of population.
There are many theories to explain the pathogenesis.
The first theory proposes the cervical aortic arch is derived from the third embryonic arch.
The second theory presents lack of caudal migration of the fourth embryonic arch.
However,
some radiologists regard it as “redundant aorta” or “pseudocoarctation”.
The third theory suggests fusion of the third and fourth embryonic arches,
combined with failure of caudal migration.
According to the first theory,
the cervical aorta crosses behind the esophagus and the internal and external carotid arteries arise separately on the same side of the aortic arch.
Therefore the number of brachiocephalic vessels is increased.
In addition,
there is usually an aberrant subclavian artery originating from an aortic diverticulum.
A pulsatile mass in the supraclavicular area is the most common clinical finding.
Chest radiograph shows the aortic knob not in its normal position and a mass lesion at superior mediastinum with tracheal displacement to the opposite side.
Interruption of Aortic Arch
Interrupted aortic arch (IAA) is defined as a complete luminal and anatomic discontinuity between the ascending and descending aorta by Steidele in 1778[2].
IAA is rare,
accounting for only 1% of congenital heart disease[3].
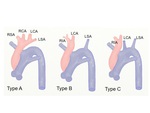
Type A to C of IAA is categorized by the Celoria-Patton classification.
Type A is defined as interruption distal to the left subclavian artery (42% of cases).
In type B,
the interruption is between the left common carotid artery and subclavian artery (53%).
In type C,
the interrupted segment is between the right brachiocephalic artery and left common carotid artery (4%) (Fig.
16-17).
Only VSD and PDA are seen in simple IAA.
The complex IAA is associated with truncus arteriosus,
transposition of the great arteries,
double-outlet right ventricle,
aortopulmonary window,
functional single ventricle,
and obstruction of the left ventricle outflow tract.
DiGeorge syndrome is presented in more than 25% of the complex IAA patients.
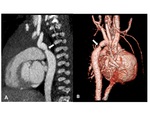
Coarctation of the aorta
This anomaly is defined by proximal aortic narrowing in the region of the ligamentum arteriosum just distal to the left subclavian artery (Fig.
18).
It was described by Morgagni in 1760.
It has a male predominance (male-to-female ratio,
1.5:1)[4].
The previous classification into preductal (infantile) and postductal (adult) is less commonly used because aortic coarctation is always periductal[5].
The key imaging findings are a discrete periductal aortic narrowing and multiple collateral vessels including internal mammary arteries,
intercostal arteries,
and thyrocervical and thoracoacromial trunks with descending scapular arteries,
which finally go into the external iliac arteries and intercostal arteries.
This anomaly should be differentiate from pseudocoarcation,
which has been described as an elongated or redundant aortic arch with "kinking" or “buckling” at the level of the ligamentum arteriosum without a pressure gradient across the lesion.
No rib notching is demonstrated on imaging.
Persistent 5th aortic arch
Normally,
the 5th aortic arch is poorly developed and therefore this entity is extremely rare.
If this 5th aortic arch persists,
it forms a “double-lumen aortic arch”.
The 4th aortic arch goes its normal course and gives rise in normal fashion to the brachiocephalic arteries.
In addition,
another left arch (the persistent 5th aortic arch) connects the ascending and descending aorta (Fig.
19-20).
Identification of a ductus arteriosus is the way to distinguish the second aortic arch not a variant of the 6th aortic arch.
Pulmonary Artery Sling
This anomaly is a subtype of abnormalities of the 6th aortic arch.
The other two types include: (1) patent ductus arteriosus,
(2) proximal interruption of the 6th aortic arch.
In this abnormality,
the left pulmonary artery arises from the right pulmonary artery and passes to the right of the trachea,
above the right mainstem bronchus,
and then between the trachea and esophagus to the left lung.
It probably develops early in embryologic life when the lungs are still a single mass.
Left and right pulmonary arteries form on each side of this single pulmonary mass and contact with the respective 6th aortic arches.
The left pulmonary artery fails to make a connection.
Because the lungs are still a single mass and have a common vascular supply,
the left portion retains a vascular connection with the right portion.
As the lung buds separate,
the left pulmonary artery arises from the right pulmonary artery and passes between trachea and esophagus to left lung (Fig.
21).
It is important because the tracheal rings of neonates are soft,
they are compressed by the left pulmonary artery,
which may lead to obstructive emphysema or atelectasis of the right lung.
If not operated,
the mortality is high.