This poster is published under an
open license. Please read the
disclaimer for further details.
Keywords:
Gastrointestinal tract, Liver, Interventional non-vascular, CT, MR, Percutaneous, Biopsy, Haemangioma, Neoplasia, Cysts
Authors:
M. Maunglay, A. Lukaszewicz, R. Sandhu, R. Muhar, H. Hayes, M. Mirza, B. Vermuri; Pontiac/US
DOI:
10.1594/ecr2016/C-0179
Conclusion
Concordance of radiological imaging interpretation and pathology findings was 100% in cases where the patient underwent prior ultrasound,
PET scan,
contrast-enhanced CT,
MRI or a combination of CT and MRI.
Overall,
63 of 180 benign hepatic lesions were clearly identified as such on imaging alone,
meaning that 35% of biopsies could have been avoided.
Imaging interpretation thereby aids in assisting clinicians in avoiding exposing patients to the risks inherent with direct tissue sampling.
In cases of CT without contrast,
20% of malignant lesions were incorrectly classified as likely being benign. Therefore,
imaging interpretation alone can accurately identify malignant hepatic lesions,
but is less accurate when intravenous contrast is not utilized for CT examinations.

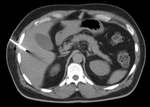
Fig. 3: Axial CT image showing biopsy needle with its tip at the site of a hepatic lesion, which is difficult to visualize, due to the lack of intravenous contrast.
Correct identification of malignant lesions,
and subsequent biopsy,
provides invaluable information on histological subtype,
tumor grade,
receptor and mutation statuses,
all of which are vital to guiding treatment.